Research Article
Peripheral Blood Neutrophil to Lymphocyte Ratio is Positively Correlated with Tumour Aggressiveness in Testicular Cancer
Mustafa Ozan Horsanali*, Kutan Ozer and Emin Ozbek
Department of Urology, Izmir Katip Çelebi University Ataturk Training and Research Hospital, Turkey
*Corresponding author: Mustafa Ozan Horsanali, Department of Urology, Izmir Katip Çelebi University Ataturk Training and Research Hospital, Turkey
Published: 17 May 2017
Cite this article as: Horsanali MO, Ozer K, Ozbek E.
Peripheral Blood Neutrophil to
Lymphocyte Ratio is Positively
Correlated with Tumour Aggressiveness
in Testicular Cancer. Clin Oncol. 2017;
2: 1298.
Abstract
Introduction:Testicular cancer represents between 1% to 1.5% of all male neoplasms and 5% of
urological tumours in general. The Neutrophil to Lymphocyte Ratio (NLR), which can easily be
calculated from routine Complete Blood Counts (CBCs) with differentials, is a marker of host
inflammation and has been shown to be an independent prognosticator for a variety of solid
malignancies.
Materials and Methods: We have retrospectively analyzed 128 patients who diagnosed testicular
cancer between January 2006 and July 2012. Patient demographics, preoperative full blood count
and standard histologic tumour characteristics were recorded. Factors analyzed included patient
age, tumour size, histological subtype, Pathological Tumour (pT) stage, N stage, neutrophil count,
lymphocyte count, preoperative and postoperative NLR, alfa fetoprotein, B-HCG and LDH levels.
Routine full blood count results were collected as part of the pre-treatment protocols.
Results: Totaly 128 patients were analyzed retrospectively. The mean lymphocyte counts of all
patients were 4.74 ±2.88 (range 0.32-5.72) and neutrophil counts were 5.93 ± 2.88 (range 1.87-17).
The mean NLR was 3.70 ± 2.87 (range 1.04-21.94). The cut-off rate for NLR was calculated as 3,72.
87 patients were < 3,72 NLR and 41 patients were ≥3,72 NLR. The mean age for the group < 3,72
NLR were 41 (10,6%) and for group ≥3,72 NLR were 34,9 (8,5%) months. There were statistically
significant association between age and NLR ratio (p: 0,002).
Discussion: NLR is one of the widely used markers for systemic inflammatory reactions. Although
increased pretreatment NLR is associated with a poor outcome for various types of cancers, we found
a positive association between preoperative NLR and age, tumour histopathology, preoperative
serum markers and rete testes invasion. In the group of NLR < 3,72 , tumour serum markers were
lower than NLR>3,72 group. In the seminoma histopathology NLR value was < 3,72 and that was
statistically significant.
Conclusion: NLR is a simple, rapid and reliable method of how to evaluate the extent of stress
or systemic inflammation. Our prognostic model based on the NLR and pathologic factors could
be helpful in clinical practice. Also, clinicians should remember that baseline NLR differs among
individuals.
Keywords: Neutrophil; Lymphocyte; Neutrophil to lymphocyte ratio, Testis cancer; Stage
Introduction
Testicular cancer represents between 1% to 1.5% of all male neoplasms and 5% of urological
tumours in general, with 3-10 new cases occurring per 100,000 males/per year in Western societies.
Only 1-2% of cases are bilateral at diagnosis. The histological type varies, although there is a clear
predominance (90-95%) of germ cell tumours. Peak incidence is in the third decade of life for
nonseminoma, and in the fourth decade for pure seminoma [1]. Inflammation has an important
role in the development and progression of many malignancies. Putative mechanisms include
the increased supply of factors that promote carcinogenesis and tumour progression by cells of
the innate immune systems and decreased antitumoral response by immune cells of the adaptive
system [2]. The Neutrophil to Lymphocyte Ratio (NLR), which can easily be calculated from routine
Complete Blood Counts (CBCs) with differentials, is an emerging marker of host inflammation
and has been shown to be an independent prognosticator for a variety of solid malignancies [3].
Neutrophil–Lymphocyte Ratio (NLR) is also used as a parameter
of systemic inflammation in intensive care patients [4]. Cancerous
tissue, besides leading to systemic inflammatory response, may also
lead to a localized, more generalized, and nonspecific inflammatory
response due to destruction and disruption caused by the physical
effects of the tumor. Therefore, NLR is a rapid and simple index of
systemic inflammatory response [5].
