Case Report
The Change of Standard Management of Post-Intubation Endotracheal Laceration Owing to Typical Wound Drainage after Mastectomy
Jarosław Szefel1,2, Wiesław Janusz Kruszewski1,2 and Anna Madej-Mierzwa2*
1Division of Propaedeutics of Oncology, Medical University of Gdansk, Gdansk, Poland
2Department of Oncological Surgery, Gdynia Oncology Centre, Gdynia, Poland
*Corresponding author: Anna Madej-Mierzwa, Department of Oncological Surgery, Gdynia Oncology Centre, Powstania Styczniowego 1, 81- 519 Gdynia, Poland
Published: 18 Aug, 2018
Cite this article as: Szefel J, Kruszewski WJ, Madej-
Mierzwa A. The Change of Standard
Management of Post-Intubation
Endotracheal Laceration Owing
to Typical Wound Drainage after
Mastectomy. Clin Oncol. 2018; 3: 1507.
Abstract
Post-intubation endotracheal laceration is very rare (1/20 000). Subcutaneous emphysema and
pneumomediastinum constitute a dominating symptom of post-intubation endotracheal laceration.
This complication can be treated conservatively but at times it requires an endoscopic intervention or
surgical procedure. We concluded that routinely applied suction drainage of a site of organ removal
allowed for a resignation from suggested bilateral 2-cm incisions of the skin and subcutaneous tissue
under the clavicles in order to remove the air collected under the skin. The classification of postintubation
endotracheal laceration suggested by Aghajanzadeh et al. as well as the algorithm of
proceeding according to Cardillo et al. facilitate therapeutic decisions in such cases.
Keywords: Breast procedures; Post-intubation endotracheal laceration; Pneumomediastinum; Subcutaneous emphysema
Case Presentation
A 84-year-old woman diagnosed with right breast cancer, stage IIA (cT2N0M0) was admitted in
a good general condition to Breast Cancer Unit in the Gdynia Oncology Centre, Maritime Hospital
in Gdynia. The multidisciplinary team offered the patient a simple mastectomy with a biopsy of
sentinel lymph nodes.
The patient was anesthetized and intubated with a cuffed endotracheal tube No. 8 to a depth
of 20 cm from the incisors. The sealing cuff was filled with 10 ml of air. Prior to the surgery, the
injection of blue dye (Patent Blue) and radioactive label in the region of the nipple- areolar complex
to locate sentinel nodes was performed. In the intraoperative histopathological examination, no
metastases were found in sentinel lymph nodes.
The operation under anesthetic was uneventful. Two Redon drainage systems were placed into
the mastectomy site, and then the skin was stitched with two layers of stitches. Post-operative active
drainage creating negative pressure in the wound area with the Redon suction bottle was applied.
After 6 hr from the end of the operation, there were gradually increasing features of restlessness,
hallucinations and delusions called postoperative delirium. The patient was given haloperidol at a
dose of 2.5 mg to 5 mg intravenously every 6 hr for sedation. Because hypoxemia is a risk factor of
postoperative delirium, we administered breathable oxygen through the face mask. After about 16
hrs, the postoperative delirium began to decrease and after 3 days it completely resolved.
The edema of subcutaneous tissue of the neck, chest wall, face, eyelids, and scalp appeared
and began to build up in the first day after tracheal extubation. Physical examination revealed
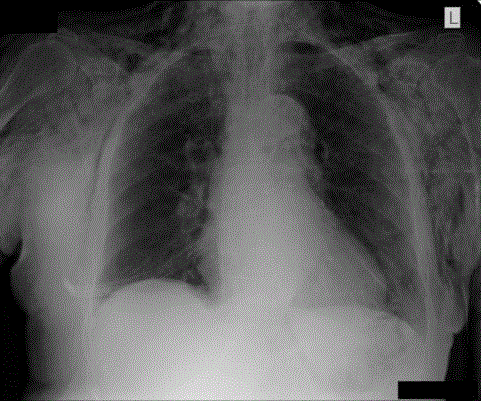
massive subcutaneous emphysema (Figure 1). Standard chest and neck X-ray was performed and
the presence of extensive subcutaneous emphysema and a pneumomediastinum were confirmed
(Figure 2).
The chest CT scan showed extensive subcutaneous emphysema in the neck and retropharyngeal
space, pneumomediastinum, a thin layer of pneumothorax, and extensive subcutaneous emphysema
of the upper chest wall and neck (Figure 4A).
There was a defect of the membranous part of the trachea at the Th2– Th3 level, 2 mm wide and
8 mm long, along its entire thickness (Figure 3).
Bronchoscopy is the gold standard for determining the correct
diagnosis, but it was not done in this case.
According to Conti recommendations conservative treatment
was implemented [1]. Empirical intravenous antibiotic therapy was
used to reduce the risk of mediastinal inflammation.
