Case Report
Mammary Paget’s Disease: a Rare Case of Early Dermal Invasion
Richard Deane1, Bradley Gluck2, Alan Heimann3, Jun Fan3 and Edna Kapenhas1*
1Department of Surgery, Stony Brook Southampton Hospital, USA
2Department of Radiology, Stony Brook Southampton Hospital, USA
3Department of Pathology, Stony Brook University Hospital, USA
*Corresponding author: Edna Kapenhas, Department of Surgery, Ellen Hermanson Breast Center, Stony Brook Southampton Hospital, Southampton, New York, 11968, USA
Published: 18 Aug, 2018
Cite this article as: Deane R, Gluck B, Heimann A, Fan
J, Kapenhas E. Mammary Paget’s
Disease: a Rare Case of Early Dermal
Invasion. Clin Oncol. 2018; 3: 1510.
Abstract
Introduction: Mammary Paget’s Disease (MPD) is a rare cancer that typically involves an
eczematous lesion of the nipple with underlying intra epidermal cancer. Mammary Paget’s disease
with dermal invasion is an unusual and poorly documented disorder, characterized as Paget disease
that invades through the basement membrane into the dermis.
Presentation: We present a 64 years old female with a 6 months history of left nipple rash. Her
physical exam and subsequent workup was suspicious for Paget’s disease of the left nipple with
Ductal Carcinoma In Situ (DCIS). Punch biopsy confirmed MPD with early dermal invasion, ER/
PR negative, and HER2 positive. A left breast MRI guided biopsy revealed a single duct profile
suspicious for DCIS. She underwent a left central partial mastectomy and subsequently a sentinel
lymph node biopsy.
Discussion: Mammary Paget’s disease is a rare cancer that represents 1% to 3% of breast cancers. The
surgical treatment for Paget’s disease is debatable. Most common form of MPD is intraepidermal
the rare case of dermal invasion has minimal documented cases. Thus, further clinical investigation
and research is required for the surgical treatment for MPD with dermal invasion. The few cases,
including our case with documented Paget’s disease with dermal invasion have been treated with
breast conserving therapy.
Conclusion: We conclude that the management of MPD with dermal invasion requires further
clinical investigation. Our case and the few others explored here reveal that a diagnosis of MPD with
dermal invasion-based on histopathological criteria-can favor conservative operative management
with radiation.
Introduction
Mammary Paget Disease is a rare cancer that typically involves an eczematous lesion of the nipple with underlying intraepidermal cancer. Most cases of Paget’s disease are due to DCIS or invasive carcinoma located deeper in the breast [1]. MPD with dermal invasion is an unusual and poorly documented disorder that is characterized as Paget’s disease with invasive characteristics that invades through the basement membrane into the dermis. Dermal Paget’s cells are unrelated to any underlying DCIS or malignancy. Little data supporting therapeutic indications for MPD with dermal invasion exist. Distinguishing criteria for the difference in surgical management of MPD and MPD with dermal invasion remain unknown.
Case Presentation
64 years old female, with family history of breast cancer in a paternal aunt diagnosed at age 65, presented with a complaint of a left nipple red, dry and scaly rash for 6 months with no response to topical treatment. A mammogram showed no abnormality, with left nipple retraction seen on the CC view only (Figure 1). A diagnostic ultrasound of the left breast was unremarkable. A breast MRI showed asymmetric retraction and enhancement of the left nipple areolar complex with asymmetric smooth linear enhancement extending 2.5 cm from the left nipple, suspicious for Paget’s disease and DCIS (Figure 2). On physical examination, the left breast showed erythematous change of the nipple extending onto the areola laterally, suspicious for Paget’s disease (Figure 3). Punch biopsy of the left nipple revealed MPD with early dermal invasion, ER and PR (-), HER2 (+) (Figure 4). An MRI guided biopsy of the subareolar enhancement revealed DCIS. She underwent a left central partial mastectomy, pathology revealed Paget’s disease of the nipple invading 1 mm into the dermis, and high grade DCIS. A sentinel lymph node biopsy was subsequently performed which revealed benign pathology. She is currently being treated with weekly Paclitaxel with Herceptin for 12 weeks; this will be followed by radiation, which will be delivered during the Herceptin administration every 3 weeks, which will extend to 1 year.
