Case Presentation
Prostate Cancer – Ignorance Isn’t Always Bliss
Gabriel C Ukala1*, Sonia P Reid-Ukala2
1Department of Internal Medicine, Mandeville Regional Hospital & Associate Lecturer, University of the West Indies, Kingston, Jamaica
2Department of Emergency Medicine, Mandeville Regional Hospital and General Practitioner, Jamaica
*Corresponding author: Gabriel C Ukala, Department of Internal Medicine, Mandeville Regional Hospital & Associate Lecturer, University of the West Indies, Kingston, Jamaica
Published: 08 Mar, 2018
Cite this article as: Ukala GC, Reid-Ukala SP. Prostate
Cancer – Ignorance Isn’t Always Bliss.
Clin Oncol. 2018; 3: 1422.
Case Presentation
This 52-year-old high school teacher of African descent (brought into office in a wheelchair),
presented with a two-week history of cramping pain and numbness in the lower chest region, lower
back and both lower limbs. He claimed to have had intermittent low back pain for years due to a
previous back injury. He said the cramping pain and numbness were such that they had begun to
affect his walking in the last four days prior to presentation. He denied any cough, fever, and weight
loss or micturition symptoms. He was, otherwise, not known to have any chronic illness.
His physical examination revealed evidence of dense paraparesis in both lower limbs (power
of grade 1/5 bilaterally) with brisk knee jerk reflexes. He had a single moderately large and mobile
left inguinal lymphadenopathy. Percussion of his vertebral column elicited mild tenderness in the
region of about the 7th to 9th thoracic vertebrae. His digital rectal examination revealed a large, firm,
nodular and craggy prostate gland. Anal sphincter tone was, however, intact.
Further history revealed that he had never had, or sought, a prostate examination before –
neither digital rectal exam nor serum prostatic specific antigen (PSA) test.
A tentative diagnosis of metastatic prostate carcinoma with possible cord compression and
dense paraparesis was considered.
Results of his investigations showed PSA >100 ng/ml (normal range 0-4.0 ng/ml). Urgent
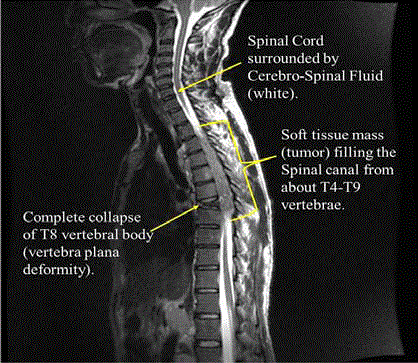
MRI- Scan of his thoraco-lumbar spine showed vertebra plana deformity at T8 due to a pathologic
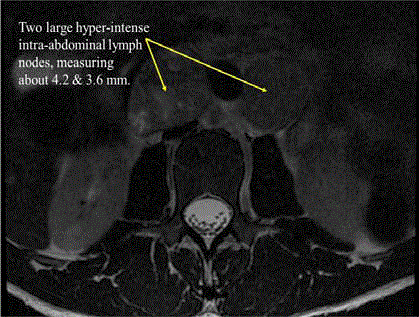
fracture, with greater than 50% decrease in vertebral body height. He also had thoracoabdominal
lymphadenopathies and soft tissue masses infiltrating as well as compressing the spinal canal from
about T4 to T9 vertebrae, suspicious for metastatic disease (Figures 1 & 2). He was immediately
immobilized, given intravenous push of high dose Dexamethasone (40 mg) to stabilize and minimize
neurological deficits, then referred for urgent neurosurgical/orthopedic consult for consideration of
surgical stabilization of the spine. Biopsy of his prostate gland showed undifferentiated prostatic
malignancy, confirming (along with clinical and radiographic findings) stage 4 disease – at
least Gleason 8 or higher. He subsequently had emergency radiation therapy for the spinal cord
compression (followed by further palliative radiation for the metastatic disease). He was then
commenced on a three-monthly androgen suppression therapy along with neuro-rehabilitative
care and followed up by a team of Urologic,Oncology/Radiation-Oncology, Orthopedic and
Neurosurgical specialists.
Discussion
Prostate cancer continues to be a major health problem worldwide with an estimated 1.1 million
cases diagnosed in 2012 [1]. It is the most commonly diagnosed cancer in men. “Men of African
ethnicity are well known to be of high risk for developing prostate cancer” [2]. And in the Caribbean,
specifically Jamaica, it is highly prevalent and the leading cause of cancer-related deaths in men [2].
