Review Article
Differentiating Pancreatic Cystic Lesions
Garg N1*, Elshikh M1, Rayan J2, Wei P3, Rajaram V1 and Bhosale P1
1Department of Diagnostic Radiology, University of Texas MD Anderson Cancer Center, USA
2Department of Diagnostic Radiology, Baylor College of Medicine, USA
3Department of Diagnostic and Interventional Imaging, University of Texas Medical School, USA
*Corresponding author: Naveen Garg, Department of Diagnostic Radiology, University of Texas MD Anderson Cancer Center, 1400 Pressler Street, Unit Number 1473, Houston, TX 77030, Room Number: FCT15.5017, USA
Published: 12 Sep, 2016
Cite this article as: Garg N, Elshikh M, Rayan J, Wei P,
Rajaram V, Bhosale P. Differentiating
Pancreatic Cystic Lesions. Clin Oncol.
2016; 1: 1088.
Abstract
Pancreatic cystic lesions (PCLs) may represent malignant or premalignant neoplasms and require
diagnostic evaluation. Patient’s demographics and clinical presentation should be considered
when diagnosing PCLs. Radiologically, location, ductal relation, external contour, wall, and septal
enhancement give important clues for each type of lesion. Imaging features that suggest a high
malignancy risk and warrant additional investigation are mural nodules, nearby mass, thick septa,
and a dilated main pancreatic duct. Pseudocysts, intraductal papillary mucinous neoplasms,
mucinous cystic neoplasms, and serous cystadenoma are the most frequently encountered cystic
lesions. Pseudocysts are most likely to follow a history of pancreatitis and have high amylase and
lipase values. Intraductal papillary mucinous neoplasms are usually connected to the pancreatic
duct and are associated with a GNAS mutation. Mucinous cystic neoplasms generally present as
a solitary distal cystic pancreatic lesion in a middle-aged woman and lack ductal communication.
Serous cystadenomas are associated with high vascular endothelial growth factor levels and a VHL
mutation and have a cyst content rich in glycogen. This review describes performance of various
imaging modalities and pathological markers for diagnosing and detecting malignant potential
of PCLs and illustrates typical pathological and radiological features of the most common PCLs,
including primary issues in the differential diagnosis of these lesions.
Highlights
• Patient demographics should be considered when diagnosing cystic lesions.
• Imaging is crucial for assessment of PCLs, by detecting the locularity, nodularity, external
contour, and enhancement characteristics.
• EUS-FNA can aid in diagnosis of indeterminate cystic lesions on imaging.
Keywords: Intraductal papillary mucinous neoplasm; Mucinous cystic neoplasm; Pancreatic
cystic lesions; Pancreatic pseudocyst; Serous cystadenoma
Introduction
PCLs represent a medical dilemma due to their heterogeneous disease processes and outcomes.
Recently, these lesions have been increasingly detected incidentally due to advances in crosssectional
imaging. Disease prevalence ranges from 2.4% to 24.3%, with a positive correlation with
age [1-6]. Approximately 1% to 3.5% of PCLs are malignant [7,8]. Treatment options vary greatly,
from observation to radical surgery, and depend on the malignant potential of the detected lesion.
Malignant potential relies on the histological subtype, with the highest risk in mucinous PCLs [9].
PCLs can be divided into three groups: (1) benign lesions, (2) cystic lesions with malignant
potential, and (3) cystic malignant tumors [10]. The benign group includes pseudocysts, serous
cystadenomas (SCAs), infectious cysts, retention cyst, Lymphoepithelial cysts, and congenital cysts
[10,11]. Cystic lesions with malignant potential include intraductal papillary mucinous neoplasms
(IPMNs), mucinous cystic neoplasms (MCNs), cystic pancreatic neuroendocrine neoplasms, and
solid pseudopapillary neoplasms (SPN) [10,12]. Cystic malignant tumors are those tumors which
are solid and undergo cystic degeneration such as cystic ductal adenocarcinoma and acinar cancers
[10]. Among the various PCLs, pseudocysts, SCAs, MCNs, and IPMNs are the most frequently
encountered [7,12,13]. To determine the PCL type, there is a need to integrate clinical, radiological,
and pathologic assessments. In this review, we summarize performance of various imaging
modalities and pathological markers in diagnosing and detecting malignant potential of PCLs and
then discuss each of the most clinically encountered PCLs individually.
The Imaging of PCLs
Radiologically, the lesion’s location, ductal relation, internal
content, external contour, wall, and septal enhancement provide
important clues for its diagnosis. Imaging features that suggest a
high malignancy risk and warrant additional investigations are mural
nodules, associated mass, thick septa, and dilated main pancreatic
duct [8,14].
CT is the most frequently used cross-sectional modality for
PCL assessment despite having an accuracy ranging from 20% to
90% [15]. Studies have shown that while CT is less sensitive than
MRI, there is no statistically significant difference between CT and
MRI in characterizing PCL features [8]. Visser et al. [16] reported
an accuracy of 57% for both CT and MRI in PCL-specific subtype
categorization. When combined together, MDCT and MRI have the
highest accuracy in PCLs characterization and 94.5% sensitivity in
malignancy detection [17].
Endoscopic ultrasonography (EUS) provides excellent tissue
resolution due to close proximity to the pancreas. Kim et al. [18]
documented no statistically significant difference between EUS and
MRI in characterizing features of PCLs, even though EUS was less
sensitive and less accurate than MRI. Del Chiaro et al. [19] reported
no stastical difference between EUS-FNA, CT, and MRI concerning
errors in PCLs diagnosis. Adimoolam et al. [20] reported that
EUS was superior at detecting PCL multifocality; the multifocality
detection rate was 47% for EUS vs. 13% for CT (P< 0.0001) and 58%
for EUS vs. 34% for MRI (P=0.0002). EUS also has the advantage of
offering interventional techniques, including cystic fluid sampling
and drainage.
PET CT can be used to determine the malignant potential of
PCLs. Kauhanen et al. [21] compared MRI and CT with PET CT, and
PET CT showed a statistically significant higher sensitivity, specificity,
positive predictive value, negative predictive value, and accuracy in
detecting malignant PCLs. With a SUV max cutoff of 3.6, PET CT
had a sensitivity and specificity of 100% and 88% in detection of
malignancy, respectively. Further, within a study population, PET CT
changed the treatment plan in 5 patients [21]. In a meta-analysis, PET
CT was found to have a sensitivity range of 57% to 94%, a specificity
range of 65% to 97%, and an accuracy of 94% in malignant or
premalignant PCL categorization. In comparison, the sensitivity and
specificity range was 36.3% to 71.4% and 63.9% to 100%, respectively,
for CT, and 91.4% to 100% and 89.7%, respectively for MRI [22].