An increased pretreatment NLR is associated with poor prognosis
in colorectal, gastric, and ovarian cancer; malignant mesothelioma;
and renal cell carcinoma (RCC) [4,6-8]. According to our knowledge,
relation between NLR and testicular cancer has not been reported
previously. The objective of our investigation was to evaluate the
association between NLR and oncological parameters in patients
undergoing radical orchiectomy for testicular cancer Table 1.
Table 1
Table 2
Materials and Methods
We have retrospectively analyzed 128 patients who diagnosed testicular cancer between January 2006 and July 2012 in Izmir Katip Celebi University Atatürk Training and Research Hospital. Patient demographics, preoperative full blood count and standard histologic tumour characteristics were recorded. It was compiled from individual patient’s medical records, laboratory results, and pathology reports. Factors analyzed included patient age, tumour size, histological subtype, Pathological Tumour (pT) stage, N stage, neutrophil count, lymphocyte count, preoperative and postoperative NLR, alfa fetoprotein, B-HCG and LDH levels. Routine full blood count results were collected as part of the pre-treatment protocols. Demographics and serum values for the NLR were measured on the day before the operation to ascertain the baseline values for neutrophil and lymphocyte counts Table 2. The NLR was defined as the absolute neutrophil count divided by the absolute lymphocyte count. Exclusion criteria for the present study were presence of hematologic disorders or malignensies, active infection at the time of surgical intervention, prior blood transfusion and the presence of other cancer types.
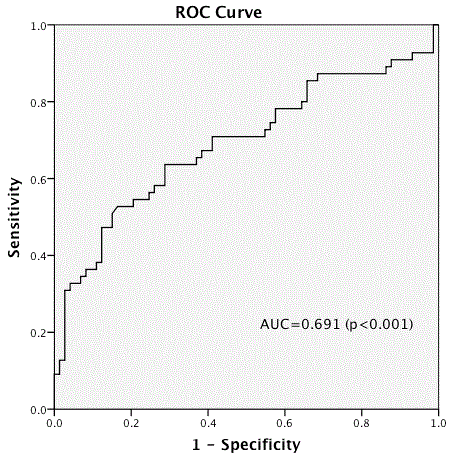
Figure 1
Istatistical Analysis
SPSS 15 statistical package program was used to evaluate the statistical analysis. Descriptive statististics were presented as mean, standard devation, median and min-max values for continuous variables, frequencies and percentages for categorical variables. Student t test was used while analyzing the mean differences of continuous variables between two NLR groups also chi square test was used to conceive the relationship between NLR and other categorical variables. You den Index and ROC Curve analysis were used to define a cut-off value for NLR. We run Kaplan Meier analysis to understand the difference in OAS between two NLR groups. Differences with a P value of < 0.05 were considered statistically significant.
Results
Totally 128 patients were analyzed retrospectively. The mean age of the patients were 39.01 ±10.33 ranging from 19-71 and median age was 38,5. The mean tumour size of the patients was 4.74 ± 2.88 cm ranging from 0 to 17. 48 (37,5 %) patients have mixed germ cell histopathology, 48 (37,5%) patients have seminoma histopathology and 32 (25%) patients have other type of testicular cancer. The mean lymphocyte counts of all patients were 4.74 ± 2.88 (range 0.32-5.72) and neutrophil counts were 5.93 ± 2.88 (range 1.87-17). The mean NLR was 3.70 ± 2.87 (range 1.04-21.94) (Table 1). 82 (64,1 %) of the patients were pT1 stage, 34 (26,6%) were pT2 stage and 12 (9,4%) patients were pT3 stage. 79 (61,7%) patients were N0, 12 (9,4%) were N1 and 12 (9,4%) patients N3 and 25 (19,5%) patients were N3 stage. The mean overall survival of the all patients were 42.37 ±32.04 (range 1-124) month. At the follow up 116 (90,6%) patients were alive and 12 (9,4%) patients were died because of the metastatic disease. The cut-off rate for NLR was calculated as 3,72 by ROC test (Figure 1). 87 patients were < 3,72 NLR and 41 patients were ≥3,72 NLR. The mean age for the group < 3,72 NLR were 41 (10,6%) and for group ≥3,72 NLR were 34,9 (8,5%) months. There were statistically significant association between age and NLR ratio (p: 0,002). There were statistically significance between NLR and tumor histopathology, preoperative AFP, B-HCG, LDH, rete-testes invasion and N stage. In the patients who have < 3,72 NLR, 26 of 87 patients were mixed germ cell carcinoma and 39 patients were seminoma histopathology (p:0,017). In these group the mean tumor size was 4,5 cm (p:0.190) (Table 2). 59 of 87 patients were pT1 stage, 23 of pT2 stage and 5 of pT3 (p: 0,110). 65 of 87 patients were N0, 7 of N1, 5 of N2 and 10 of N3 (p < 0,001) (Table 3). 58 patients have lymphovascular invasion (p: 0,371), 83 patients have rete-testes invasion (p: 0,004), 82 patients had epididymal invasion (p: 0,289) and only one patient has positive surgical margin. For this group, 82 patients have < 1000 preoperative AFP level and 5 patients have ≥1000 AFP levels (p: 0,006). 85 patients have < 1000 B-HCG level and 2 patients have ≥1000 B-HCG levels (p < 0,001). 52 patients have < 225 LDH level and 35 patients have ≥225 LDH levels (p: 0,001) (Table 4).
