Clinical Image
Multiple Myeloma Relapse Revealed by a Solitary Skin Plasmocytoma
Filipe Martins and Gregoire Stalder*
Service and Central Laboratory of Hematology, Centre Hospitalier Universitaire Vaudois, Switzerland
*Corresponding author: Gregoire Stalder, Service and Central Laboratory of Hematology, Centre Hospitalier Universitaire Vaudois, CH- 1011 Lausanne, Switzerland
Published: 13 May, 2018
Cite this article as: Martins F, Stalder G. Multiple Myeloma
Relapse Revealed by a Solitary Skin
Plasmocytoma. Clin Oncol. 2018; 3:
1462.
Abstract
We describe an unusual case of early multiple myeloma relapse as a solitary skin plasmocytoma, in a
65-year-old woman in very good partial response (VGPR)* after induction regimen and autologous
stem cell transplantation.
*International Myeloma Working Group (IMWG) 2010 Uniform Response Criteria for Multiple
Myeloma.
Clinical Image
A 65-year-old woman diagnosed with an IgG Lambda multiple myeloma (MM) eight month
earlier attended a follow-up hematologic consultation. She underwent a high-dose melphalan
chemotherapy and autologous stem cell transplantation, after induction regimen with four cycles
of bortezomib, lenalidomide and dexamethasone, five months earlier. She had recently begun a
lenalidomide maintenance therapy. A bone marrow biopsy realized one month prior to consultation
did not show remnant clonal plasma cells. A serum immunosubtraction revealed a slight IgG
Lambda unquantifiable band, together with a normal free light chain ratio. A cytogenetic analysis
revealed the persistence of a complex and hyperploid karyotype including a chromosome 1p gain.
These abnormalities were already present at diagnosis.
At this follow-up consultation, a round 4 cm large mass surrounded by a dense reticular small
vessel net WAS found at clinical exam (Figure 1). A biopsy of the lesion revealed highly proliferative
malignant plasmocytes (MIB-1 staining >95%) with vascular plasma cell thrombi. Immunostaining
for MYC was intensely strong but negative for BRAF. The later was confirmed by RT-PCR. A FISH
analysis did not reveal a MYC rearrangement. PET-CT restaging revealed the described lesion
(SUVmax= 4.6 g/ml) but also a centimetric subcutaneous lesion of the right thigh (SUVmax=1.9 g/
ml) and a lymph node of the left external iliac region (SUVmax=4.4), together with disseminated
highly metabolic bone lesions (SUVmax between 5 g/ml and 6.6 g/ml). The cutaneous lesion was
treated with radiotherapy (10 Gy x 3 Gy) with a good response (Figure 2). Systemic treatment
was then pursued with carfilzomib, lenalidomide and dexamethasone, until a diffuse soft-tissue,
cutaneous and lymph node spread, together with a biological relapse, surged 6 months later.
Extraosseous myeloma (EM) may surge during the disease course in almost one fifth of patients
[1,2]. Its incidence is increasing, due to more extensive radiological staging, extended survival and
suspected selection of more aggressive myeloma cell clones after allogenic stem cell transplant
[3,4]. A shift from intact immunoglobulin towards light chain only secretion is possible [5].
Although several breakthroughs have been made in MM treatment,
this subgroup of patients still carries a poor prognosis [6]. Liver is
the more frequent extraosseous site of disease spread at relapse [7].
Skin involvement is rare in the relapse setting and more prevalent at
diagnosis [7]. Underlying its rarity, a recent literature review gathered
44 published cases of EM involving extremities soft tissues [8].
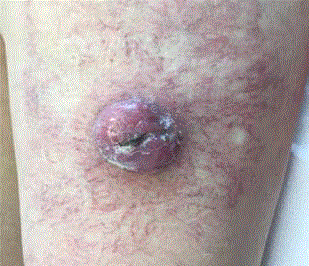
Figure 1
Figure 1
Plasmocytoma of the skin (left thigh). Note the dense reticular vascular bed surrounding the lesion.
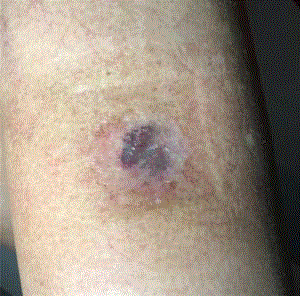
Figure 2
Figure 2
Plasmocytoma of the skin (left thigh), 8 weeks after radiotherapy (10
Gy × 3 Gy) and pursue of systemic treatment with carfilzomib, lenalidomide
and dexamethasone.
References
- Blade J, Fernandez de Larrea C, Rosinol L, Cibeira MT, Jimenez R, Powles R. Soft-tissue plasmacytomas in multiple myeloma: incidence, mechanisms of extramedullary spread, and treatment approach. J Clin Oncol. 2011;29(28):3805-12.
- Varga C, Xie W, Laubach J. Development of extramedullary myeloma in the era of novel agents: no evidence of increased risk with lenalidomidebortezomib combinations. Br J Haematol. 2015;169(6):843-50.
- Varettoni M, Corso A, Pica G, Mangiacavalli S, Pascutto C, Lazzarino M. Incidence, presenting features and outcome of extramedullary disease in multiple myeloma: a longitudinal study on 1003 consecutive patients. Ann Oncol. 2010;21(2):325-30.
- Vincent L, Ceballos P, Plassot C. Factors influencing extramedullary relapse after allogeneic transplantation for multiple myeloma. Blood Cancer J. 2015;5:e341.
- Dawson MA, Patil S, Spencer A. Extramedullary relapse of multiple myeloma associated with a shift in secretion from intact immunoglobulin to light chains. Haematologica. 2007;92(1):143-4.
- Pour L, Sevcikova S, Greslikova H. Soft-tissue extramedullary multiple myeloma prognosis is significantly worse in comparison to bone-related extramedullary relapse. Haematologica. 2014;99(2):360-4.
- Usmani SZ, Heuck C, Mitchell A. Extramedullary disease portends poor prognosis in multiple myeloma and is over-represented in high-risk disease even in the era of novel agents. Haematologica. 2012;97(11):1761- 7.
- Ames J, Al-Samaraee A, Takahashi T. Extraosseous Multiple Myeloma: Case Report of Presentation in the Lower Extremity Soft Tissues with Literature Review. Case Rep Radiol. 2017;2017:9159035.