Pathological Features
Multiple cystic fluid pathological parameters can be used
to categorize the lesions, including fluid amylase, lipase,
carcinoembryonic antigen (CEA), cancer antigen (CA)-125,
mucin content, cytology, DNA content, and detection of genetic
mutations. To date, CEA is the most reliable pathological marker
in discriminating between mucinous and non mucinous PCLs.
Brugge et al. [23] reported that a CEA value ≥192 ng/mL indicates a
mucinous lesion [21]. CEA showed a sensitivity and specificity of 73%
and 84%, respectively, in categorizing PCLs [23,24]. When combined
with CEA, cystic fluid mucin (MUC) content analysis can add to the
diagnostic accuracy [25]. Mucins are membrane bound or secretory
glycoproteins. MUC1 is overexpressed in pancreatic adenocarcinoma,
while MUC6 is characteristic of serous cysts [26-28]. Jabbar et al. [29]
reported that cystic fluid mucin profiling performed better than both
cytology and CEA in diagnosing PCLs. Proteomic mucin profiling
has a sensitivity, specificity, and accuracy of 97.3%, 97.6%, and 97.5%,
respectively, in determining PCLs’ malignant potential. Cysts with
MUC5A, MUC2, and MUC1 overexpression have the highest risk of
being premalignant or malignant [29].
Molecular analysis of the cystic fluid may provide a specific tool
for detecting malignant cysts. Winner et al. [30] documented that
the presence of the K-ras mutation and >2 loss of heterozygosity
was 96.2% specific for malignant cysts. On the other hand, both of
these parameters were less sensitive than CEA in discriminating
between mucinous and non mucinous cysts. A combination of
these parameters with CEA is better at differentiation [30]. Micro
RNA expression is a promising tool for categorization of different
PCLs. Micro RNAs-noncoding RNA molecules that control mRNA
processing-are expressed differently in various PCLs [31].
Pancreatic Pseudocyst
Pancreatic pseudocysts are purely benign lesions [10,12,32-34]
and are the most frequently encountered PCL in clinical practice.
They are not true cysts, but a collection of inflammatory debris
surrounded by a false wall of granulation tissue that develops 4
weeks after pancreatitis onset [35]. Pseudocyst represents a local
complication of interstitial edematous pancreatitis [35]. After acute
pancreatitis, 5% to 16% of patients are at risk of having a pancreatic
pseudocyst, while 20% to 40% are at risk after chronic pancreatitis
[36]. Clinically, patients with pseudocysts may be asymptomatic;
may present with abdominal pain, early satiety, weight loss, may have
complications of infection, rupture, biliary obstruction, or gastric
outlet obstruction [33]. In most instances, pseudocysts are located in
the peripancreatic region or within the pancreas, but rarely occur in
other organs such as the liver, spleen, or mediastinum [12,35,37,38].
Microscopically, a pseudocyst is characterized by absent epithelial
lining and hyper-cellularity in the surrounding stroma. Cyst content
is variable according to cyst stage [39]. The fluid aspirate of pancreatic
pseudocysts is characterized by high amylase and lipase and low CEA
and CA 125 values [33].
Management strategies differ according to the pseudocyst’s
duration, size, location, and relation to the pancreatic duct.
Pseudocysts <5 cm that do not persist for more than 6 weeks may
resolve spontaneously. Pseudocysts which communicate with
the main pancreatic duct and are located in the uncinate process,
head, body, or neck of the pancreas are candidates for endoscopic
transpapillary drainage by ERCP. If no ductal communication is
present, pseudocysts can be managed by internal drainage, whether
surgically or through an endoscopic transmural approach. The
endoscopic transmural approach is feasible if the pseudocyst is <1cm
from or plugging through an adjacent gastrointestinal hollow organ.
Pancreatic tail pseudocysts are the least accessible by ERCP; they are
managed surgically or via transmural endoscopic internal drainage
if they are <1 cm away from a hollow organ [36,40]. Percutaneous
drainage can be done in immature or infected cysts [36].
On ultrasonography, a pseudocyst usually appears as a welldefined,
unilocular, anechoic cyst with distal enhancement. Increased
internal echogenicity is noted if the pseudocyst is detected early
or is complicated with infection or hemorrhage [33]. On CT, the
pseudocyst usually appears as a unilocular hypodense cystic lesion
surrounded by a smooth dense wall that shows contrast enhancement
(Figure 1 and 2). Cystic fluid may show areas of increased attenuation
if complicated [13,32,36,41]. Usually, the pancreatic pseudocyst is
associated with radiological evidence of chronic or acute pancreatitis,
such as necrotic pancreas, duct dilatation, fibrotic parenchyma, ductal
stone, or calcifications [13,14]. CT attenuation can differentiate
between pancreatic pseudocyst and mucinous cystic lesions. Chalian
et al. reported that pseudocyst has a higher attenuation than mucinous
cystic lesions. 14.5 HU cutoff had a sensitvity and specificity of 74.4%,
71.9%, respectively in discriminating between both lesions [42].
On MRI T2-weighted images, it often appears as a hyperintense,
unilocular cyst with a thick enhancing wall [43]. Presence of internal
debris and absence of lobulated surface and calcification differentiate
pseudocyst from other pancreatic cystic lesions [44]. Internal debris
or clotting may resemble a mural nodule; post-contrast enhancement
distinguishes mural nodules [12]. Location, ductal communication,
and relation to other gastrointestinal organs should be reported, as
they affect the management plan.
Figure 1
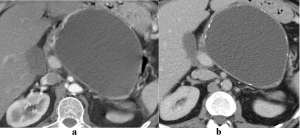
Figure 1
Pseudocyst.40-year-old man who presented with intermittent
epigastric pain, with moderate alcohol intake and no documented history of
pancreatitis. Contrast-enhanced axial CT images of the abdomen on (a)
arterial and (b) portal-venous phases show a cystic mass in the pancreatic
tail with a thick wall and calcifications. This was proven to be a pseudocyst.
