Letter to Editor
Time for a New Appraisal of the Management of Thyroid Nodules
Laura Sterian Ward*
Laboratory of Cancer Molecular Genetics Faculty of Medical Sciences, University of Campinas (FCM-Unicamp), Rua Tessalia Vieira de Camargo 126, Barao Geraldo, Campinas, Sao Paulo, Brazil
*Corresponding author: Laura Sterian Ward, Laboratory of Cancer Molecular Genetics Faculty of Medical Sciences, University of Campinas (FCM-Unicamp), Rua Tessalia Vieira de Camargo 126, Barao Geraldo, Campinas, Sao Paulo, Brazil
Published: 18 Aug, 2018
Cite this article as: Ward LS. Time for a New Appraisal of
the Management of Thyroid Nodules.
Clin Oncol. 2018; 3: 1511.
Letter to Editor
Brazilian National Institute of Cancer (INCA) estimates an incidence of 1.570 new thyroid
tumors in males and 8.040 in females for each year of the 2018-2019 biennium, with an appraised
risk of 1.49 and 7.57 cases per 100.000 men and women, respectively [1]. As represented in (Figure
1), thyroid cancer is the fifth most common tumor in women.
The incidence varies considerably among different regions [1]. Well-developed regions, such as
the Southeast, presents 9.75 cases/100 thousand women, in contrast with only 2.80/100 thousand
women from the poorer north part of the country [1]. The remarkable geographic variation and sex
disparity in thyroid cancer rates observed across the regions may reflect differences in ascertainment,
diagnosis, treatment, and death certification of this disease, as well as healthcare access. The same
phenomenon has been observed in other Latina American countries [2]. However, it is north worthy
that mortality rates have declined in Brazil, likewise observed in many other countries, suggesting
there is widespread over diagnosis (detection of tumors that will not cause clinical illness or death)
[3,4].
New detection techniques, in addition to the very sensitive ultrasound equipment largely
available and accessible to the general population at relatively low cost now routinely reveal small
tumors of the prostate, breast, kidney and lung. These diagnoses may raise anxiety not only to
the patient and his family, but also to the physician. The easiest and more practical way to deal
with the situation is often immediate surgery, and, in the case of thyroid tumors, the procedure is
often followed by unnecessary and even harmful radioiodine administration. The burden of such
interventions has dramatically increased in the part years. An increasing number of individuals are
condemned to long-life levothyroxine replacement, not mentioning the individuals that may have
the sequelae of vocal cord paralysis or even hypoparathyroidism.
In fact, recent data from South Korea suggest that the epidemic of thyroid tumors observed in
this country dramatically dropped to before ultrasound screening levels after a group of physicians,
supported by the media, and led a campaign against routine screening for thyroid cancer [5,6].
In fact, the United State Preventive task Force (USPTF) recommends against screening for
thyroid cancer in asymptomatic adults and the American Thyroid Association advice refraining
from biopsying small thyroid nodules [7,8].
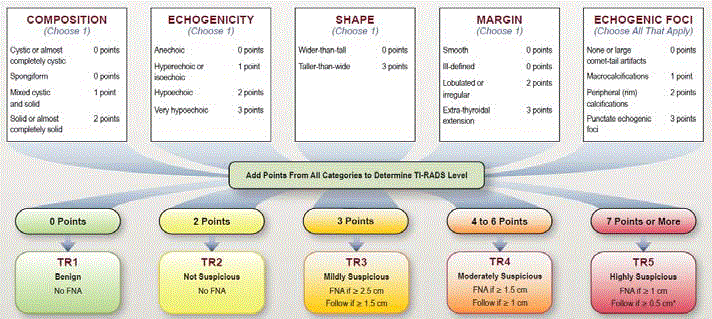
The use of quantitative criteria such as the ones employed in the TI-RADS classification of the
American College of Radiology (Figure 2) may help select better nodules that are suspected [9].
There is an urgent need for a new appraisal of the management of thyroid nodules ant thyroid
tumors. Active surveillance should be considered for thyroid nodules and for papillary cancers. In
addition, it is very important to make clear to the patients that choose
immediate intervention that less aggressive procedures, including
lobectomy over total thyroidectomy, are the more convenient choices.
Figure 1
Figure 2
References
- http://www1.inca.gov.br/estimativa/2018/sintese-de-resultadoscomentarios.asp
- Sierra MS, Soerjomataram I, Forman D. Thyroid cancer burden in Central and South America. Cancer Epidemiol. 2016;44 Suppl 1:S150-7.
- La Vecchia C, Malvezzi M, Bosetti C, Garavello W, Bertuccio P, Levi F, et al. Thyroid cancer mortality and incidence: a global overview. Int J Cancer. 2015;136(9):2187-95.
- Ahn HS, Kim HJ, Welch HG. Korea's thyroid-cancer "epidemic"-- screening and overdiagnosis. N Engl J Med. 2014;371(19):1765-7.
- Ahn HS, Welch HG. South Korea's Thyroid-Cancer "Epidemic"--Turning the Tide. N Engl J Med. 2015;373(24):2389-90.
- Jung KW, Won YJ, Kong HJ, Lee ES. Prediction of Cancer Incidence and Mortality in Korea, 2018. Cancer Res Treat. 2018;50(2):317-23.
- US Preventive Services Task Force, Bibbins-Domingo K, Grossman DC, Curry SJ, Barry MJ, Davidson KW, et al. Screening for Thyroid Cancer: US Preventive Services Task Force Recommendation Statement. JAMA. 2017;317(18):1882-7.
- Haugen BR, Alexander EK, Bible KC, Doherty GM, Mandel SJ, Nikiforov YE, et al. 2015 American Thyroid Association Management Guidelines for Adult Patients with Thyroid Nodules and Differentiated Thyroid Cancer: The American Thyroid Association Guidelines Task Force on Thyroid Nodules and Differentiated Thyroid Cancer. Thyroid. 2016;26(1):1-133.
- Tessler FN, Middleton WD, Grant EG. Thyroid Imaging Reporting and Data System (TI-RADS): A User's Guide. Radiology. 2018;287(1):29-36.