Research Article
Diagnostic Accuracy of Technetium-99m -Octreotide in Imaging Neuroendocrine, Our Experience with Literature Review
Naima Al Bulushi1*, Badriya Al Saqri1, Marwa Al Amri1, Aymen Al Hadidi2, Hafidh Al Jahdami1, Mohammed Al Zadjali3 and Mimouna Al Risi3
1Royal Hospital, Ministry of Health, Oman
2Oman Medical Specialty Board (OMSB), Oman
3Medical students, College of Medicine, Sultan Qaboos University Hospital, Oman
*Corresponding author: Naima Al Bulushi, Nuclear Medicine Department and Molecular Imaging Centre, Royal Hospital, P.O. BOX 1331, P.C:111 Muscat International Airport, Oman
Published: 24 Oct, 2017
Cite this article as: Al Bulushi N, Al Saqri B, Al Amri M,
Al Hadidi A, Al Jahdami H, Al Zadjali
M, et al. Diagnostic Accuracy of
Technetium-99m -Octreotide in Imaging
Neuroendocrine, Our Experience with
Literature Review. Clin Oncol. 2017; 2:
1361.
Abstract
Purpose: The aim of this observational cross-sectional study with retrospective review of the data is
to evaluate the efficacy of using Technetium-99m - Octreotide in imaging Neuroendocrine tumors
(NETs).
Materials and Methods: A total of 58 patients with Technetium-99m -Octreotide (Tc-99m- OCT)
were identified in our database, from January 2013 until December 2016. 41 patients (age range
of 15-75 year) meet our inclusion criteria namely; histopathology proven neuroendocrine tumors,
Technetium-99m -Octreotide scan, CT, MRI or both done in our institute for correlation.
Results: 23 patients had true positive Tc-99m– OCT scan. In addition to the primary tumors the
Octeriotide scan revealed metastasis in the lung, liver and retroperitoneal lymph nodes. The smallest
lesion detected on Octreotide scan was a 4-mm pulmonary nodule, that was missed on lung window
CT scan. The Tc-99m– OCT had 17 true negative, one false negative and no false positive. The CT
and MRI scans had 18 true positive, 17 true negative, 5 false negative and one false positive. The
overall sensitivity, specificity, accuracy, positive and negative predictive values of Tc-99m– OCT
scan were; 96%, 100%, 97%, 100% and 94% respectively. Whereas those of CT and MRI were; 78%,
94%, 85%, 94% and 77%, respectively.
Conclusion: The overall diagnostic accuracy of Technetium-99m-Octreotide is high. In addition to
the conventional radiological investigations, Tc-99m-OCT scan is a mandate for better and accurate
staging of patients with NETs.
Keywords: Neuroendocrine tumors; Somatostatin; Technetium-99m; Indium-111; Octreotide;
Gallium-68
Introduction
Neuroendocrine tumours (NET) are uncommon type of tumors arising from the epithelial
tissue of the neuroendocrine system [1]. They can be either functioning or non-functioning type
depending on the presence or absence of hormone and peptide secretions from the tumors. There
are about 40-50 cases per million habitants which accounts for 0.5% of all adult cancers [1]. The
NET form 2% – 4% of the adults with Cancer of Unknown Primary (CUP) [2,3]. Identifying the
primary tumor in patients with NETs, is crucial in the management of those patients even in the
advanced stages with metastasis. Studies showed that resecting the primary tumor improves the
quality of life and the overall survival in patients with NET even with metastatic disease [4,5].
As the NETs have increased density of somatostatin receptors (SSTRs), it was possible to
visualize those tumors with radiolabeled somatostatin analogues. The imaging of NETs and other
tumors with positive SSTRs started more than two decades back using Indium-111-DTPA-[DPhe1]-
Octreotide) (In-111-OCT) [6]. However, because the somatostatin analogue is labeled with
Indium-111 this enforced some limitations such as limited availability, high coast, higher radiation
burden to the patient and the overall suboptimal image quality [7]. One and a half decade back
Decristoforo et al. [8] described the development of a Tc-99m-labeled somatostatin analogue [Tyr3-
octreotide (TOC) and hydrazinonicotinic acid (HYNIC)]. In their study, they found that Tc-99m-
TOC had high tumor to back ground ratio and optimal imaging
time, which was done as one-day protocol as appose to the two days’
protocols (4 and 24 hours imaging) for In-111-OCT. with the advent
of PET/CT more positron emitting radiotracers were used to image
the NETs, those include F-18-FDG followed by F-18-FDOPA [9].
