Case Report
Mediastinal Cavernous Hemangioma in a Child with Pulmonary Hypertension
Rotaru N1*, Maliga O1, Crivcheanschii M1, Codreanu I1, Repin O2 and Munteanu A3
1Department of Radiology, State University of Medicine and Pharmacy Republic of Moldova, Moldova
2Department of Cardiac Surgery, Clinical Republican Hospital, State University of Medicine and Pharmacy Republic of Moldova, Moldova
3Department of Pathology, Clinical Republican Hospital, State University of Medicine and Pharmacy Republic of Moldova, Moldova
*Corresponding author: Natalia Rotaru, Department of Radiology, State University of Medicine and Pharmacy “Nicolae Testemitanu” Chisinau, MD 2025, Moldova
Published: 09 Sep, 2016
Cite this article as: Rotaru N, Maliga O, Crivcheanschii
M, Codreanu I, Repin O, Munteanu A.
Mediastinal Cavernous Hemangioma in
a Child with Pulmonary Hypertension.
Clin Oncol. 2016; 1: 1086.
Abstract
We present a rare case of mediastinal cavernous hemangioma in a 9-year old girl with advanced pulmonary hypertension. Dynamic contrast enhanced computed tomography of the chest revealed a heterogeneous mass in the antero-superior mediastinum with multiple scattered calcifications, gradually increasing puddles of contrast enhancement and a dilated central vein draining into the superior venae cavae. Surgical resection was performed via median sternotomy. The central vein was ligated in close proximity to its draining point and the entire mass was carefully dissected and excised. The histopathological findings were consistent with cavernous hemangioma. Her postoperative course was uneventful and she was subsequently discharged. The cause of her pulmonary hypertension, however, remained uncertain and required further investigation.
Introduction
Cavernous hemangiomas (also known as cavernomas or cavernous angiomas) are developmental vascular malformations commonly considered as vascular hamartomas [1,2]. Usual locations are in the skin, subcutaneous tissue, brain, several viscerae and vertebral bodies [1,3]. Cavernomas within the lungs or mediastinum are very rare [1,4]. Hereby we present a rare case of mediastinal cavernous hemangioma in a child with advanced pulmonary hypertension.
Case Presentation
A 9-year old girl presented with exertional dyspnea that has been gradually increasing during
the last year. On examination, her physical development and growth appeared normal for her age
with no cyanosis, digital clubbing or peripheral edema. Chest auscultation revealed normal breath
sounds and a louder S2 at the heart base.
Her chest X-ray revealed an abnormal mediastinal shadow, the findings being suspicious of a
right upper mediastinal mass (Figure 1). Noncontrast enhanced computed tomography (CT) scan of
the chest revealed a well-circumscribed ovoid mass in the antero-superior mediastinum, measuring
8.4 x 5.0 x 4.4cm (Figure 2). The content of the mass was heterogeneous with regions of nodular and
tubular soft-tissue, liquid and fat attenuation as well as multiple scattered calcifications. Contrastenhanced
CT (following inravenous administration of 45 mL of Visipaque 320) demonstrated
mild heterogeneous enhancement within the mass during the arterial phase (up to +80HU, Figure
3) with subsequent intensification during the venous phase (up to +130HU, Figure 4). A dilated
central vein measuring 1.2cm in diameter was also seen draining directly into the superior vena
cavae, the appearance being suggestive of a mediastinal hemangioma rather than teratoma. In
addition, the pulmonary artery appeared prominently dilated (2.9cm in diameter versus 1.9cm for
ascending aorta), the findings being highly suggestive of pulmonary hypertension (Figure 3 and
4). Catheterization of the right side of the heart revealed a systolic pressure in the right ventricle
of 74 mmHg and resting systolic/diastolic/mean pulmonary arterial pressures of 60/34/46 mmHg,
confirming the diagnosis of pulmonary hypertension. No intracardiac shunts were present.
