Case Report
A Case Report of Paratesticular Rhabdomyosarcoma in an Adolescent
Shazly AR1, Abd M1 and Shazly MU2*
1Urology and Nephrology Center, Menoufia University Hospital, Egypt
2Department of Urology, Menoufia University, Egypt
*Corresponding author: Shazly MU, Department of Urology, Menoufia University, Shibin Al Kom, Menoufia, Egypt
Published: 14 Sep, 2016
Cite this article as: Shazly AR, Abd M, Shazly MU.
A Case Report of Paratesticular
Rhabdomyosarcoma in an Adolescent.
Clin Oncol. 2016; 1: 1094.
Abstract
Rhabdomyosarcoma (RMS) is a malignant tumor of mesenchymal origin typically affects children and adolescents, with an annual incidence of 4.3 cases per 1 million population aged <20 years. Para testicular RMS is rare, constituting 4-7% of all RMS in children and young adults. Here we report a case of 16-year old boy with right paratesticular solid mass. Ultrasound revealed vascular paratesticular mass separated from the testis. Right Inguinal orchiectomy was done. Histopathology revealed embryonal Rhabdomyosarcoma (a plastic variant) infiltrating fascia of the spermatic cord. There was no lymph node infiltration or distant metastasis in further work up.
Introduction
About 30% of all paratesticular neoplasms are malignant. Their real origin is somewhat hard to
determine; however, spermatic cord is the most common site (90%) [1].
Rhabdomyosarcoma (RMS) is one of the commonest paratesticular malignancies [2-4]. RMS
is a malignant tumor thought to arise from cells committed to a skeletal muscle lineage. However,
these tumors can arise in locations where skeletal muscle is not typically found (e.g. the urinary
bladder). Paratesticular localization includes the epididymis or spermatic cord and occurs mostly in
the young people. Paratesticular RMS is extremely rare and has high malignant potential. It spreads
rapidly and thus needs to be diagnosed accurately and to be treated early especially in older patients
that reported to have a worse prognosis [5].
Case Presentation
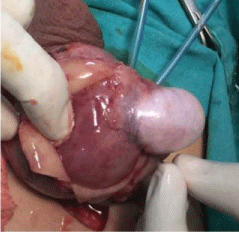
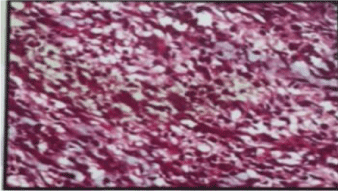
A 16-year old boy presented to urology clinic with right painless paratesticular solid mass measuring about 8 cm in its largest diameter. With no other history of medical importance ultrasound examination revealed solid vascular right paratesticular mass separated from the testis. Tumor markers levels (B-HCG, LDH, alpha feto protein) were within normal. Patient underwent right high inguinal orchiectomy and the specimen was sent for histopathological assessment. Histopathology report revealed embryonal Rhabdomyosarcoma (a plastic variant) (Figure 1 and 2). It was Grade III according to FNCLCC grading system, stage PT2 (tumor larger than 5cm) infiltrating the fascia of the spermatic cord. Thoracoabdominal CT was done as a further work up to search for metastasis and was free. The patient was referred to oncologist and he received chemotherapy.
Figure 1
Figure 2
Discussion
Rhabdomyosarcoma (RMS) is the most common soft tissue
tumor of childhood that typically affects children and adolescents.
Approximately 3 in 4 cases occur in children aged <10 years, with a
peak incidence between ages 3 and 5 years and a second, smaller peak
in adolescence, after which, the incidence drops significantly with
increasing age [6]. Any body part can be affected by RMS. However,
the most common primary sites are the head and neck region (35
to 40%), the genitourinary (GU) tract (25%), and the extremities
(20%) [7-9] approximately 7% of RMS is paratesticular. Clinically
paratesticular tumour presents as a hard painless inguino scrotal
swelling [2,7]. A hydrocele can be occasionally present in adults
explaining the frequent misdiagnosis of paratesticular RMS with
hydrocele in this population [10].
Three major histologic subtypes of RMS are identified:
1. Embryonal (59% of all RMS cases. 50% are of the classic
subtype, and the botryoid and spindle cell variants comprise 6 and
3%, respectively).
2. Alveolar (21%).
3. Undifferentiated sarcoma (20%) [9-11].
Embryonal RMS typically arises in the head and neck region or
in the genitourinary tract although they may occur at any primary
site. They are the most common histologic subtype of paratesticular
RMS [12]. Spindle cell variant is most frequently observed at the
paratesticular site [13]. Spread of the tumor is mostly by lymphatics
to the iliac and paraaortic nodes, but hematogenous spread does
occur most commonly to the lungs and liver [14,15]. In our case, the
patient presented with stage III (no distant metastasis).
Paratesticular sarcomas are rare. There is no standard treatment.