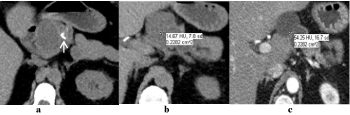
Figure 2
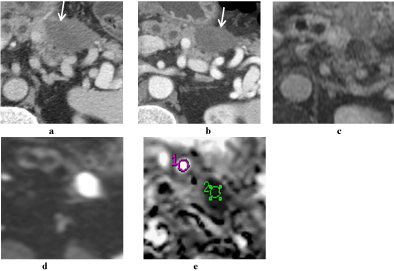
Figure 2
Pseudocyst.60-year-old man with a history of main duct intraductal
papillary mucinous neoplasm who developed pancreatitis following
endoscopic ultrasonography for biopsy. Contrast-enhanced axial CT images
of the pancreas obtained on follow-up; (a) 5 months, (b) 9 months after biopsy
for the neoplasm showed an evolving pseudocyst (arrows). Gadoliniumenhanced
axial MR images of the pancreas obtained 13-monthsafter biopsy
shows (c) a T1-hypointense non-enhancing lesion (d) with increased signal
on DWI and (e) corresponding low signal intensity on the ADC map. Note the
opposite signal characteristics of the nearby pancreatic duct.
Intraductal Papillary Mucinous Neoplasm
IPMN is caused by hyperplasia of the mucinous epithelium lining
the pancreatic ducts, forming papillae and cystic ductal dilatation
[39]. IPMN is categorized as a main duct, branch duct, or mixed type.
Malignancy risk is highest in the main duct group at 62.2%, compared
with 57.4% for the mixed group and 24.4% for the branch duct group
[45]. Based on degree of dysplasia, the World Health Organization
classifies IPMN as low or intermediate-grade, high-grade, or
associated with invasive carcinoma [32]. IPMN is the most common
incidentally detected PCL (50%) [46,47].
Histologically, IPMN is classified as gastric (null cell-type),
intestinal, pancreatobiliary, and oncocytic; the gastric and intestinal
subtypes are the most frequently encountered [48-50]. Subtypes are
differentiated not only morphologically, but also by expression of
different types of mucin glycoproteins (Table 1). The gastric subtype,
which is described as intraductal papillary mucinous adenoma, is
negative for both MUC1 and MUC2 (null subtype). It is the least
likely IPMN to develop invasive malignancy and usually has a smaller
cyst diameter than other subtypes [48,51,52]. On the other hand,
pancreatobiliary IPMN is usually MUC1 positive, which may explain
its aggressive behavior, as MUC1 is linked to pancreatic ductal
adenocarcinoma.
On progression to invasive malignancy, IPMN can give rise to
colloid, tubular, or oncocytic carcinomas. Intestinal IPMNs are
more likely to develop the less aggressive colloid carcinoma. The
pancreatobiliary subtype frequently develops invasive tubular ductal
adenocarcinoma. Despite being the most indolent IPMN, the gastric
subtype usually gives rise to the most invasive tubular adenocarcinoma.
Oncocytic carcinoma classically is preceded by oncocytic IPMN
[46,53]. The prognosis and survival of IPMN associated with invasive
carcinoma are generally better than those of pancreatic ductal
adenocarcinoma. Mino-Kenudson et al. [55] reported a higher 5-year
survival rate in IPMN associated with invasive carcinoma (47%) than
in pancreatic ductal adenocarcinoma (34%) [48]. DPC4 is a tumor
suppressor gene that was found to be expressed in all IPMNs, even
in IPMN associated with invasive carcinoma; but was downregulated
in 55% of pancreatic ductal adenocarcinoma. Persistent expression
of DPC4 in IPMN associated with invasive carcinoma may explain
its indolent biological behavior in comparison to pancreatic ductal
adenocarcinoma [54].
Malignancy detection remains the challenging point in IPMN
management. Histological subtype and relation to pancreatic duct can
predict the IPMN’s malignant potential. Gastric IPMN usually arises
as branch duct type IPMN with benign behavior in most instances,
while other types frequently affect the main pancreatic duct and have
a higher incidence of malignancy. Even risk of malignant conversion
is higher in intestinal IPMN than gastric IPMN when both are related
to a branch duct [48,53]. Clinically, this pattern of biological behavior
is reflected in disease outcome and prognosis. Hisaka et al. [48]
documented 5-year survival rates of 91%, 75%, and 17% in gastric,
intestinal, and pancreatobiliary IPMNs, respectively.
As in all mucinous PCLs, IPMNs’ cystic fluid usually shows a CEA
>192 ng/dL (Table 2). Differences in CEA have been reported between
different IPMN histological subtypes, with the highest mean in gastric
IPMN and the lowest in the oncocytic subtype [55]. Fluid DNA
analysis may give clues to malignant risk. K-ras and GNAS mutations
have been associated with a higher malignancy incidence [56]. TP53
mutations are useful molecular marker for intermediate and high
grade IPMN. TP53 mutations were reported in 17.8% and 38.1% of
intermediate and high grade IPMNs respectively. In low grade IPMN
no TP53 mutations were described [57]. Clinically, IPMN is more
common in men than women, with a higher incidence in the sixth
and seventh decades. Despite having a lower incidence rate than men,
women are more prone to have the aggressive pancreatobiliary IPMN
[49]. IPMN may be multifocal in 20% to 30% of patients [31,32].
Radiologically, ductal relation is a key radiographic feature
for IPMN. Main duct IPMN is identified when there is segmental
or diffuse main pancreatic duct dilation>5 mm without any
obstruction (Figure 3) [13,58-60]. BD-IPMN typically presents as a
unilocular or multilocular cystic mass connected to the pancreatic
duct, although absent ductal communication does not exclude
BD-IMPN [13,60]. MR cholangiopancreatography (MRCP) and
secretin-enhanced MRCP showed better performance in detecting
ductal relation [61]. BD-IPMN may be multifocal (Figure 4 and
5).Without ductal communication, multilocular BD-IPMN may be
misinterpreted as serous cystadenoma (SCA) or MCN, especially
in the absence of salient imaging features of those lesions (Table 3)
[7]. Considering demographics, cystic fluid analysis, enhancement
pattern, calcifications and tumor location (Table 2 and 3) may help to
discriminate between multilocular BD-IPM, MCN, and SCA. Mixed
IPMN carries features of both main duct and branch duct IPMNs
[60]. On EUS mucin is seen extruding through the duodenal papilla
and is considered as a characteristic feature of IPMN [12].