Surgical resection was performed via median sternotomy. Intraoperatively the mass appeared
well demarcated, located between the pericardium and right mediastinal pleura, encasing the right
phrenic nerve and having a large central vein that was draining into the superior vena cavae. The
central vein was ligated in close proximity to its draining point and the entire mass was carefully
dissected and excised (Figure 5). The postoperative recovery was
uneventful. A chest X-ray obtained in the early postoperative period
is shown in Figure 6. The histological results of the excised mass
revealed a cavernous hemangioma (Figure 7) and the patient was
subsequently discharged.
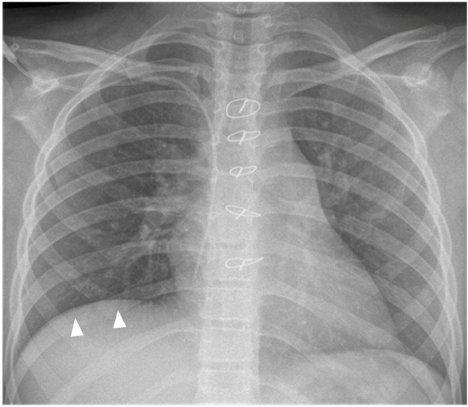
Figure 1
Figure 1
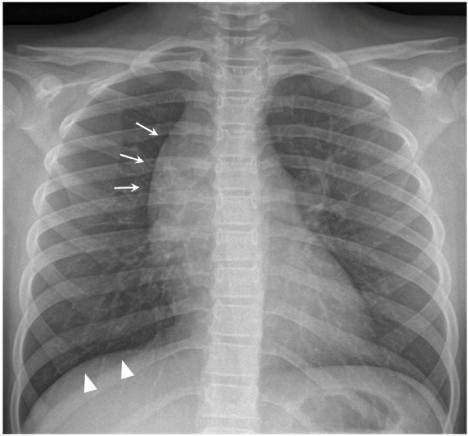
Chest X-ray in posteroanterior (PA) view showing a well-marginated
mass in the right upper mediastinum (arrows). Intraoperatively it has been
found the mass was encasing the right phrenic nerve, which might be related
to mildly elevated right hemidiaphragm (arrowheads).
Figure 2
Figure 2
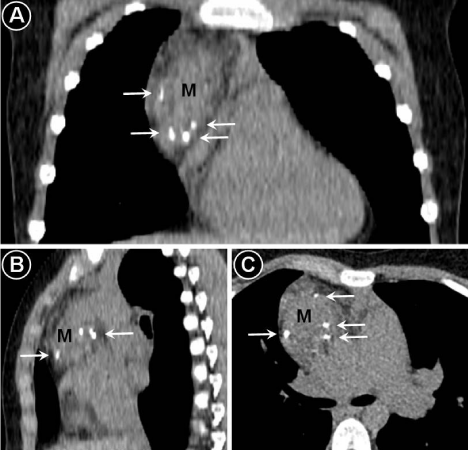
Noncontrast enhanced computed tomography of the chest showing
a heterogeneous mass (M) in the antero-superior mediastinum with scattered
calcifications pointed by arrows. Panel A – coronal view, panel B – sagittal
view, panel C – axial view.
Discussion
Mediastinal hemangiomas usually occur in children and young
adults, up to 75% cases being registered before the age of 35 years
[5-7]. Pre-operative diagnosis can be challenging, as the lesion
usually manifests as a nonspecific mass [5,6,8,9]. Transthoracic
core needle biopsy may be associated with significant bleeding
complications [10,11], therefore medical imaging plays an important
role in the management of these patients. When presenting as an
anterior mediastinal mass, differential diagnosis is commonly made
with other heterogeneous lesions such as teratoma, lymphoma or
lymphangioma [5].