However, Ga-68-DOTA-peptide PET/CT was found to be the most
useful in imaging NETs including visualization, initial staging and
detection of relapse [10]. It is also used to select patients who are
likely to benefit from molecular radiotherapy i.e., Peptide Receptor
Radionuclide Therapy (PRRT), which consists of administration
of radio-therapeutic Yttrium-90 (Y-90) or Lutetium-177 (Lu-177)
versions of the same peptides used for imaging of inoperable NET
[10]. However, the latter is not readily available, hence most of
patients with NETs were scanned and operated based on the findings
on multidetector computed tomography (MDCT) and Magnetic
Resonance Imaging (MRI) only.
Table 1
Materials and Method
Patients
We introduce Technetium-99m instead of Indium-111 labeled
Octeriotide in the last quarter of 2012. In our data base, there were
58 patients who had Tc-99m- OCT scans done between January
2013 and December 2016. 41 patients meet our inclusion criteria;
that were histopathology proven somatostatin positive tumors,
biochemical evidence of somatostatin tumors, Technetium-99m
labeled Octreotide scan, CT and MRI. They were 21 males and 20
females with age range of 15-75 years (mean age of 42.7 years) Table
1. The findings on the Tc-99m-OCT scans were correlated lesion by
lesion to the available MDCT and MRI scans.
Patients preparations
The patient should be off somatostatin receptor blocking agents
for 72 hours prior to the study. Occasionally, patients will be studied
on somatostatin agents to assess the degree of suppression of uptake
in a known lesion. In addition, the patients are advised to be on a
liquid diet for two days before the scan with a mild laxative to be
taken the evening before. On the day of the scan the patient should
fast until the end of the first scan, but should be well hydrated. For
breast feeding mothers, they need to stop breast feeding 12 Hrs post
Tc-99m-OCT injection [11].
Preparation Technetium-99m- labeled Octreotide
The Tc-99m-OCT is prepared as per the instructions attached to
the product kit. The Octreotide kit consist of two vials; vial (1) which
contains 20 micrograms of Hynic- Tyr-Octreotide.TFA and vial (2)
which contains 10 microgram (EDDA) as a stabilizing Re-agent.
The preparation starts by placing vial (1) in a suitable lead shielded
container. This is followed by dissolving the content of vial (2) (EDDA)
in 1 ml of saline and shaking it gently. Following that 0.5 ml from vial
(2) (EDDA) is injected to vial (1) Hynic- Tyr-(Octreotide). This step
is followed by gentle shaking to dissolve the content of vial (1). 1ml
of Tc-99m-sodium pertechnetate from the elution, which should be
2200 MBq (59.45 mCi), is injected to vial (1). The reconstituted vial
(1) Hynic- Tyr-(Octreotide) is then placed on the dry heater block
which should is set at 80˚ degree. The vial should be boiled for 20
minutes using a breathing needle. The reconstituted vial is left to cool
down at room temperature for 30 min. The radiopharmaceutical Tc-
99m-Hynic-Tyr-(Octreotide) should be used within 6 hours.
Technetium-99m - Octreotide scan
The dose used for adult patients is 740 MBq (20 mCi) Tc-99m-
Octreotide and the whole body and static images are done at two
and four hours' post radiotracer injection. The whole-body scan is
performed using dual head gamma camera, using image matrix of
256 x 1024 with speed of 8 cm/min and 5 minutes for the each static
image. The SPECT images are performed for the region of interest, as
requested by the nuclear medicine physician, using 128 x 128 matrix,
1.45 zoom and 30 seconds per view for 32 frames.
This study was approved by the Ethics and research committee in
our institution (MESRC-11/2015).