IPMN and MCN management is guided to a great extent
by radiological interpretation. In 2012, international consensus
was reached for management of IPMN and MCN relying on risk
stratification according to certain radiographical findings (cyst and
main pancreatic duct diameter, associated mass, wall enhancement,
and lymphadenopathy). According to the 2012 consensus guidelines,
asymptomatic PCLs with a diameter <1 cm are less likely to harbor
malignancy. A high-risk stigmata has been characterized for high-risk
mucinous lesions consisting of a main pancreatic duct diameter >10
mm without obstruction, obstructive jaundice, and the presence of
an enhancing solid mass. In the presence of these high-risk stigmata,
surgical resection should be deemed without any further workup.
Other worrisome features have been identified for further risk
determination, including cyst diameter ≥3 cm, main duct diameter
of 5 to 9mm, a non-enhancing mass, an enhancing wall, a sudden
main duct diameter change with distal pancreatic atrophy, and
lymphadenopathy. If any worrisome feature is detected, diagnostic
EUS is the next step. Once the feature is confirmed, surgical resection
is the best management modality. In the absence of high-risk stigmata
and worrisome features, follow-up imaging is performed at certain
intervals according to cyst size [45].
Table 1
Table 1
Expression of mucin glycoproteins in histological subtypes of intraductal
papillary mucinous neoplasm.
Table 2
Table 2
Summary of clinical and pathological differences between the most frequently encountered PCLs.
Figure 3
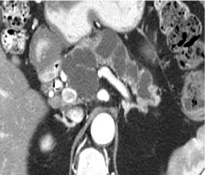
Figure 3
Main duct intraductal papillary mucinous neoplasm (MD-IPMN).75-
year-old woman presented with obstructive jaundice. Axial contrast enhanced
CT shows dilated main pancreatic duct with no evident obstruction. This was
proven to be malignant IPMN on pathological assessment.
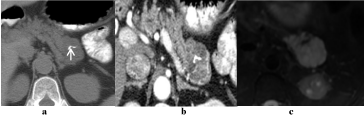
Figure 4
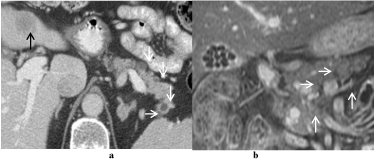
Figure 4
Branch duct intraductal papillary mucinous neoplasm (BDIPMN).
75-year-old woman complaining of abdominal pain, was found to
have multiple hypodense pancreatic lesion without ductal dilatation on (a)
portal-venous axial contract enhanced CT (white arrows) with a hypodense
metastatic lesion in the left hepatic lobe (black arrow) from pancreatic
adenocarcinoma associated with BD-IPMN. (b)Coronal FIESTA MRI shows
multifocal hyperintense lesions (arrows). Her carcinoembryonic antigen level
was 25 ng/dL.
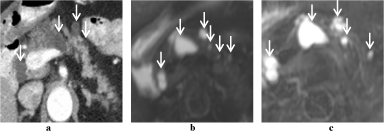
Figure 5
Figure 5
Branch duct intraductal papillary mucinous neoplasm (BD-IPMN).
59-year-old woman with incidentally discovered multifocal branch duct IPMN.
(a) Contrast-enhanced axial CT of the abdomen shows multifocal hypodense
lesions within the pancreas (arrows), which are more conspicuous on MRI,
with a greater number of lesions seen (arrows) on (b) DWI, and (c) T2
sequences.
Table 3
Mucinous Cystic Neoplasms
MCNs represent 10% of clinically encountered PCLs [20,62,63].
The classic presentation of MCN is a solitary distal cystic pancreatic
lesion in a middle-aged woman. MCNs, unlike IPMNs, are solitary
and usually lack ductal communication, especially branch duct
IPMNs. Nevertheless, MCN ductal communication has been
documented in 15% of MCN patients. Grossly, MCNs may be
unilocular or multilocular cystic lesions surrounded by a fibrous
capsule. Microscopically, they are differentiated from other PCLs
by the presence of ovarian stroma. Also, MCNs have been found to
express estrogen, progesterone, α-inhibin, and β-human chorionic
gonadotropin receptors [64]. Multiple theories have been suggested
for the pathogenesis of pancreatic MCN, including metaplasia and
ectopic ovarian tissue implantation in the pancreas. These theories
can be supported by finding the same lesions in other anatomical
sites, such as the liver and retroperitoneum [62].
The malignant conversion risk for MCN is about 13.4%to 30.8%,
with a higher incidence in older patients; most MCNs progress to
tubular ductal adenocarcinoma. Malignant MCNs usually express
MUC1 glycoprotein, while benign MCNs express MUC2 and CDX2
[65-67]. In two reports, MCN patients were found to have other
tumors, especially breast carcinoma, with a prevalence of 6.5% in
one study and 1.9% in another [68,69]. High cystic fluid CA19-9, CA
125, and CA 72-4 can be useful markers in discriminating between
malignant and benign MCN [63,66]. Also, progesterone receptor
(PR) expression was found to be negatively correlated to MCN grade.
The higher MCN grade, the lower is the PR expression [66].
Radiologically, MCN appears as a unilocular or multilocular mass
in the distal pancreas with no ductal communication in most instances
(Figure 6 and 7). On MRI, MCN has high signal intensity on T2 series
(Figure 7) and usually low signal on T1. Nevertheless, MCN signal
intensity may vary according to internal content (mucin, hemorrhage
or debris) [12,32,70,71]. With contrast, MCN often shows peripheral
enhancement (88%) and may exhibit septal enhancement (38%)
[70]. MCN may display peripheral calcifications, mural or septal
nodules or papillary projections [12,32,71]. Differentiation between
MCN and pseudocyst, BD-IPMN, and macrocystic SCA is a tedious
task (Table 3). A smooth outer surface, peripheral enhancement,
and peripheral calcifications can help distinguish MCN from
macrocystic SCA (lobulated outer surface, septal enhancement, and
central calcification) [32,71]. When present with BD-IPMN, ductal
communication distinguishes BD-IPMN from MCN. A history of
pancreatitis is characteristic for pseudocyst [12,71]. Nevertheless,
pathological assessment remains the last resort for discrimination
between indeterminate lesions. Certain radiological findings have
been found to predict a higher malignancy risk. Procacci et al. [67]
reported that an MCN would be 95% likely to be malignant if there
were thick septations, a thick wall, and mural or septal calcification.