Even though many lesions can be appreciated at conventional
radiography, computed tomography (CT) is the most important
tool in the evaluation of a mediastinal mass [12]. Several imaging
features in our patient were highly suggestive of mediastinal
hemangioma, avoiding the need for biopsy and potential bleeding
complications. Scattered punctuate calcifications within the mass
resembled the pattern seen in phleboliths. Although several patterns
of calcification resembling that of teeth or bones can be seen in
teratoma, phleboliths are virtually diagnostic of hemangioma [5,13].
A dilated central vein draining into the superior vena cava was also
indicative of mediastinal hemangioma rather than teratoma. Slow,
gradually increasing and prolonged contrast stains were similarly
favoring a diagnosis of hemangioma, the characteristic “puddles” of
enhancement after contrast administration being usually seen in the
cavernous subgroup [5,8,10]. Mediastinal lymphoma can appear as a
heterogenous mediastinal mass; however, calcifications in untreated
patients with lymphoma are exceedingly rare [5,14]. Lymphangiomas
can also present as anterior or superior mediastinal masses; however
they are commonly cystic lesions and calcifications are rather
unusual [5,15]. Most lymphangiomas typically do not enhance after
contrast administration, even though marked enhancement has been
reported in certain lymphangiomas with associated hemangiomatous
components or vascular aneurysms [5,15].
The choice of treatment is dependent on various factors such
as related organ, clinical symptoms, depth of invasion and the
vascular structure of the tumor, the size of hemangioma or interval
progression and can include embolization, sclerotherapy, and surgical
resection. Resection of mediastinal hemangiomas via video-assisted
thoracoscopic surgery has also been reported [6,11,16]. In cases of
resection, the lesion should be completely removed as relapses are
directly related to incomplete resection [6,7,13]. Irradiation is not
recommended as the needed radiation dose is very high and has
severe potential complications especially in children [13]. Longterm
clinical and radiological follow-up is recommended for early
diagnosis of relapses [6,13].
Our patient was also referred for further evaluation and close
monitoring of her pulmonary hypertension. Recent studies define
pulmonary hypertension as an abnormal elevation of pressure
in pulmonary circulation, with a resting mean pulmonary arterial
pressure higher than 25 mmHg at catheterization of the right side
of the heart, regardless of the underlying mechanism [17,18].
Pulmonary hypertension has been reported in patients with
pulmonary hemangiomatosis [19]. Hemangiomas can also represent
a potential source of recurrent pulmonary embolism [20,21]. In our
patient the cause of her pulmonary hypertension remained uncertain
and required further investigation.
Figure 3
Figure 3
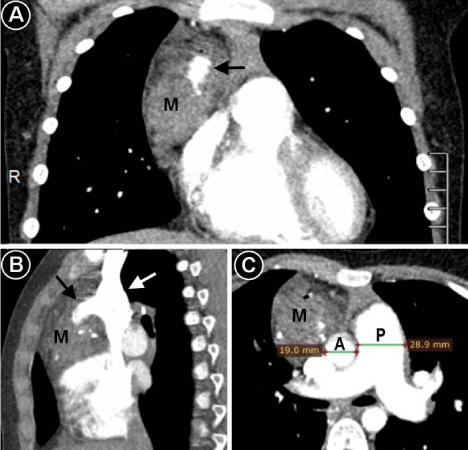
Arterial phase of contrast enhanced computed tomography
showing only mild enhancement of the mediastinal mass (M). A large vein
in the center of the mass (pointed by a black arrow) was filled with contrast
retrogradely from superior vena cavae (pointed by a white arrow), the
contrast being injected into a vein of the right arm. The pulmonary artery (P)
appears prominently dilated compared to ascending aorta (A), the findings
being consistent with pulmonary hypertension. Panel A – coronal view, panel
B – sagittal view, panel C – axial view.