Figure 1
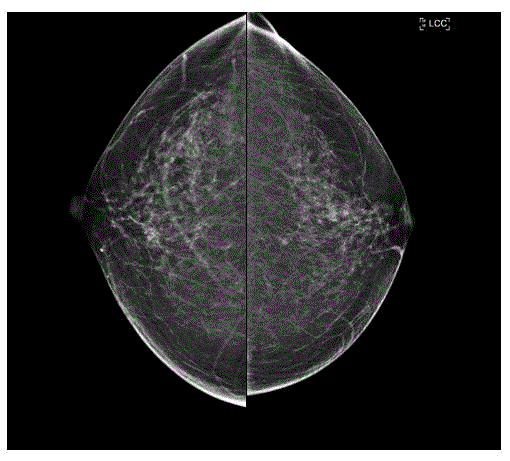
Figure 1
Side by side Cranio-Caudal (CC) mammograms show left nipple
retraction (right image marked LCC), compared to normal right nipple
position (left image).
Figure 2
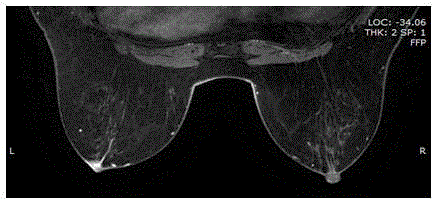
Figure 2
Non-subtracted T1 contrast-enhanced MRI shows asymmetric Left
nipple enhancement and adjacent linear enhancement (breast left side mark
L) consistent with Paget disease with subareolar ductal carcinoma in situ.
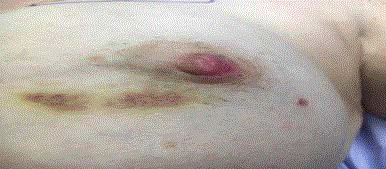
Figure 3
Discussion
Paget’s disease was initially described by Sir Paget in 1874 after
Paget observed 15 women with chronic nipple lesions that progressed
to develop cancer of the involved breast. Thus, Paget’s disease of the
breast, also known as MPD, was viewed as an erythematous, scaly
eczematous lesion of the nipple with underlying breast cancer. Paget’s
disease is a rare entity occurring in 1% to 3% of breast cancers [1].
Mammary Paget’s disease with dermal invasion has been reported in
a selection of female patients 4 times and in 2 male patients in the last
two decades. A study in 2012 revealed that out of 146 patients with
MPD there were 6 who classified as MPD with dermal invasion, a 4%
incidence [2]. The low detection of this entity is most likely due to
the lack of information regarding its clinical relevance. The rare case
presented here will add to the few cases of MPD with dermal invasion
that underwent breast-conserving therapy.
Differentiating underlying breast cancer with invasion to the skin
and PMD with dermal invasion is important to prevent the more
aggressive treatment that is performed on the former. The diagnosis
of dermal invasion in MPD is based on histopathological criteria that
were initially based on extra mammary Paget’s disease, which more
commonly features dermal invasion [3]. Paget cells are characterized
as microscopically large clear cells with an abundant cytoplasm and
hyperchromatic nuclei that is commonly found in the epidermal layer
[1]. The diagnosis for MPD with dermal invasion is pathologically
characterized by the isolated or clustered Paget cells that have invaded
the dermal-epidermal junction. It is important to differentiate
between MPD with dermal invasion and breast cancer invasion to
the skin that is more common and carries a poorer prognosis and
has been documented to present with increased numbers of lymph
node metastases. Invasive MPD (with dermal invasion) is an under
recognized entity, however, with careful pathological analysis; we
can differentiate between these two entities with a vast difference in
prognosis and treatment.
In accordance with the American Joint Committee on Cancer
(AJCC) and Union for International Cancer Control (UICC)
classification, skin invasion from underlying breast cancer carries a
T4b classification. An institutional study in 2012 found 6 patients
with MPD and dermal invasion, which underwent breast conserving
therapy with no evidence of recurrence after an average of 20 months
of follow up [3]. Sanders et al. [4] in 2013 concluded that patients
with MPD with dermal invasion who underwent breast conserving
therapy either with or without sentinel lymph node biopsy did not
need further operative intervention and all sentinel lymph nodes
were negative for malignancy. Those patients underwent radiation
therapy, none received chemotherapy, and after an average of 20
months follow-up showed no evidence of recurrence [4]. On the
other hand, there is one documented case in 2015 of invasive MPD,
HER2 negative, involving axillary metastasis that had undergone
sentinel lymph node biopsy [2,5]. According to the current NCCN
guidelines, adjuvant chemotherapy with weekly Paclitaxel and
Trastuzumab can be considered for T1, N0, M0, and HER2-positive
cancers; particularly if the primary cancer is ER negative.
Overall, MPD with dermal invasion is treated with breast
conserving surgery with or without sentinel lymph node biopsy.