Table 3
Table 4
Discussion
NLR is one of the widely used markers for systemic inflammatory
reactions. Increasing evidence supports the association between
cancer progression and inflammation [9]. Although increased
pretreatment NLR is associated with a poor outcome for various
types of cancers [4,6,7,10], no study of association between NLR and
testicular cancer has been done to date. To our knowledge we are the
first to investigate the clinical value of NLR for patients with testicular
cancer.
Our study’s goal was to determine whether preoperative NLR
can be incorporated in age, tumor histopathology, tumour serum
markers and TNM stage. There was statistically significance between
preoperative NLR values between age, tumor histopathology,
rete testes invasion and preoperative tumour markers. There is heterogeneity in reported thresholds used to define an elevated NLR
in the literature (range 2-7.7). This may reflect variations in the host
response for different disease sites and stages, or may reflect the
different approaches used when determining cutoff values. Not all
studies used an accepted method for cutoff point determination, and
in some instances the rationale for the cutoff point decision was not
described [11]. In our study we used Youden test to calculate cut off
value of NLR and 3,7 value was calculated as cutoff value for NLR
[12]. Showed a correlation between the NLR ratio of the patients with
early gastric cancer and the prognosis of the patients [13]. Showed
that NLR independently predicts survival in patients with colorectal
liver metastases treated with chemotherapy followed by resection
or chemotherapy only. When chemotherapy normalizes the high
NLR, improved survival is expected. Also, in one study, elevated
preoperative NLR was identified as an adverse predictor of outcome in
patients undergoing potentially curative resection for hepatocellular
carcinoma, and, therefore, patients with high preoperative NLR should
be considered candidates for additional therapies after resection [14].
Reported that increased preoperative NLR was strongly associated
with a poor prognosis in patients with Upper Urinary Tract Urothelial
Carcinoma (UUTUC) by multivariate analysis [15]. In contrast,
an increased NLR was strongly associated with pathologic T stage,
tumor grade, and LVI. Twenty-two (26.5%) of the 83 patients with an
NLR < 2.5 had stage pT3 disease or higher compared with 36 (66.7%)
of the 54 patients with an NLR >=2.5. Twenty- three (27.7%) of the
83 patients with NLR < 2.5 had grade 3 disease compared with 36
(66.7%) of the 54 patients with an NLR >= 2.5. Thirty-three (39.8%)
of the 83 patients with an NLR < 2.5 were LVI positive compared with
39 (72.2%) of the 54 patients with an NLR >= 2.5. These pathologic
factors are important for predicting the prognosis of UUTUC. In our
study we found a positive association between preoperative NLR and
age, tumour histopathology, preoperative serum markers and rete
testes invasion. In the group of NLR < 3,72, tumour serum markers
were lower than NLR >3,72 group and first group was older than
second group. For seminoma histopathology NLR value was < 3,72
and these was statistically significant. In the NLR< 3,72 group lymph
node invasion was higher than other group. NLR can easily evaluated
with preoperative peripheral blood count. We consider that results
of our study can help phycision to predict prognosis and survival of
the patients. Because we found that the patients with NLR < 3,72 have
lymph node metastasis and rete testes invasion as a poor prognostic
factors. So these patients OAS are worst than the patients with NLR
>3,72. In addition, NLR can be predictive factor for other therapies
such as chemotherapy or radiotherapy after surgery. And also NLR
is the easy preoperative test for physician to evaluate patients with
testicular cancer.