Figure 4
Figure 4
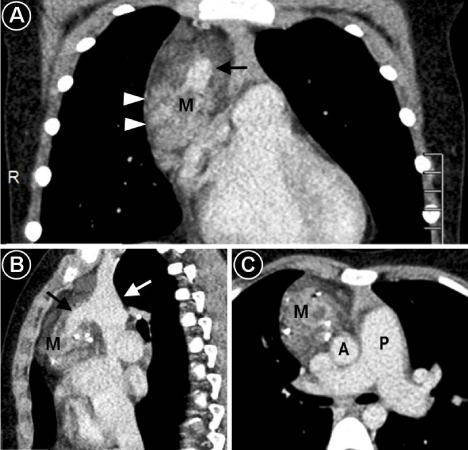
Venous phase of contrast enhanced computed tomography
showing puddles of heterogeneous enhancement (arrowheads) within the
mediastinal mass with a better visualization compared to arterial phase. A
large vein in the center of the mass (pointed by a black arrow) is draining
into superior vena cavae (pointed by a white arrow). The pulmonary artery
(P) appears prominently dilated compared to ascending aorta (A). Panel A –
coronal view, panel B – sagittal view, panel C – axial view.
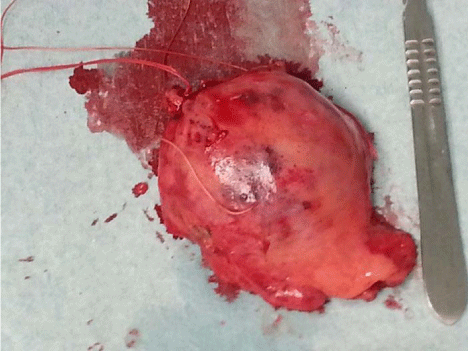
Figure 5
Figure 6
Figure 6
A chest X-ray obtained in the early postoperative period. The
previously seen mediastinal mass (pointed by arrows in Figure 1) is no longer
visualized. Elevation of right hemidiaphragm (arrowheads) is likely related
to partial resection of the right phrenic nerve, which was encased by the
mediastinal mass. Sternal wires after median sternotomy are also noted.
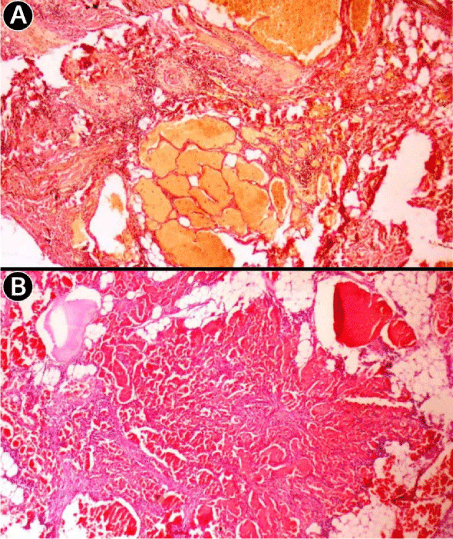
Figure 7
Figure 7
Histopathological findings of the excised mediastinal mass were
consistent with cavernous hemangioma. A - Van Gieson's picrofuchsin staining
(magnification ×10) demonstrates large cavernous spaces and stromal
vessels with an intervening fibrous interstitium. B - Hematoxylin and eosin
(HE) staining (magnification ×20) reveals multiple cavernous spaces
separated by fibrous septa, smaller capillaries and congested vascular
channels interconnected within a fibrous stroma.
References
- Saumench R, Barcia JA, Arnau A, Canto A. Combined thoracotomy and laminectomy for spinal cavernomas with intrathoracic growth. Interact Cardiovasc Thorac Surg. 2004; 3: 76-78.
- Saringer W, Nobauer I, Haberler C, Ungersbock K. Extraforaminal, thoracic, epidural cavernous haemangioma: case report with analysis of magnetic resonance imaging characteristics and review of the literature. Acta Neurochir (Wien). 2001; 143: 1293-1297.
- Badinand B, Morel C, Kopp N, Tran Min VA, Cotton F. Dumbbell-shaped epidural capillary hemangioma. AJNR Am J Neuroradiol. 2003; 24: 190-192.