If only two of these features were found, the MCN would carry a
malignancy risk of 56% to 74%. They also documented that patient
age and lesion diameter did not correlate with malignancy. On the
other hand, other reports documented that malignant potential of
MCN correlates with cyst size and presence of mural nodules [66,69].
Le Baleur et al. [72] reported that a diameter cutoff of 4 cm is 100%
sensitive and 54% specific in MCN malignancy risk identification.
MCNs with a diameter >4 cm are more likely to be malignant [58]. In
the same study, mural nodules were 100% sensitive and 98% specific
for malignant MCN. Two other studies documented a statistically
higher diameter mean in malignant vs. benign MCN [66,69].
Surgical resection of an MCN is recommended unless patients have
comorbidities [45,63].
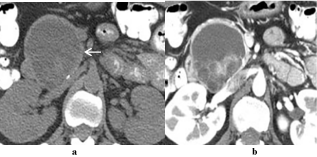
Figure 6
Figure 6
Mucinous cystic neoplasm (MCN).44-year-old woman complained
of postprandial epigastric pain. (a) Precontrast CT show a multilocular (white
arrow) pancreatic head mass with (b) evident post contrast wall and septations
enhancement and no evident ductal communication. Pathologically, the
lesion was proven to be a low-grade mucinous cystic neoplasm.
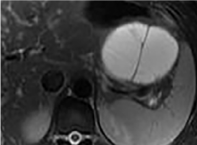
Figure 7
Figure 7
Mucinous cystic neoplasm (MCN). T2-weighted MRI of a 34-yearold
woman with an incidentally discovered pancreatic tail cystic lesion
showed a hyperintense multilocular pancreatic cystic lesion with evident
septations. Pathologically, it was proven to be mucinous cystic neoplasm
with intestinal metaplasia.
Figure 8
Figure 8
Serous cystadenoma(SCA). 65 year old woman with incidentally
detected microcytic SCA.(a) Pre-contrast CT shows pancreatic tail cystic
lesion with central scar (white arrow)which demonstrate (b) septal contrast
enhancement, cyst size less than 1 cm, and has(c) a high signal intensity on
T2 weighted MRI.
Serous Cystadenoma
SCA is a benign cystic lesion that affects women more than
men (at a 3:1 ratio) and is more likely to affect the distal pancreas.
Malignant conversion is extremely rare. Around 16% of PCLs are
SCAs [73]. SCA is a clear cell tumor type that grossly presents as
a large cystic lesion, formed of multiple small cysts with a central
stellate scar. Microscopically, SCA is a glycogen-rich cyst lined with
cuboidal cells that have a clear cytoplasm and round homogenous
nuclei with a hypercapillarized stroma. Due to high glycogen content,
SCA stains positive on Periodic acid-Schiff stain. In 40% of SCA cases,
Von Hippel-Lindau (VHL) gene mutations have been described,
which lead to overexpression of hypoxia-inducible factors. Increased
hypoxia-inducible factors result in overproduction of VEGF and
glucose transporter 1. SCA cystic fluid typically has a low CEA and
CA19-9 and a high VEGF-A (>8500 pg/mL) and VEGF-C (>200 pg/
mL). Elevated VEGF is 100% specific and 97% sensitive for SCA.
VHL-associated SCA is usually multifocal. Despite being serous,
MUC glycoproteins have been documented in SCA (MUC6, 70%;
MUC2, 34%; MUC1, 5%) [74-76].
Two variants of SCA have been identified: microcytic and
macrocytic (oligocytic). Microcytic is the most common form (70%).
It is a well-circumscribed lesion comprising multiple (>6) small cysts
<2 cm in diameter, giving a honeycomb appearance (Figure 8). The
macrocytic variant comprises larger cysts >2cm with less outlines
demarcation than the microcytic variant and may be unicystic (Figure
9) [74,75]. On MRI, SCA appears hyperintense on T2 weighted
images and usually hypointense on T1-WI and commonly shows
post-contrast septal enhancement in 67% of lesions [70]. Typical
imaging features of SCA that distinguish it from other PCL include;
Microcytic morphology, surface lobulations, central scar, and dense
septal enhancement (Table 3) [12,77]. Microcytic pattern presents
in 70% of SCA and has a specificity of 97.8% alone for diagnosing
SCA and 100% in presence of surface lobulations. Despite high
specificity (100%) for SCA, central scar presents only in 30% of SCA.
Central scar may show calcifications [77]. Macrocystic SCAs have
large cysts and may be unilocular resembling MCN. The presence of
surface lobulations, septal enhancement, central scar, and absence
of peripheral enhancement favors diagnosis of SCA, but cystic fluid
aspiration may be needed for definitive differentiation [12,70,78].
Wall thickness was documented to be larger in MCN compared to
SCA. Manfredi et al reported a statistically significant difference in
median wall thickness between MCN (4 mm) and SCA (2 mm) [70].
Management of SCA varies according to symptoms and size.
Since most cases are benign, watchful follow-up is a good choice
for management. For symptomatic lesions or those >4 cm, surgical
resection might be considered [12,74].
Figure 9
Figure 9
Serous cystadenoma(SCA). 65 year old woman with incidentally
detected microcytic SCA.(a) Pre-contrast CT shows pancreatic tail cystic
lesion with central scar (white arrow)which demonstrate (b) septal contrast
enhancement, cyst size less than 1 cm, and has(c) a high signal intensity on
T2 weighted MRI.
Conclusion
PCLs are a heterogeneous group of diseases. Imaging is crucial for assessment of PCLs, by assessing the locularity, nodularity, ductal relation, calcification and enhancement characteristics. EUS-FNA can aid in diagnosis of indeterminate cystic lesions. To improve the accuracy of diagnosis, radiologists should give careful attention to patient history and cystic fluid pathology.
References
- de Jong K, Nio CY, Hermans JJ, Dijkgraaf MG, Gouma DJ, van Eijck Ch, et al. High prevalence of pancreatic cysts detected by screening magnetic resonance imaging examinations. Clin Gastroenterol Hepatol. 2010; 8: 806-811.
- Kimura W, Nagai H, Kuroda A, Muto T, Esaki Y. Analysis of small cystic lesions of the pancreas. Int J Pancreatol. 1995; 18: 197-206.
- Laffan TA, Horton KM, Klein AP, Berlanstein B, Siegelman SS, Kawamoto S, et al. Prevalence of unsuspected pancreatic cysts on MDCT. AJR Am J Roentgenol. 2008; 191: 802-807.