Conclusion
Neutrophilia and lymphocytopenia are typical phenomena of the innate immune response to various stressful insults. Relation of neutrophils and lymphocytes during the development of systemic inflammatory response expressed as NLR is a simple, rapid and reliable method of how to evaluate the extent of stress or systemic inflammation. NLR can be used routinely in daily clinical practice of intensive medicine. Our prognostic model based on the NLR and pathologic factors could be helpful in clinical practice. Further multicenteral studies with more patients are needed to confirm our suggestions. Also, clinicians should remember that baseline NLR differs among individuals.
References
- Albers P, Albrecht W, Algaba F, Bokemeyer C, Cohn-Cedermark G, Fizazi K, et al. [EAU guidelines on testicular cancer: 2011 update. European Association of Urology]. Actas Urol Esp. 2012; 36: 127-145.
- Hanahan D1, Weinberg RA. Hallmarks of cancer: the next generation. Cell. 2011; 144: 646-674.
- Proctor MJ, Talwar D, Balmar SM, O'Reilly DS, Foulis AK, Horgan PG, et al. The relationship between the presence and site of cancer, an inflammation-based prognostic score and biochemical parameters. Initial results of the Glasgow Inflammation Outcome Study. Br J Cancer. 2010: 103: 870-876.
- Ohno Y, Nakashima J, Ohori M, Hatano T, Tachibana M. Pretreatment neutrophil-to-lymphocyte ratio as an independent predictor of recurrence in patients with nonmetastatic renal cell carcinoma. J Urol. 2010; 184: 873-878.
- Zahorec R. Ratio of neutrophil to lymphocyte counts-rapid and simple parameter of systemicinflammation and stress in critically ill. Bratisl Lek Listy. 2012: 102: 514.
- Walsh SR, Cook EJ, Goulder F, Justin TA, Keeling NJ. Neutrophil-lymphocyte ratio as a prognostic factor in colorectal cancer. J Surg Oncol. 2005; 91: 181-184.
- Cho H, Hur HW, Kim SW, Kim SH, Kim JH, Kim YT, et al. Pre-treatment neutrophil to lymphocyte ratio is elevated in epithelial ovarian cancer and predicts survival after treatment. Cancer Immunol Immunother. 2009; 58: 15-23.
- Kao SC, Pavlakis N, Harvie R, Vardy JL, Boyer MJ, van Zandwijk N, et al. High blood neutrophil-to-lymphocyte ratio is an indicator of poor prognosis in malignant mesothelioma patients undergoing systemic therapy. Clin Cancer Res. 2010; 16: 5805-5813.
- Mantovani A, Allavena P, Sica A, Balkwill F. Cancer-related inflammation. Nature. 2008; 454: 436-444.
- Ubukata H, Motohashi G, Tabuchi T, Nagata H, Konishi S, Tabuchi T. Evaluations of interferon-gamma/interleukin-4 ratio and neutrophil/lymphocyte ratio as prognostic indicators in gastric cancer patients. J Surg Oncol. 2010; 102: 742.
- Templeton AJ, McNamara MG, Šeruga B, Vera-Badillo FE, Aneja P, Ocaña A, et al. Prognostic role of neutrophil-to-lymphocyte ratio in solid tumors: a systematic review and meta-analysis. J Natl Cancer Inst. 2014; 106: dju124.
- Hirashima M, Higuchi S, Sakamoto K. The ratio of neutrophils to lymphocytes and the phenotypes of neutrophils in patients with early gastric cancer. J Cancer Res Clin Oncol. 1998; 124: 329-334.
- Kishi Y, Kopetz S, Chun YS, Palavecino M, Abdalla EK, Vauthey JN. Blood neutrophil-to lymphocyte ratio predicts survival in patients with colorectal liver metastasis treated with systemic chemotherapy. Ann Surg Oncol. 2009; 16: 614-622.
- Gomez D, Farid S, Malik HZ, Young AL, Toogood GJ, Lodge JP, et al: Preoperative neutrophil-to lymphocyte ratio as a prognostic predictor after curative resection for hepatocellular carcinoma. World J Surg. 2008; 32: 1757-1762.
- Azuma T, Matayoshi Y, Odani K, Sato Y, Sato Y, Nagase Y, et al. Preoperative Neutrophil-Lymphocyte Ratio as an Independent Prognostic Marker for Patients With Upper Urinary Tract Urothelial Carcinoma. Clinical Genitourinary Cancer. 2013; 11: 337-341.