At least 11.6% of all men will be diagnosed with prostate cancer during their life time, most being
diagnosed between age 55 and 74 (median age of 66) [3,4]. There is evidence that reduced screening
with prostate-specific antigen (PSA) leads to increased incidence of advanced or metastatic disease
[3-6]. While 79% of prostate cancer cases are localized at diagnosis, there is local spread to regional
lymph nodes in 12% and distant metastasis in 5% [3]. Patients with distant metastasis or advanced
disease have 29.8% relative 5-year survival rate compared to 100% in localized or regional disease
[3,4]. The later underscores the need for early screening.
Clinical presentation of metastatic prostate cancer may vary depending on the organs and/
or extent of involvement/sequelae of metastasis. Consequences of metastatic disease include
“anemia, bone marrow suppression, weight loss, pathologic fractures, spinal cord compression,
pain, hematuria, ureteral and/or bladder outlet obstruction, urinary
retention, chronic renal failure, urinary incontinence and other
symptoms related to bony or soft-tissue metastases” [3]. In patients
with pathologic fractures and spinal cord compression (as in this
case), neurologic manifestations may range from numbness and
neuropathic pain in the lower limbs to partial or complete paralysis.
Treatment of advanced metastatic prostate cancer is not
only challenging but can be perplexing and disappointing for
both physician and patient. It often calls for a multidisciplinary
approach requiring therapies ranging, where appropriate, from
external beam radiation therapy, long-term androgen suppression,
neurosurgical and orthopedic intervention in cases with pathologic
fractures complicated by spinal cord compression and other medical
supportive care as needed. Surgical intervention is mandatory for
pathologic fractures involving weight bearing bones and if spinal cord
compression is present, immediate bilateral orchidectomy must also
be considered [3].
Figure 1
Figure 2
Conclusion
The practice of prostate specific antigen (PSA) testing and
subsequent biopsy is becoming more widespread allowing for early
diagnosis, management and possible cure but not all at risk men are
availing themselves of this development. In our experience, most men
are terrified about finding out that they have prostate cancer; some
claim a feeling of being violated by digital rectal examination. As a
result, many men choose not to be screened but being diagnosed with
an advanced disease always proves to be regretfully devastating (as in
this case).
Prostate cancer-related deaths remain more than twice as high
in men of African origin compared to other groups [5]. Also at
diagnosis, it is often at a higher grade in men of African origin with
a more aggressive and progressive course [3,7,8]. More needs to be
done to encourage all men above the age of forty, especially those
with a family history or other significant risk factors (including being
black) to be screened, at least, annually as outcome is directly related
to stage of disease at the time of diagnosis. And since most prostate
cancers are diagnosed by Primary Care Physicians and Internists,
emphasis should be placed on heightened awareness for preventive
screening by these practitioners.
References
- Prostate Cancer Estimated Incidence, Mortality and Prevalence Worldwide in 2012. 2018.
- Belinda F. Morrison, William Aiken, Richard Mayhew, Yulit Gordon, Marvin Reid. Prostate Cancer Screening in Jamaica: Results of the Largest National Screening Clinic. Journal of Cancer Epidemiology. 2018;2016 (2016).
- Martha K Terris, Shaukat M Qureshi, Edward David Kim. Metastatic and Advanced Prostate Cancer, Medscape. Urology. 2018.
- Cancer Stat Facts: Prostate Cancer. National Cancer Institute. 2018.
- Cancer Facts & Figures 2017. American Cancer Society. 2018.
- Weiner AB, Matulewicz RS, Eggener SE, Schaeffer EM. Increasing incidence of metastatic prostate cancer in the United States (2004-2013). Prostate Cancer Prostatic Dis. 2016;19 (4):395-7.
- Fowler JE Jr, Sanders J, Bigler SA, Rigdon J, Kilambi NK, Land SA. Percent free prostate specific antigen and cancer detection in black and white men with total prostate specific antigen 2.5 to 9.9 ng./ml. J Urol. 2000;163(5):1467-70.
- Moul JW, Douglas TH, McCarthy WF, McLeod DG. Black race is an adverse prognostic factor for prostate cancer recurrence following radical prostatectomy in an equal access health care setting. J Urol. 1996;155(5):1667-73.