- Lee KS, Sekhar A, Rofsky NM, Pedrosa I. Prevalence of incidental pancreatic cysts in the adult population on MR imaging. Am J Gastroenterol. 2010; 105: 2079-2084.
- Spinelli KS, Fromwiller TE, Daniel RA, Kiely JM, Nakeeb A, Komorowski RA, et al. Pitt HA Cystic pancreatic neoplasms: observe or operate. Annals of surgery. 2004; 239: 651.
- Zhang XM, Mitchell DG, Dohke M, Holland GA, Parker L, Parker. Pancreatic Cysts: Depiction on Single-Shot Fast Spin-Echo MR Images 1. Radiology. 2002; 223: 547-553.
- Di Cataldo A, Palmucci S, Latino R, Trombatore C, Cappello G, Amico A, et al. Cystic pancreatic tumors: should we resect all of them? Eur Rev Med Pharmacol Sci. 2014; 18: 16-23.
- Sainani NI, Saokar A, Deshpande V, Fernández-del Castillo C, Hahn P, Sahani DV. Comparative performance of MDCT and MRI with MR cholangiopancreatography in characterizing small pancreatic cysts. AJR Am J Roentgenol. 2009; 193: 722-731.
- Clores MJ, Thosani A, Buscaglia. JMMultidisciplinary diagnostic and therapeutic approaches to pancreatic cystic lesions. J Multidiscip Healthc. 2014; 7: 81-91.
- Basturk O, I Coban, NV Adsay. Pancreatic Cysts: Pathologic Classification, Differential Diagnosis, and Clinical Implications. Archives of Pathology & Laboratory Medicine. 2009; 133: 423-438.
- Tseng JF, Warshaw AL, Sahani DV, Lauwers GY, Rattner DW, Fernandez-del Castillo C. Serous Cystadenoma of the Pancreas: Tumor Growth Rates and Recommendations for Treatment. Ann Surg. 2005; 242: 413-421.
- Barral M, Soyer P, Dohan A, Laurent V, Hoeffel C, Fishman EK, et al. Magnetic resonance imaging of cystic pancreatic lesions in adults: an update in current diagnostic features and management. Abdom Imaging. 2014; 39: 48-65.
- Sahani DV, Kadavigere R, Saokar A, Fernandez-del Castillo C, Brugge WR, Hahn PF. Cystic pancreatic lesions: a simple imaging-based classification system for guiding management. Radiographics. 2005; 25: 1471-1484.
- Brugge WR. The Incidental Pancreatic Cyst on Abdominal Computerized Tomography Imaging: Diagnosis and Management. Clinical Gastroenterology and Hepatology. 2008; 6: 140-144.
- Ng DZ, Goh BK, Tham EH, Young SM, Ooi LL. Cystic neoplasms of the pancreas: current diagnostic modalities and management. Ann Acad Med Singapore. 2009; 38: 251-259.
- Visser BC, Yeh BM, Qayyum A, Way LW, McCulloch CE, Coakley FV. Characterization of cystic pancreatic masses: relative accuracy of CT and MRI. AJR Am J Roentgenol. 2007; 189: 648-656.
- Jang DK, Song BJ, Ryu JK, Chung KH, Lee BS, Park JK, et al. Preoperative Diagnosis of Pancreatic Cystic Lesions: The Accuracy of Endoscopic Ultrasound and Cross-Sectional Imaging. Pancreas. 2015; 44: 1329-1333.
- Kim YC, JY Choi, YE Chung, S Bang, MJ Kim, MS Park. Comparison of MRI and Endoscopic Ultrasound in the Characterization of Pancreatic Cystic Lesions. American Journal of Roentgenology. 2010; 195: 947-952.
- Del Chiaro M, Segersvärd R, Pozzi Mucelli R, Rangelova E, Kartalis N, Ansorge C, et al. Comparison of preoperative conference-based diagnosis with histology of cystic tumors of the pancreas. Ann Surg Oncol. 2014; 21: 1539-1544.
- Adimoolam V, Sanchez MJ, Siddiqui UD, Yu S, Dzuira JD, Padda MS, et al. Aslanian HREndoscopic ultrasound identifies synchronous pancreas cystic lesions not seen on initial cross-sectional imaging. Pancreas. 2011; 40: 1070-1072.
- Kauhanen S, Rinta-Kiikka I, Kemppainen J, Grönroos J, Kajander S, Seppänen M, et al. Ovaska J Accuracy of 18F-FDG PET/CT, Multidetector CT, and MR Imaging in the Diagnosis of Pancreatic Cysts: A Prospective Single-Center Study. J Nucl Med. 2015; 56: 1163-1168.
- Jones MJ, AS Buchanan, CP Neal, AR Dennison, MS Metcalfe, G Garcea. Imaging of indeterminate pancreatic cystic lesions: a systematic review. Pancreatology. 2013; 13: 436-442.
- Brugge WR, Lewandrowski K, Lee-Lewandrowski E, Centeno BA, Szydlo T, Regan S, et al. Diagnosis of pancreatic cystic neoplasms: a report of the cooperative pancreatic cyst study. Gastroenterology. 2004; 126: 1330-1336.
- Nagula S, Kennedy T, Schattner MA, Brennan MF, Gerdes H, Markowitz AJ, et al. Evaluation of cyst fluid CEA analysis in the diagnosis of mucinous cysts of the pancreas. J Gastrointest Surg. 2010; 14: 1997-2003.
- Utomo WK, Braat H, Bruno MJ, van Eijck CH, Groot Koerkamp B, Krak NC, et al. Cytopathological Analysis of Cyst Fluid Enhances Diagnostic Accuracy of Mucinous Pancreatic Cystic Neoplasms. Medicine (Baltimore). 2015; 94: e988.
- Qu CF, Li Y, Song YJ, Rizvi SM, Raja C, Zhang D, et al. MUC1 expression in primary and metastatic pancreatic cancer cells for in vitro treatment by (213)Bi-C595 radioimmunoconjugate. Br J Cancer. 2004; 91: 2086-2093.
- Teresa L, Tinder, Durai B, Subramani, Gargi D, Basu. Judy M. Bradley,1 Jorge Schettini,1 Arefayene Million,2 Todd Skaar,2 and Pinku Mukherjeecorresponding author1 MUC1 enhances tumor progression and contributes toward immunosuppression in a mouse model of spontaneous pancreatic adenocarcinoma. J Immunol. 2008; 181: 3116-3125.
