Case Report
Orbital Myositis Secondary to Cytotoxic T-Lymphocyte-Associated Protein 4 Antibody – A Case Report
Patel D, Tremont A and Fuloria J*
Department of Oncology, Ochnser Health System, USA
*Corresponding author: Fuloria J, Department of Oncology, Ochnser Health System, USA
Published: 30 Nov, 2016
Cite this article as: Patel D, Tremont A, Fuloria J. Orbital
Myositis Secondary to Cytotoxic
T-Lymphocyte-Associated Protein 4
Antibody – A Case Report. Clin Oncol.
2016; 1: 1149.
Abstract
Ipilimumab, a monoclonal antibody targeting cytotoxic T-lymphocyte antigen 4 (CTLA-4) was approved in 2011 for the treatment of metastatic melanoma after a phase 3 study showed an improvement in overall survival. The majority of adverse events related to the drug noted in the study were immune-mediated, causing dermatologic, gastrointestinal and endocrine dysfunction. These side-effects are consistent with the idea that by enhancing a patient’s immunoreactivity there will be increased self reactivity. This report describes a patient with orbital myositis secondary to Ipilimumab.
Case Report
A 39-year-old male was diagnosed with a melanoma, BRAF wild type, of his left cheek. He
underwent a submandibular sentinel lymph node excision [1]. 1 out of 2 removed lymph nodes
were positive for melanoma. He had a left neck dissection that did not show any other evidence of
disease. MRI of the brain was negative. A PET scan was negative for distant disease. He was staged
as a T4aN1M0 lesion. He was started on adjuvant therapy with Ipilimumab at 10 mg/kg given every
21 days [2]. He complained of progressive fatigue and a transient episode of right post auricular
swelling with tenderness after his first infusion. Otherwise, his treatment was tolerated well until
after his fourth cycle. He developed left-sided facial edema with diplopia four days after receiving
his fourth treatment of Ipilimumab. He complained of blurriness with distant vision and double
vision while driving. He also had associated headache and dizziness. Thyroid function tests at this
time were unremarkable.
He was started on oral prednisone, 100 mg daily when he presented with facial edema and
diplopia and had some clinical improvement. A MRI with and without contrast of the brain was
performed that was negative for metastatic disease. Both a slit lamp and a fund us exam were
performed by optometry and were unremarkable. A week later after being instructed to taper
prednisone from 100 mg to 50 mg daily, his symptoms worsened and his prednisone dose had
to be re-escalated to 100 mg daily. In spite of this he presented to the emergency department 10
days later for worsening symptoms. He now had associated photophobia and tearing. His extra ocular movements were limited in every direction of gaze with the left
eye and he had left hypotropia in primary gaze [3]. Prednisone was
increased to 125 mg by mouth daily. MRI with contrast at this time
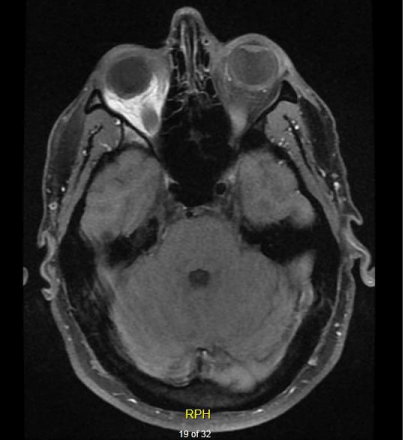
showed subtle heterogeneous edema and enhancement of the extra
ocular muscles bilaterally but most prominent on the left involving the
superior and lateral rectus muscles (Figure 1). He was diagnosed with
orbital myositis. Again, thyroid function test were unremarkable. He
was discharged with some improvement but needed a readmission
for worsening symptoms. Intravenous steroids were now instituted.
Intraocular pressure (IOP) was noted to be elevated with tonometry
and patient was started on timolol and brimonidine eye drops to
both eyes. Elevated intraocular pressure was thought to be secondary
to steroid use. Ophthalmology suggested patching the left eye for
symptom relief.
Figure 1
Figure 1
The patient was switched back to oral prednisone at the time of discharge and this was tapered very
slowly over the next 3 months as his symptoms resolved gradually. He eventually discontinued medications for
elevated IOP and hypertension that were secondary to steroid use.
Discussion
To our knowledge, this is one of the first few clinical reports of orbital myositis as an adverse event related to anti-CTLA-4 antibody treatment [3]. Both timing and usual profile of adverse events support the hypothesis that orbital myositis has to be attributed to ipilimumab. While several dysimmune toxicities have been observed with ipilimumab, ophthalmic toxicity is less common. Most cases described have been of uveitis. Orbital myositis has a unique presentation and should be identified early along with administration of high dose steroids to improve symptoms. Close follow-up is required to monitor intraocular pressure and other side effects related to high dose steroids.
References
- Hodi FS, O Day SJ, McDermott DF, Weber RW, Sosman JA, Haanen JB, et al. Improved survival with ipilimumab in patients with metastatic melanoma. N Engl J Med. 2010; 363: 211–223.
- Robert C, Ghiringhelli F. What is the role of cytotoxic T lymphocyteassociated antigen 4 blockade in patients with metastatic melanoma? Oncologist. 2009; 14: 848-861.
- Lecouflet M, Verschoore M, Giard C, Gohier P, Le Corre Y, Milea D, et al. Orbital myositis associated with ipilimumab. Ann Dermatol Venereol. 2013; 140: 448–451.