Despite one documented case involving axillary metastasis, most
documented cases were treated with breast conserving therapy
and radiation post-operatively. Whether a sentinel lymph node
biopsy should be performed on all patients with invasive MPD is
unknown. Only one institutional study in 2014 compared invasive
and non-invasive MPD together. It retrospectively compared
survival outcome in invasive MPD and noninvasive MPD and found
no significant difference between the two patient populations with
regard to underlying breast cancer, immunohistochemical stain for
ER or HER2, rate of distant metastasis or recurrence, and treatment
modality. The overall survival and disease-free interval were not
significantly different [6]. Thus treatment for MPD with dermal
invasion should be the same as the treatment for non-invasive
Mammary Paget’s Disease.
Figure 4
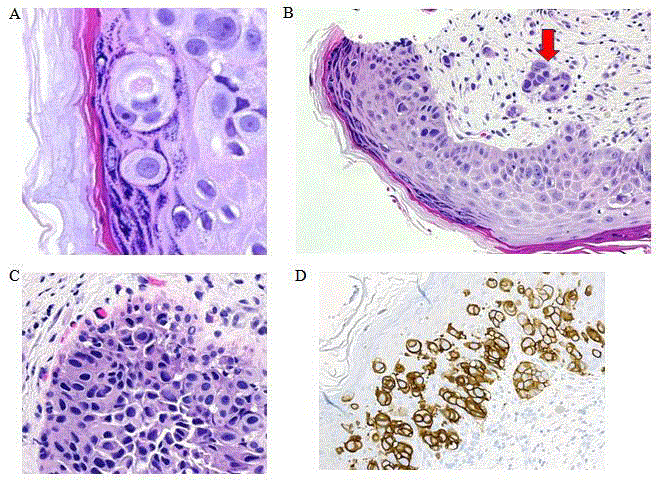
Figure 4
(A) Typical Paget’s cells located in the granular layer of skin 600x.
(B) Mammary Paget’s disease with dermal invasion in the superficial dermis
observed at 200x located at the tip of the arrow. (C) DCIS cells located in the
duct at 400x. (D) (+) HER2 staining in invasive tumor at 200x.
Conclusion
Our case reports a rare finding of MPD with early dermal invasion that was successfully managed with left central partial mastectomy with sentinel lymph node biopsy. Few cases have been reported of Paget’s disease of the breast with dermal invasion and there are no studies outlining the difference in surgical treatment between invasive MPD and non-invasive MPD. The patients in the three studies reported above on this rare form of MPD all underwent breast conserving surgical therapy with no evidence of recurrence on follow up [2-4,6,7]. Distinction between underlying breast cancer invasion of skin and MPD with dermal invasion is critical as the latter exhibits a favorable prognosis. Although prior studies have shown that invasive MPD favor a treatment similar to non-invasive MPD with good response; it remains an under recognized disease. According to the current NCCN guidelines, adjuvant chemotherapy with weekly Paclitaxel and Trastuzumab can be considered for T1, N0, M0, and HER2-positive cancers; particularly if the primary cancer is ER negative. The clinical significance of invasive Paget’s disease of the breast is unknown as all studies have a limited follow up time interval. Further studies are required to dictate its clinical significance and surgical management.
References
- Dubar S, Boukrid M, Bouquet de Joliniere J, Guillou L, Vo QD, Major A, et al. Paget's Breast Disease: A Case Report and Review of the Literature. Front Surg. 2017;4:51.
- Saluja K, Sahoo S. Invasive Paget Disease of the Nipple of Luminal-B Subtype With Axillary Lymph Node Metastasis in a 60-Year-Old White Woman. Lab Med. 2015;46(4):332-7.
- Duan X, Sneige N, Gullett AE, Prieto VG, Resetkova E, Wu Y, et al. Invasive paget disease of the breast: Clinicopathologic study of an underrecognized entity in the breast. Am J Surg Pathol. 2012;36(9):1353-8.
- Sanders MA, Dominici L, Denison C, Golshan M, Wiecorek T, Lester SC. Paget disease of the breast with invasion from nipple skin into the dermis: an unusual type of skin invasion not associated with an adverse outcome. Arch Pathol Lab Med. 2013;137(1):72-6.
- Wolff AC, Hammond ME, Hicks DG, Dowsett M, McShane LM, Allison KH, et al. Recommendations for human epidermal growth factor receptor 2 testing in breast cancer: American Society of Clinical Oncology/College of American Pathologists clinical practice guideline update. J Clin Oncol. 2013;31(31):3997-4013.
- Lee HW, Kim TE, Cho SY, Kim SW, Kil WH, Lee Je, et al. Invasive Paget disease of the breast: 20 years of experience at a single institution. Hum Pathol. 2014;45(12):2480-7.
- Tomoi Sato, Ichiro Muto, Takeshi Oya, Takeshi Sakai. Invasive Paget's disease of the male nipple: A case report. J Surg Case Rep. 2017;2017(7):rjx137.