- Kosmahl M, Wagner J, Peters K, Sipos B, Klöppel G. Serous cystic neoplasms of the pancreas: an immunohistochemical analysis revealing alpha-inhibin, neuron-specific enolase, and MUC6 as new markers. Am J Surg Pathol. 2004; 28: 339-346.
- Jabbar KS, Verbeke C, Hyltander AG, Sjövall H, Hansson GC, Sadik R. Proteomic mucin profiling for the identification of cystic precursors of pancreatic cancer. J Natl Cancer Inst. 2014; 106: djt439.
- Winner M, Sethi A, Poneros JM, Stavropoulos SN, Francisco P, Lightdale CJ, et al. The role of molecular analysis in the diagnosis and surveillance of pancreatic cystic neoplasms. Jop. 2015; 16: 143-149.
- Lee LS, Szafranska-Schwarzbach AE, Wylie D, Doyle LA, Bellizzi AM, Kadiyala V, et al. Investigating MicroRNA Expression Profiles in Pancreatic Cystic Neoplasms. Clin Transl Gastroenterol. 2014; 5: e47.
- Brugge WR, Diagnosis and management of cystic lesions of the pancreas. J Gastrointest Oncol. 2015; 6: 375-388.
- Habashi S, PV Draganov, Pancreatic pseudocyst. World J Gastroenterol. 2009; 15: 38-47.
- Volkan Adsay N, Cystic lesions of the pancreas. Mod Pathol. 2007; 20: S71-93.
- Foster BR, KK Jensen, G Bakis, AM Shaaban, FV Coakley. Revised Atlanta Classification for Acute Pancreatitis: A Pictorial Essay. Radiographics. 2016; 36: 675-687.
- Aghdassi A, J Mayerle, M Kraft, AW Sielenkämper, CD Heidecke, MM Lerch. Diagnosis and treatment of pancreatic pseudocysts in chronic pancreatitis. Pancreas. 2008; 36: 105-112.
- Karamouzos V, Karavias D, Siagris D, Kalogeropoulou C, Kosmopoulou F, Gogos C, et al. Pancreatic mediastinal pseudocyst presenting as a posterior mediastinal mass with recurrent pleural effusions: a case report and review of the literature. J Med Case Rep. 2015; 9: 110.
- Guesmi F, Zoghlami A, Saidi Y, Najeh N, Dziri C. Pancreatic pseudocysts located in the liver: a systematic review of the literature. Tunis Med. 2009; 87: 801-804.
- Adsay NV. Cystic lesions of the pancreas. Modern Pathology. 2007; 20: S71-S93.
- Pan G, Wan MH, Xie KL, Li W, Hu WM, Liu XB, et al. Classification and Management of Pancreatic Pseudocysts. Medicine (Baltimore). 2015; 94: e960.
- Kim YH, Saini S, Sahani D, Hahn PF, Mueller PR, Auh YH. Auh, Imaging diagnosis of cystic pancreatic lesions: pseudocyst versus nonpseudocyst. Radiographics. 2005; 25: 671-685.
- Chalian H, Töre HG, Miller FH, Yaghmai V. CT attenuation of unilocular pancreatic cystic lesions to differentiate pseudocysts from mucin-containing cysts. Jop. 2011; 12: 384-388.
- Kalb B, JM Sarmiento, DA Kooby, NV Adsay, DR Martin, MR imaging of cystic lesions of the pancreas. Radiographics. 2009; 29: 1749-1765.
- Macari M, Finn ME, Bennett GL, Cho KC, Newman E, Hajdu CH, et al. Differentiating pancreatic cystic neoplasms from pancreatic pseudocysts at MR imaging: value of perceived internal debris. Radiology. 2009; 251: 77-84.
- Tanaka M, Fernández-del Castillo C, Adsay V, Chari S, Falconi M, Jang JY, et al. International Association of Pancreatology.International consensus guidelines 2012 for the management of IPMN and MCN of the pancreas. Pancreatology. 2012; 12: 183-197.
- Sahora K, C Fernandez-del Castillo. Intraductal papillary mucinous neoplasms. Curr Opin Gastroenterol. 2015; 31: 424-429.
- Machado NO, H Al Qadhi, K Al Wahibi. Intraductal Papillary Mucinous Neoplasm of Pancreas. N Am J Med Sci. 2015; 7: 160-175.
- Hisaka T, Horiuchi H, Uchida S, Ishikawa H, Kawahara R, Kawashima Y, et al. Potential usefulness of mucin immunohistochemical staining of preoperative pancreatic biopsy or juice cytology specimens in the determination of treatment strategies for intraductal papillary mucinous neoplasm. Oncol Rep. 2013; 30: 2035-2041.
- Furukawa T, Hatori T, Fujita I, Yamamoto M, Kobayashi M, Ohike N, et al. Shimizu M Prognostic relevance of morphological types of intraductal papillary mucinous neoplasms of the pancreas. Gut. 2011; 60: 509-516.
- Mohri D, Asaoka Y, Ijichi H, Miyabayashi K, Kudo Y, Seto M, et al. Different subtypes of intraductal papillary mucinous neoplasm in the pancreas have distinct pathways to pancreatic cancer progression. J Gastroenterol. 2012; 47: 203-213.
- Adsay NV, Merati K, Basturk O, Iacobuzio-Donahue C, Levi E, Cheng JD, et al. Pathologically and biologically distinct types of epithelium in intraductal papillary mucinous neoplasms: delineation of an "intestinal" pathway of carcinogenesis in the pancreas. Am J Surg Pathol. 2004; 28: 839-848.
- Furukawa T, Klöppel G, Volkan Adsay N, Albores-Saavedra J, Fukushima N, Horii A, et al. Classification of types of intraductal papillary-mucinous neoplasm of the pancreas: a consensus study. Virchows Arch. 2005; 447: 794-799.
- Mino-Kenudson M, Fernández-del Castillo C, Baba Y, Valsangkar NP, Liss AS, Hsu M, et al. Prognosis of invasive intraductal papillary mucinous neoplasm depends on histological and precursor epithelial subtypes. Gut. 2011; 60: 1712-1720.
- Iacobuzio-Donahue CA, Klimstra DS, Adsay NV, Wilentz RE, Argani P, Sohn TA, et al. Dpc-4 protein is expressed in virtually all human intraductal papillary mucinous neoplasms of the pancreas: comparison with conventional ductal adenocarcinomas. Am J Pathol. 2000; 157: 755-761.