In the localized disease (92% of cases) [16], treatment strategies
include radical high inguinal orchiectomy, retroperitoneal lymph
node dissection, chemotherapy and radiotherapy [17-19]. The
treatment strategy is made according to the clinical condition of the
patient and work up investigations that include physical examination,
chest x-ray, bilateral bone marrow smears and biopsies, abdominal
and chest computed tomography (CT) scan, and bone scan [20]. These
investigations determine tumor staging and presence of metastatic
nodules. RMS is more aggressive in adolescents than children.
Adolescents have less satisfactory outcome than children (late
diagnosis, more lymph node infiltration, more distant metastasis, less
progression free survival) [21]. A better cooperation with pediatric
and adult oncologists is mandatory to improve the treatment of
adolescents with RMS.
Conclusion
Paratesticular Rhabdomyosarcoma is a rare aggressive tumor. Its awareness, early diagnosis, and intervention need to be emphasized since it grows and metastasizes rapidly leading to poor prognosis.
References
- Ries LAG, Harkins D, Krapcho M, et al. SEER Cancer Statistics Review; National Cancer Institute. Bethesda. 2003.
- Agrons GA, Wagner BJ, Lonergan GJ, Dickey GE, Kaufman MS. From the archives of the AFIP. Genitourinary rhabdomyosarcoma in children: Radiologic-pathologic correlation. Radiographics. 1997; 17: 919-937.
- Richie JP, Walsh PC, Retik AB, Vaughan ED, Wein AJ. Neoplasm of testis In: Campbell's Urology. 7th ed. III. Philadelphia: WB Saunders. 1998. 2411–2452.
- Khoubehi B, Mishra V, Ali M, Motiwala H, Karim O. Adult paratesticular tumours. BJU Int. 2002; 90: 707-715.
- Haga K, Kashiwagi A, Nagamori S, Yamashiro K. Adult paratesticular rhabdomyosarcoma. Nat Clin Pract Urol. 2005; 2: 398-402.
- Bisogno G, Compostella A, Ferrari A, Pastore G, Cecchetto G, Garaventa A, et al. Rhabdomyosarcoma in adolescents: a report from the AIEOP Soft Tissue Sarcoma Committee. Cancer. 2012; 118: 821-827.
- Trippitelli A, Rosi P, Selli C, Carini M, Turini D. Rhabdomyosarcoma of spermatic cord in adult. Urology. 1982; 19: 533-535.
- Boudahna L, Benbrahim Z, Amaadour L, Mazouz A, Benhayoune K, Tahiri Y, et al. Para testicular rhabdomyosarcoma in adults: three case reports and review of literature. Pan Afr Med J. 2014; 19: 279.
- Qualman SJ, Coffin CM, Newton WA, Hojo H, Triche TJ, Parham DM, et al. Intergroup Rhabdomyosarcoma Study: update for pathologists. Pediatr Dev Pathol. 1998; 1: 550.
- Hicks J, Flaitz C. Rhabdomyosarcoma of the head and neck in children. Oral Oncol. 2002; 38: 450.
- Holsinger FC, Weeks BH, Hicks MJ. Contemporary concepts in the management of pediatric rhabdomyosarcoma. Curr Opin Otolaryngol Head Neck Surg. 2002; 10: 91.
- Folpe AL, Weiss SW. Paratesticular soft tissue neoplasms. 2000; 17: 307-318.
- Leuschner I. Spindle cell rhabdomyosarcoma: histologic variant of embryonal rhabdomyosarcoma with association to favorable prognosis. Curr Top Pathol. 1995; 89: 261-272.
- Ferrari A, Dileo P, Casanova M, Bertulli R, Meazza C, Gandola L, et al. Rhabdomyosarcoma in adults. A retrospective analysis of 171 patients treated at a single institution. Cancer. 2003; 98: 571-580.
- Elsässer E. Tumors of the epididymis. Recent Results Cancer Res. 1977; 163-175.
- Debruyne FM, Bökkerink JP, de Vries JD. Current concepts in the management of paratesticular rhabdomyosarcoma. Eur Urol. 1985; 11: 289-293.
- Blyth B, Mandell J, Bauer SB, Colodny AH, Grier HE, Weinstein HJ, et al. AB paratesticular Rhabdomyo sarcoma: results of therapy in 18 cases. J Urol. 1990; 144: 1450-1453.
- Panicek DM, Gatsonis C, Rosenthal DI, Seeger LL, Huvos AG, Moore SG, et al. CT and MR imaging in the local staging of primary malignant musculoskeletal neoplasms: Report of the Radiology Diagnostic Oncology Group Radiology. 1997; 202: 237-246.
- Maurer HM, Beltangady M, Gehan EA, Crist W, Hammond D, Hays DM, et al. The Intergroup Rhabdomyosarcoma Study-I. A final report. Cancer. 1988; 61: 209.
- Maurer HM, Gehan EA, Beltangady M, Crist W, Dickman PS, Donaldson SS, et al. The Intergroup Rhabdomyosarcoma Study-II. Cancer. 1993; 71: 1904.
- Crist W, Gehan EA, Ragab AH, Dickman PS, Donaldson SS, Fryer C, et al. The Third Intergroup Rhabdomyosarcoma Study. J Clin Oncol. 1995; 13: 610.