Table 2
Results
Out of the41patients who were included in this study, 23
showed single or multiple Tc-99m-OCT avid lesions. Most of our
patients had either NET, some were known or with strong family
history of multiple neuroendocrine neoplasms (MEN) subtype I
or II. Others had specific type of NET such as carcinoid tumors of
bowel or bronchus, medullary thyroid cancer, islet cell tumors and
pheochromocytoma, (Table 1).
The Tc-99m-OCT showed true positive results in 23 patients,
whereas the CT and MRI showed true positive results in 18 patients.
The Tc-99m-OCT showed one false negative result in a patient with
incidental finding of left retroperitoneal mass, the histopathology
of which was a well differentiated paraganglioma. The CT and MRI
on the other hand showed false positive result in 1 patient with
carcinoid tumor of the appendix and few mesenteric lymph nodes
and the patient was upstaged metastatic disease. The Tc-99m-OCT
scan was performed to confirm the CT findings, but it showed no
uptake in the mesenteric lymph nodes, on 6 months' follow-up CT
scan the mesenteric lymph nodes resolved and the patient remained
disease free after 2 years of follow-up. Also the CT and MRI showed
false negative results in 5 patients, in which the TC-99m-OCT scan
detected metastasis in the bones, lung and retroperitoneal lymph
nodes, resulting in upstaging of those patients. (Table 2).
The Octreotide scan SN, SP, PPV and NPV were 96%, 100%,
100% and 94% respectively. On the other hand, the SN, SP, PPV and
NPV of the CT and MRI were 78%, 94%, 94%, 77% respectively. The
Tc-99m-OCT showed significantly higher sensitivity and negative
predictive value compared to those of CT and MRI. However, the
specificity and positive predictive values of CT and MRI were not
significantly lower than those of Tc-99m-OCT scan.
One of the patients in this cohort was 47 years old female who
is known to have multiple endocrine neoplasia type 1 (MEN 1). She
presented with severe diarrhoea and she was investigated for NET.
The post contract CT scan of the abdomen and pelvis revealed no
abnormality apart for a small, 7 mm, benign looking preduodenal
lymph node. She then had Tc-99m-Octreotide scan which revealed
focal uptake in the preduodenal lymph node and intense uptake in
the proximal small bowel, Figure 1. For further confirmation, the
patient was sent abroad for Gallium-68-DOTA scan which revealed
intense abnormal uptake in the stomach, duodenum, pancreas
and preduodenal lymph node. The patient underwent Whipple’s
procedure and the histopathology report came as multiple gastrinomas
in the stomach, duodenum, pancreas and one preduodenal metastatic
lymph node. In a second patient, who was 72 years old male with
known NET of the colon with single metastasis to the liver, the post
contrast CT scan of chest and abdomen showed the known metastatic
lesion in the liver with a small, 9 mm, mesenteric lymph node of query
significance. The Tc-99m-Octreotide scan showed Octreotide avid
lesion in the liver, focal uptake in the mesenteric lymph node and a
small, 4 mm, Octreotide avid lung nodule that was overlooked in the
CT scan as it was solitary and small, denoting additional metastatic
foci and changing the surgical management in this patient, (Figure 2).
Another patient who was 29 years old female known as MEN1, and
the post contrast CT scan showed pancreatic lesion. The Octreotide
scan upstaged this patient by showing additional foci of Octreotide
avid lesions in the right breast and left distal femur in addition to
the known lesion in the pancreas. Additional examples of Octreotide
scan upstaging the patients was in a 33 years old female, known to
have medullary thyroid cancer. Post contrast CT chest, that was done
as part of the disease surveillance, showed left sided cervical lymph
nodes only. However, the Octreotide scan showed the uptake in the
cervical lymph nodes in addition to focal uptake in the left clavicle.
Reviewing the CT images revealed that there was a destructive lesion
involving the distal aspect of the right clavicle, as this was at the tip of
the field of view, it was overlooked on the CT.