- Yoon WJ, Daglilar ES, Mino-Kenudson M, Morales-Oyarvide V, Pitman MB, Brugge WR, et al. Characterization of epithelial subtypes of intraductal papillary mucinous neoplasm of the pancreas with endoscopic ultrasound and cyst fluid analysis. Endoscopy. 2014; 46: 1071-1077.
- Wu J, Matthaei H, Maitra A, Dal Molin M, Wood LD, Eshleman JR, et al. Papadopoulos N, Hruban RH, Vogelstein B. Recurrent GNAS mutations define an unexpected pathway for pancreatic cyst development. Sci Transl Med. 2011; 3: 92ra66.
- Kanda M, Sadakari Y, Borges M, Topazian M, Farrell J, Syngal S, et al. Goggins M Mutant TP53 in duodenal samples of pancreatic juice from patients with pancreatic cancer or high-grade dysplasia. Clin Gastroenterol Hepatol. 2013; 11: 719-730.
- Chandwani R, PJ Allen. Cystic Neoplasms of the Pancreas. Annu Rev Med. 2016; 67: 45-57.
- Kang HJ, Lee JM, Joo I, Hur BY, Jeon JH, Jang JY, et al. Assessment of Malignant Potential in Intraductal Papillary Mucinous Neoplasms of the Pancreas: Comparison between Multidetector CT and MR Imaging with MR Cholangiopancreatography. Radiology. 2016; 279: 128-139.
- Stark A, TR Donahue, HA Reber, OJ Hines. Pancreatic Cyst Disease: A Review. Jama. 2016; 315: 1882-1893.
- Rastegar N, Matteoni-Athayde LG, Eng J, Takahashi N, Tamm EP, Mortele KJ, et al. Incremental value of secretin-enhanced magnetic resonance cholangiopancreatography in detecting ductal communication in a population with high prevalence of small pancreatic cysts. Eur J Radiol. 2015; 84: 575-580.
- Farrell JJ. Prevalence, Diagnosis and Management of Pancreatic Cystic Neoplasms: Current Status and Future Directions. Gut Liver. 2015; 9: 571-589.
- Barral M, Soyer P, Dohan A, Laurent V, Hoeffel C, Fishman EK, et al. Magnetic resonance imaging of cystic pancreatic lesions in adults: an update in current diagnostic features and management. Abdominal imaging. 2014; 39: 48-65.
- Izumo A, Yamaguchi K, Eguchi T, Nishiyama K, Yamamoto H, Yonemasu H, et al. Tsuneyoshi MMucinous cystic tumor of the pancreas: immunohistochemical assessment of "ovarian-type stroma". Oncol Rep. 2003; 10: 515-525.
- Baker ML, Seeley ES, Pai R, Suriawinata AA, Mino-Kenudson M, Zamboni G, et al. Invasive mucinous cystic neoplasms of the pancreas. Exp Mol Pathol. 2012; 93: 345-349.
- Jang KT, Park SM, Basturk O, Bagci P, Bandyopadhyay S, Stelow EB, et al. Clinicopathologic Characteristics of 29 Invasive Carcinomas Arising in 178 Pancreatic Mucinous Cystic Neoplasms With Ovarian-type Stroma: Implications for Management and Prognosis. Am J Surg Pathol. 2015; 39: 179-187.
- Procacci C, Carbognin G, Accordini S, Biasiutti C, Guarise A, Lombardo F, et al. CT features of malignant mucinous cystic tumors of the pancreas. Eur Radiol. 2001; 11: 1626-1630.
- Yamao K, Yanagisawa A, Takahashi K, Kimura W, Doi R, Fukushima N, et al. Tanaka M Clinicopathological features and prognosis of mucinous cystic neoplasm with ovarian-type stroma: a multi-institutional study of the Japan pancreas society. Pancreas. 2011; 40: 67-71.
- Crippa S, Salvia R, Warshaw AL, Domínguez I, Bassi C, Falconi M, et al. Castillo CF Mucinous cystic neoplasm of the pancreas is not an aggressive entity: lessons from 163 resected patients. Ann Surg. 2008; 247: 571-579.
- Manfredi R, Ventriglia A, Mantovani W, Mehrabi S, Boninsegna E, Zamboni G, et al. Mucinous cystic neoplasms and serous cystadenomas arising in the body-tail of the pancreas: MR imaging characterization. Eur Radiol. 2015; 25: 940-949.
- Palmucci S, Cappello G, Trombatore C, Tilocca C, Todaro R, Mauro LA, et al. Cystic pancreatic neoplasms: diagnosis and management emphasizing their imaging features. Eur Rev Med Pharmacol Sci. 2014; 18: 1259-1268.
- Le Baleur Y, Couvelard A, Vullierme MP, Sauvanet A, Hammel P, Rebours V, et al. Mucinous cystic neoplasms of the pancreas: definition of preoperative imaging criteria for high-risk lesions. Pancreatology. 2011; 11: 495-499.
- Kim TS, Fernandez-del Castillo C. Diagnosis and Management of Pancreatic Cystic Neoplasms. Hematol Oncol Clin North Am. 2015; 29: 655-674.
- Reid, Choi H, Balci S, Akkas G, Adsay V. Serous cystic neoplasms of the pancreas: clinicopathologic and molecular characteristics. Semin Diagn Pathol. 2014; 31: 475-483.
- Adsay NV. Cystic neoplasia of the pancreas: pathology and biology. J Gastrointest Surg. 2008; 12: 401-404.
- Yip-Schneider MT, Wu H, Dumas RP, Hancock BA, Agaram N, Radovich M. Schmidt CM Vascular endothelial growth factor, a novel and highly accurate pancreatic fluid biomarker for serous pancreatic cysts. Journal of the American College of Surgeons. 2014; 218: 608-617.
- Shah AA, Sainani N, Kambadakone AR, Shah ZK, Deshpande V, Hahn PF, et al. Predictive value of multi-detector computed tomography for accurate diagnosis of serous cystadenoma: radiologic-pathologic correlation. World J Gastroenterol. 2009.
- Choi JY, Kim MJ, Lee JY, Lim JS, Chung JJ, Kim KW, et al. Typical and atypical manifestations of serous cystadenoma of the pancreas: imaging findings with pathologic correlation. AJR Am J Roentgenol. 2009; 193: 136-142.