- Kaya SO, Samancilar O, Usluer O, Acar T, Yener AG. Giant Cavernous Haemangioma of the Anterior Mediastinum. Eurasian J Med. 2015; 47: 216-217.
- Agarwal PP, Seely JM, Matzinger FR. Case 130: mediastinal hemangioma. Radiology. 2008; 246: 634-637.
- Roldan-Banos S, Garcia-Barajas S, Leon-Medina D. Cavernous hemangioma of the thymus. Arch Bronconeumol. 2012; 48: 303.
- Ose N, Kobori Y, Takeuchi Y, Susaki Y, Taniguchi S, Maeda H. Cavernous hemangioma in the thymus: a case report. Surg Case Rep. 2016; 2: 10.
- Nishikawa H, Osaki T, Tajima Y, Yoshimatsu T, Nagashima A, Yasumoto K. Hemangioma in the anterior mediastinum. Jpn J Thorac Cardiovasc Surg. 2003; 51: 442-444.
- Deepak J, Babu MN, Gowrishankar BC, Ramesh S. Mediastinal hemangioma: Masquerading as pleural effusion. J Indian Assoc Pediatr Surg. 2013; 18: 162-164.
- Cheung YC, Ng SH, Wan YL, Tan CF, Wong HF, Ng KK. Dynamic CT features of mediastinal hemangioma: more information for evaluation. Clin Imaging. 2000; 24: 276-278.
- Schreiner W, Sirbu H. Video-assisted technique for resection of a large mediastinal hemangioma. Multimed Man Cardiothorac Surg. 2010; 1: 2010(316): mmcts.2009.004135.
- Juanpere S, Canete N, Ortuno P, Martinez S, Sanchez G, Bernado L. A diagnostic approach to the mediastinal masses. Insights Imaging. 2013; 4: 29-52.
- Calisaneller T, Ozdemir O, Yildirim E, Kiyici H, Altinors N. Cavernous hemangioma of temporalis muscle: report of a case and review of the literature. Turk Neurosurg. 2007; 17: 33-36.
- Alobeidy ST, Ilowite J, Donovan V, Selbs E, Badler R, Katz DS. Calcification in untreated mediastinal Hodgkin's lymphoma. J Thorac Imaging. 2001; 16: 304-306.
- Shaffer K, Rosado-de-Christenson ML, Patz EF Jr, Young S, Farver CF. Thoracic lymphangioma in adults: CT and MR imaging features. AJR Am J Roentgenol. 1994; 162: 283-289.
- Hirai K, Takeuchi S, Bessho R, Ohaki Y, Koizumi K, Shimizu K. Venous hemangioma of the anterior mediastinum. J Nippon Med Sch. 2010; 77: 115-118.
- Pena E, Dennie C, Veinot J, Muniz SH. Pulmonary hypertension: how the radiologist can help. Radiographics. 2012; 32: 9-32.
- Badesch DB, Champion HC, Sanchez MA, Hoeper MM, Loyd JE, Manes A, et al. Diagnosis and assessment of pulmonary arterial hypertension. J Am Coll Cardiol. 2009; 54: S55-66.
- O'Keefe MC, Post MD. Pulmonary capillary hemangiomatosis: a rare cause of pulmonary hypertension. Arch Pathol Lab Med. 2015; 139: 274-277.
- Yokosuka T, Yoshii S, Hosaka S, Suzuki S, Takahashi W, Osawa H, et al. Surgical treatment of chronic pulmonary thromboembolism caused by a cavernous hemangioma at the lower limb. Kyobu Geka. 2001; 54: 973-976.
- Arkadopoulos N, Stafyla V, Karapanos K, Yiallourou AI, Koureas A, Kondi-Pafiti A, et al. Recurrent pulmonary embolism due to giant hepatic hamangioma treated with hepatectomy under vascular exclusion. Ann Vasc Surg. 2010; 24: 827.