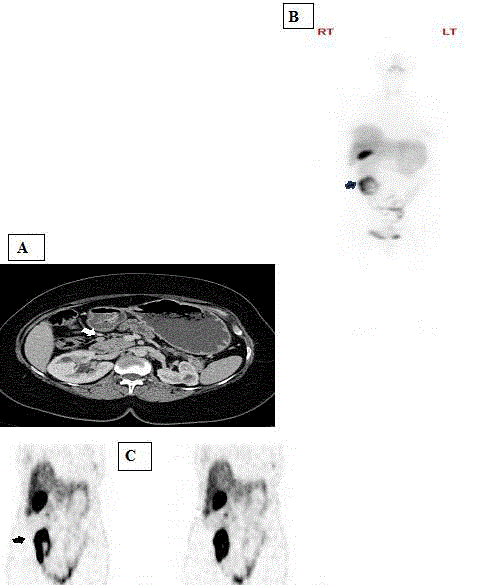
Figure 1
Figure 1
Tc-99m-OCT upstaged this patient with false negative contrast
enhanced CT scan.
Axial post contrast CT scan image in (A) only found a 7 mm preduodenal
lymph node, reported as benign looking (white arrow). Whole body of Tc-
99m-OCT in (B) showed abnormal uptake in the small bowel (black arrow).
Selected coronal images of the Tc-99m-OCT in (C) showed abnormal
radiotracer uptake in the preduodenal lymph node (white arrow) and in the
proximal small bowel (black arrow).
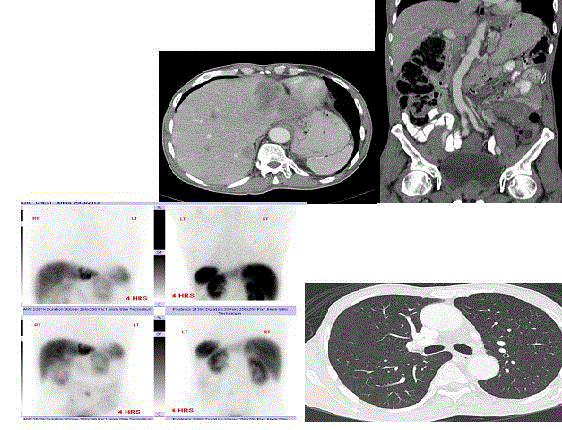
Figure 2
Figure 2
Tc-99m-OCT detected additional pulmonary nodule that was
missed on CT scan. Axial CT scan image in (A) showed the metastatic lesion
in the left liver lobe (white arrow). Coronal CT image in (B) showed the left.
Discussion
Somatostatin is a peptide hormone made of 14 amino acids, it is
normally found in the cerebral cortex, hypothalamus, brain steam,
gastrointestinal tract and in the pancreas [6]. To date there are five
known subtypes of Somatostatin receptors (SSTR)that are expressed
in various levels in NETs, SSTR 2 & 5 are the commonest with their
frequency of expression in the NET ranging from 70% – 90% [12].
Octreotide is the first somatostatin known analogue, it is SST subtype
2 receptor agonists [13,14]. Somatostatin receptor (SSR) imaging is
used for; gastrointestinal and brain tissues evaluation, neuroendocrine
tumors (NET), lung cancer, meningioma and lymphoma. In addition,
it is used prior to Peptide Receptor Radionuclide Therapy (PRRT).
For decades radiolabeled somatostatin analogue, DTPA-[DPhe1]-
Octreotide) was used in imaging NET [6]. However, in our
study, we replaced the traditionally used radioisotope, Indium-111
(In-111) by Technetium 99m (Tc-99m). Using Tc-99m instead of
In-111 solved the issues of availability as the Octreotide is readily
available as a cold kit in our department. Hence, it is labeled with
Tc-99m whenever it’s needed. It is also much cheaper than buying
the In-111-labelled Octreotide and the overall image quality with Tc-
99m is much better than those with In-111. In both Tc-99m&In-111
labeled Octreotide, the spleen is the highest exposed organ (the
critical organ). The estimated absorbed dose of the spleen with Tc-
99m-OCTin mGy/MBq is 0.030 [15] and that of In-111-OCT is 0.665
[16]. The risk-weighted equivalent dose to whole body or “effective
dose” is measured in (mSv/MBq). The effective dose of Tc-99m-OCT
is much less than that of In-111-OCT, 0.0056 [15] and 0.117 [16]
respectively (Table 2). In addition, Gamma Exposure rate at 1 cm
from 1 mCi ofTc-99m is 720 mR/hr and that of In-111 is 3200 mR/h,
i.e. the exposure of the workers form the In-111 is 4.4 times that of
Tc-99m.