Maintaining the negative pressure in the system draining the space
after mastectomy was difficult, for the first days after surgery. Initially,
Redon's bottle required repeating the maneuver of creating a vacuum
every 2 hrs, because it quickly filled up with gas and serous-bloody
contents. After 3 days, the subcutaneous emphysema of the face, neck
and chest began to decrease. We believe that the outflow of air from
the subcutaneous tissue and mediastinum to the suction container
was the cause of rapid reduction of subcutaneous emphysema.
In computed tomography of the chest performed on day
13 after surgery, a reduction in subcutaneous emphysema and
pneumomediastinum was demonstrated. Tracheal injury was no
longer visible (Figure 4B). In good general condition, the patient was
discharged home on the 14th day after surgery.
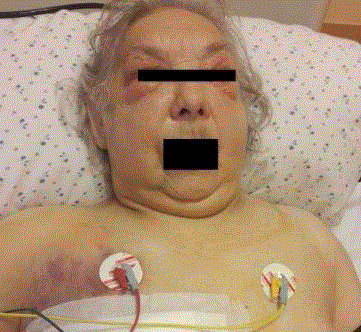
Figure 1
Figure 1
Photo taken on the first day after surgery. The edema of
subcutaneous tissue of the neck, chest wall, face, eyelids, and scalp.
Figure 2
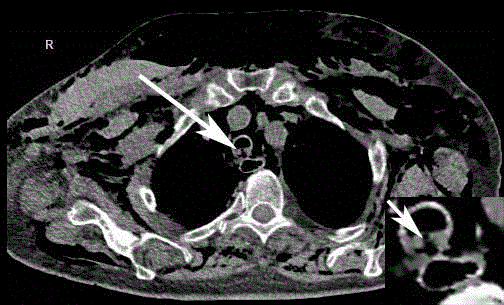
Figure 3
Figure 3
Axial chest computed tomography image with lung window (see
arrow) indicates the disruption of the membranous part of the trachea,
pneumomediastinum and subcutaneous emphysema.
Figure 4A
Figure 4A
CT scan on the first day after mastectomy. The arrow shows
post-intubation endotracheal laceration at the same level as in Figure 3.
Figure 4B
Figure 4B
A follow-up CT scan on day 13 after mastectomy shows no defect
in the tracheal wall, with substantial resolution of the pneumomediastinum
and subcutaneous emphysema.
Discussion
Post-intubation endotracheal laceration is very rare but it is a
potentially life-threatening condition (1/20 000) [2]. In the available
scientific literature we have not found any reports concerning such
complications after mastectomy.
The trachea wall may be injured during endotracheal intubation
by the stylets or tube tips placed excessively; cuff over inflation or tube
repositioning maneuvers without deflating the cuff [3,4].
The communication of the space between the fascias enables the
flow of air from an endotracheal laceration to the region of the neck,
mediastinum and the thoracic cavity.
If there is a suspicion of post-intubation tracheal laceration, a
high resolution computed tomography with contrast and flexible
bronchoscopy should be performed [5,6].
Treatment of tracheal rupture may include conservative,
endoscopic and surgical treatment depending on the patient’s clinical
condition and on the characteristic endotracheal laceration [7,8].
According to Conti et al. a conservative treatment is indicated
in patients with superficial and short tracheal tears <4 cm in length
stable emphysema, and no evidence of sepsis while surgery is the
treatment of choice for laceration >4 cm [1].
Mullan et al. have suggested that the length of intact trachea >3
cm above the carina is the important predictive factor for a successful
conservative treatment [9]. Cardillo et al. classified endotracheal
laceration into four levels and proposed an algorithm for its
management [10]. Level I – IIIA can be managed conservatively e.g.
with a bronchoscopic application of fibrin sealant onto the lesion or
other materials [11,12]. Any III B tracheal laceration requires surgical
treatment.
Aghajanzadeh M. and all. proposed a classification of
subcutaneous emphysema based on an anatomical range of five
grades [13]. Subcutaneous emphysema in grades 1 and 2 usually
subsides spontaneously and does not require a specific treatment.
However, in grade 3, 4 and 5 patients require treatment with two
bilateral 2-cm infraclavicular incisions to the external thoracic fascia
followed by suction for evacuating air [14]. Pneumothorax requires
chest drainage.
The main presenting symptom pneumomediastinum is a sudden
and acute chest pain, usually retrosternal, radiating to the neck or the
back which occurs in 60% to100% [15,16].
Other presenting symptoms include rhinolalia (nasally sounding
voice), hoarseness, neck swelling and Hamman's sign (crunching,
rasping sound, synchronous with the heartbeat) [17].
The diagnosis of pneumomediastinum is usually confirmed on
the basis of a frontal and lateral chest X-ray showing lucent streaks,
bubbles of air outlining mediastinal structures [18].
Patients with pneumomediastinum who are treated conservatively
should be ensured bed rest, effective pain and cough treatment as well
as preventive antibiotic therapy. Haloperidol has been a widely used
antipsychotic medication in the treatment of postoperative delirium
[19]. Antibiotic is applied preventively.
Conclusion
Post-intubation endotracheal laceration is very rare but is a potentially life-threatening condition. For the first time it is described in patient subjected mastectomy. In this case, an effective way to treat this complication was drainage sucking the place after removal of the breast. It allowed for a resignation from bilateral 2-cm incisions under the clavicles in order to remove the air collected under the skin.
References
- Conti M, Pougeoise M, Wurtz A, Porte H, Fourrier F, Ramon P, et al. Management of postintubation tracheobronchial ruptures. Chest. 2006;130(2):412-8.
- Minambres E, Buron J, Ballesteros MA, Llorca J, Munoz P, GonzalezCastro A. Tracheal rupture after endotracheal intubation: a literature systematic review. Eur J Cardiothorac Surg. 2009;35(6):1056-62.
- Marty-Ane CH, Picard E, Jonquet O, Mary H. Membranous tracheal rupture after endotracheal intubation. Ann Thorac Surg. 1995;60(5):1367-71.
- Evagelopoulos N, Tossios P, Wanke W, Krian A. Tracheobronchial rupture after emergency intubation. Thorac Cardiovasc Surg. 1999;47(6):395-7.
- Chen JD, Shanmuganathan K, Mirvis SE, Kileen KL, Dutton RP. Using CT to diagnose tracheal rupture. Am J Roentgenol. 2001;176(5):1273-80.
- Scaglione M, Romano S, Pinto A, Sparano A, Scialpi M, Rotondo A. Acute tracheobronchial injuries: Impact of imaging on diagnosis and management implications. Eur J Radiol. 2006;59(3):336-43.
- Prokakis C, Koletsis EN, Dedeilias P, Fligou F, Filos K, Dougenis D. Airway trauma: a review on epidemiology, mechanisms of injury, diagnosis and treatment. J Cardiothorac Surg. 2014;9:117.
- Panagiotopoulos N, Patrini D, Barnard M, Koletsis E, Dougenis D, Lawrence D. Conservative versus Surgical Management of Iatrogenic Tracheal Rupture. Med Princ Pract. 2017;26(3):218-20.
- Mullan GP, Georgalas C, Arora A, Narula A. Conservative management of a major post-intubation tracheal injury and review of current management. Eur Arch Otorhinolaryngol. 2007;264:685-8.
- Cardillo G, Carbone L, Carleo F, Batzella S, Jacono RD, Lucantoni G, et al. Tracheal lacerations after endotracheal intubation: a proposed morphological classification to guide non-surgical treatment. Eur J Cardiothorac Surg. 2010;37(3):581-7.
- Ishikawa K, Kato T, Aragaki M, Hase R, Saikai T, Matsui Y, et al. Endobronchial Closure of a Bronchopleural Fistula Using a Fibrin Glue-Coated Collagen Patch and Fibrin Glue. Ann Thorac Cardiovas. 2013;19(6):423-7.
- Fiorelli A, Cascone R, Di Natale D, Pierdiluca M, Mastromarino R, Natale G, et al. Endoscopic treatment with fibrin glue of post-intubation tracheal laceration. J Vis Surg. 2017;3:102.
- Aghajanzadeh M, Dehnadi A, Ebrahimi H, Fallah Karkan M, Khajeh Jahromi S, Amir Maafi A, et al. Classification and Management of Subcutaneous Emphysema: a 10-Year Experience. Indian J Surg. 2015;77:673-7.
- Beck PL, Heitman SJ, Mody CH. Simple construction of a subcutaneous catheter for treatment of severe subcutaneous emphysema. Chest. 2002;121(2):647-9.
- Macia I, Moya J, Ramos R, Morera R, Escobar I, Saumench J, et al. Spontaneous pneumomediastinum: 41 cases. Eur J Cardiothorac Surg. 2007;31(6):1110-4.
- Caceres M, Ali SZ, Braud R, Weiman D, Garrett HE, Jr. Spontaneous pneumomediastinum: a comparative study and review of the literature. Ann Thorac Surg. 2008;86(3):962-6.
- Kobashi Y, Okimoto N, Matsushima T, Soejima R. Comparative study of mediastinal emphysema as determined by etiology. Internal Med. 2002;41:277-82.
- Iyer VN, Joshi AY, Ryu JH. Spontaneous pneumomediastinum: analysis of 62 consecutive adult patients. Mayo Clin Proc. 2009;84(5):417-21.
- Breitbart W, Marotta R, Platt MM, Weisman H, Derevenco M, Grau C, et al. A double-blind trial of haloperidol, chlorpromazine, and lorazepam in the treatment of delirium in hospitalized AIDS patients. Am J Psychiat. 1996;153(2):231-7.