When comparing lesion by lesion detected by Tc-99m-OCT to
those detected by MDCT and MRI, the Octreotide study could detect
all lesion except one, which was a well differentiated paraganglioma.
The Sensitivity of Octreotide in detecting NET was higher than that of
MDCT and MRI (96% vs. 78%). The Octreotide showed more lesions
than MDCT and MRI which upstaged the patients and changed the
management.
Reviewing the literature for Tc-99m-OCT, there were very few
papers available and the number of patients in this paper might be
the largest mentioned in the literature so far. In the last decade, many
centers shifted from conventional scintigraphy imaging for NET
using In-111 /Tc-99m labeled Octreotide to PET/CT, particularly
after the advent of Ga-68-DOTA peptides. Studies have shown
the superiority of Ga-68-DOTA peptide PET/CT imaging over
conventional SRS [17]. In a study that included one hundred nine
patients with gastro-entero-pancreatic NETs, Ga-68-DOTA-NOC
PET/CT showed sensitivity and specificity of 78.3% and 92.5%,
respectively, for primary tumor and 97.4% and 100% for metastases.
It was better than a conventional imaging modality for the detection
of both primary tumor (p <0.001) and metastases (p <0.0001). It
changed the management strategy in 21 patients (19%) and supported
management decisions in 32 patients (29%) [18].
Reasons for the preference of using Ga-68-DOTA include easy and
economical synthesis of peptides which does not require a cyclotron
unlike 111In. Another important factor is the less imaging time (2 h for
Ga-68-DOTA peptides, instead of the 4 plus 24 h acquisition for In-
111). When compared to the Tc-99m-OCT, both are imaged within
2 hours, however PET has higher spatial resolution compared to the
single photon emission computed tomography (SPECT) (3 mm - 6
mm versus 10 mm -15 mm). Although in our study the smallest lesion
detected was 4 mm lung nodule, the Tc-99m-OCT missed multiple
small lesions in the stomach and pancreas that were detected by Ga-
68-DOTA PET/CT scan. In addition, DOTA-peptides have higher
and broader affinity for SSTRs compared to Octreotide. Finally, tracer
uptake quantification in the region of interest can be achieved using
PET [17].
Conclusion
In staging and follow-up patients with NETs, Somatostatin
receptor imaging (SSRT) is a mandate for better and accurate staging
as well assessing the avidity of the primary tumor for future follow-up.
In this study, we showed that the sensitivity and negative predictive
values of Tc-99m-OCT scan is significantly higher than that of CT
and MRI.
Using Tc-99m instead of In-111 had several advantages that
include better availability, cheaper and higher quality images. In
addition, to less radiation exposure to both patients and nuclear
medicine personnel. The introduction of PET imaging with 68Ga
and its labelling with DOTA compounds has cleared the way
for somatostatin receptor imaging with a viable PET agent, with
all the advantages compared to single photon imaging. This has
revolutionized the current and future clinical practice for NET [19].
The main limitation of the study is a retrospective data collection and
hence all the patients included were known to have NETs, in addition,
to the small sample size.
References
- Plöckinger U, Rindi G, Arnold R, Eriksson B, Krenning EP, de Herder WW, et al. Guidelines for the diagnosis and treatment of neuroendocrine gastrointestinal tumours: a consensus statement on behalf of the European Neuroendocrine Tumour Society (ENETS). Neuroendocrinology. 2004; 80(6): 394–424.
- Kwekkeboom DJ, Krenning EP, Lebtahi R, Komminoth P, Kos-Kudła B, de Herder WW, et al. ENETS consensus guidelines for the standards of care in neuroendocrine tumors: peptide receptor radionuclide therapy with radiolabeled somatostatin analogs. Neuroendocrinology. 2009; 90(2): 220–226.
- O¨ berg K, Castellano D. Current knowledge on diagnosis and staging of neuroendocrinetumors. Cancer Metastasis Rev. 2011; 30(suppl): 3–7.
- Rothenstein J, Clearly SP, Pond GR, Dale D, Gallinger S, Moore MJ, et al. Neuroendocrine tumors of the gastrointestinal tract: a decade of experience at the Princess Margaret Hospital. Am J Clin Oncol. 2008; 31(1): 64–70.
- Abbruzzese JL, Abbruzzese MC, Lenzi R, Hess KR, Raber MN. Analysis of a diagnostic strategy for patients with suspected tumors of unknown origin. J Clin Oncol. 1995; 13(8): 2094–2103.
- Sandler MP, Coleman RE, Patton JA, et al. Diagnostic Nuclear Medicine. 4th ed. LWW, 2003. P 734.
- Bluma Linkowski Faintuch, Nilda Petrona Sosa Pereira, Solomon Faintuch II, Emiko Muramoto I, Constancia Pagano Gonçalves Silva. Lanreotide and octreotide complexed with technetium-99m: labelling, stability and biodistribution studies. Brazilian Journal of Pharmaceutical Sciences. 2004; 40(1).
- Decristoforo C, Melendez-Alafort L, Sosabowski JK, Mather SJ. 99mTc-HYNIC-[Tyr3]-octreotide for imaging somatostatin-receptor-positive tumors: preclinical evaluation and comparison with 111In-octreotide. J Nucl Med. 2000; 41(6): 1114–1119.
- Imperiale A, Rust E, Gabriel S, Detour J, Goichot B, Duclos B, et al. 18F-Fluorodihydroxyphenylalanine PET/CT in Patients with Neuroendocrine Tumors of Unknown Origin: Relation to Tumor Origin and Differentiation. J Nucl Med 2014; 55(3): 367–372.
- Banerjee SR, Pomper MG. Clinical Applications of Gallium-68. Appl Radiat Isot. 2013; 0: 2–13.
- Stabin MG, Breitz HB. Breast Milk Excretion of Radiopharmaceuticals: Mechanisms, Findings, and Radiation Dosimetry. J Nucl Med. 2000; 41(5): 863-873.
- Papotti M, Bongiovanni M, Volante M, Allìa E, Landolfi S, Helboe L, et al. Expression of somatostatin receptor types 1-5 in 81 cases of gastrointestinal and pancreatic endocrine tumors: a correlative immunohistochemical and reverse-transcriptase polymerase chain reaction analysis. Virchows Arch. 2002; 440: 461–475.
- Schmid HA Schoeffter P. Functional activity of the multiligand analog SOM230 at human recombinant somatostatin receptor subtypes supports its usefulness in neuroendocrine tumors. Neuroendocrinology. 2004; 80 Suppl 1: 47-50.
- Schmid HA. Pasireotide (SOM230), development, mechanism of action and potential applications. Mol. Cell. Endocrinol. 2008; 286(1–2): 69–74.
- Grimes J, Celler A, Birkenfeld B, Shcherbinin S, Listewnik MH, Piwowarska-Bilska H, et al. Patient-Specific Radiation Dosimetry of 99mTc-HYNIC-Tyr3-Octreotide in Neuroendocrine Tumors. J Nucl Med. 2011; 52(9): 1474-1481.
- Krenning EP, Bakker WH, Kooij PP, Breeman WA, Oei HY, de Jong M, et al. Somatostatin Receptor Scintigraphy with Indium-111-DTPA-D-Phe-1-Octreotide in Man: Metabolism, Dosimetry and Comparison with Iodine-123-Try-3-Octreotide. J Nucl Med. 1992; 33(5): 652-658.
- Sharma P, Singh H, Bal C, Kumar R. PET/CT imaging of neuroendocrine tumors with 68Gallium-labeled somatostatin analogues: An overview and single institutional experience from India. Indian J Nucl Med. 2014; 29(1): 2–12.
- Naswa N, Sharma P, Kumar A, Nazar AH, Kumar R, Chumber S, et al. Gallium-68-DOTA-NOC PET/CT of Patients With Gastroenteropancreatic Neuroendocrine Tumors: A Prospective Single-Center Study. AJR Am J Roentgenol. 2011; 197(5): 1221-1228.
- Al-Nahhas A, Win Z, Szyszko T, Singh A, Nanni C, Fanti S, et al. Gallium-68 PET: a new frontier in receptor cancer imaging. Anticancer Res. 2007; 27(6B): 4087-4094.