Research Article
Assessment of Low Dose Vigil® Engineered Autologous Tumor Cell (EATC) Immunotherapy in Patients with Advanced Solid Tumors
Luisa Manning1, Minal Barve2,3,4, Gladice Wallraven1, Padmasini Kumar1, Nicolas Taquet1, Ernest Bognar1, Eric Mendeloff4, Jonathan Oh3, Donald D. Rao5, Beena O. Pappen1, Neil Senzer1,2,5, John Nemunaitis1,2,3,4,5*
1Gradalis, Inc., Dallas, TX, USA
2Mary Crowley Cancer Research Centers, Dallas, TX, USA
3Texas Oncology, P.A., Dallas, TX, USA
4Medical City Dallas Hospital, Dallas, TX, USA
5Strike Bio, Dallas, TX, USA
*Corresponding author: John Nemunaitis, Mary Crowley Cancer Research Centers, 12222 Merit Drive, Suite 1500, Dallas, Texas 75251, USA
Published: 03 Apr, 2017
Cite this article as: Manning L, Barve M, Wallraven G,
Kumar P, Taquet N, Bognar E, et
al. Assessment of Low Dose Vigil®
Engineered Autologous Tumor Cell
(EATC) Immunotherapy in Patients with
Advanced Solid Tumors. Clin Oncol.
2017; 2: 1254.
Abstract
Previously we demonstrated not only safety but also provided evidence of clinical benefit to Vigil® vaccine (1 x 107cells/injection 1x/month for 1-8 injections). In addition, we identified a relationship between survival and Vigil® induced circulating activated T-cells against autologous, preprocessed tumor cells (γIFN-ELISPOT) [1,2]. Here we review 15 patients with advanced, heavily pretreated progressive metastatic disease who underwent autologous tumor harvest and subsequent Vigil® construction but in whom manufacturing was only able to construct low-dose Vigil® (1 x 106 – 8.3 x 106 cells/injection 1x/month for 1-8 injections). Of the 12 patients for whom sequential γIFNELISPOT assessment was available, all were γIFN-ELISPOT response negative (<10 spots) at baseline and subsequently developed a positive response. Specifically, 11 converted after 1 cycle of Vigil® immunotherapy and one after 2 cycles. The median (range) γIFN-ELISPOT response was 143.5 (6-474) spots post Vigil® compared to 1 (0-2) pre Vigil®. Median overall survival for these 12 patients was 28.7 months. The three patients without γIFN-ELISPOT assessment had a median survival of 25.3 months. No ≥ grade 1 Vigil® related toxicity was observed. These data which suggest comparable immunological and clinical effectiveness of low-dose Vigil® imply that a smaller harvest tumor volume may be adequate for Vigil® construction, possibly allowing for an image guided core needle biopsy procedure rather than excisional resection for tumor acquisition.
Introduction
The absence of antitumor T-cell activity in advanced cancer patients indicates not only the results of central and peripheral processing, but also one or more of a variety of afferent immune response pathway defects such as impaired antigen processing and presentation, altered cell-to-cell and co-stimulatory signals, secreted tumor and micro environment immunosuppressive cytokines, alterations in effector cell signal transduction and chronic antigen exposure negatively influencing T-cell differentiation and resulting in T-cell exhaustion [3]. Restoration and/or revitalization of T effector cell function is a promising approach for immunotherapy. Vigil® is a DNA plasmid based immunotherapy which utilizes autologous irradiated tumor cells transfected with a DNA plasmid, encoding for GMCSF expression and furin knockdown mediated TGFβ 1 and 2 downregulation. In a previously reported Phase I clinical trial of Vigil® administered at ≥ 1 x 107 cells/injection 1x/month for 1-12 injections in patients with heavily pretreated advanced solid tumors, in addition to demonstrated safety the study suggested a survival advantage as well as a correlation of survival duration with an elicited positive γIFN-ELISPOT response (25.7 months γIFN-ELISPOT + vs. 11.6 months γIFN-ELISPOT-)[1,2]. The safety, effective induction of an immune response (γIFN-ELISPOT) and clinical benefit of Vigil® has been shown in a variety of advanced cancer types [4-7]. However, heretofore there has no data available to characterize the effectiveness of lower dose-range Vigil® (i.e., < 1 x 107 cells/ injection) including both the quantitative γIFN-ELISPOT response and correlation to survival. We now report on 15 patients with less than optimal accessible disease volume for harvest or without sufficient tumor harvest for higher dose, in whom only lower dose Vigil® was able to be constructed and administered under protocol.
Methods
Study design
These lower dose patients were participants in an expanded cohort
of an ongoing open-label, non-randomized, single-arm Phase 1 study
[1,2]. It was established in order to assess lower dose Vigil® above 1
x 106 cells/injection x 4 injections. The standard dose for other Vigil®
dosing has been ≥ 1 x 107 cells/injection x 4 injections. Patients with
solid tumors following prior standard of care cancer treatment were
grouped into 1 of 3 lower dose (1 x 106, 4 x 106, 8 x 106 cells/intradermal
injection) cohorts of plasmid transfected autologous tumor cells once
a month for up to 12 doses as long as sufficient material was available
(minimum of 4 injections). Selection of patients for each dose cohort
was dependent on the amount of tumor cell yield following harvest
and processing of patients entered into the Phase 1 study.
Patients were followed for safety, sequential γIFN-ELISPOT
response assessment and survival. Written documentation of full IRB
approval of the protocol and consent document was required before
a patient could be registered at the site. All patients were treated at a
single site, The Mary Crowley Cancer Research Center (Dallas, TX).
Inclusion criteria
Histologically confirmed advanced or metastatic deemed noncurable
with standard of care therapy (if limited to a single lesion
may not be a candidate for curative surgery or radiation therapy)
was required. Successful vaccine manufacture from one or more
tissue sites or fluid obtained from the following major organ systems:
digestive, endocrine, reproductive, respiratory and urinary was
allowed. Clinically indicated surgical procedure to collect viable
tumor for Vigil® EATC manufacturing was required for enrollment.
All patients were required to have signed IRB approved informed
consent.
Vigil® manufacture
The construction and GMP manufacturing of Vigil®
immunotherapy have previously been described [1,2]. Vigil® cellular
immunotherapy was constructed for every patient after surgical
collection of autologous tumor tissue, dissociation into single-cell
suspension, plasmid transfection, incubation and irradiation.
γIFN-ELISPOT assay
The γIFN-ELISPOT (enzyme-linked immunospot) assay as
previously described [4] was performed using the enzyme-linked
immunospot assay for IFN-γ, (BD Biosciences, San Jose, CA, USA).
Target (Tumor) cells and Effector (mononuclear) cells were applied
in a 3:1 ratio (7.5 x 103 : 2.5 x 103) on an antibody coated microplate
reacting with IFN-γ. Quantitative results in form of reactive spots
to IFN-γ, secreted by cytotoxic CD8+ T-cells, were measured and
used for immune response function analysis. The reading of the
γIFN-ELISPOT plates was performed independently by ZellNet
Consulting, Inc. (Fort Lee, NJ, USA). A value of ≥ 10 spots and 2x
baseline was considered as positive γIFN-ELISPOT response status.
Serial γIFN-ELISPOT analyses were performed at baseline, month 2,
month 4 and subsequent time points. Vigil® induced γIFN-ELISPOT
conversion was defined as ≥ 10 spots and 2x baseline. All patients
were γIFN-ELISPOT negative at baseline.
Statistical evaluation
Survival was analyzed from time of surgical procurement. Patients
were censored for survival on the last known date alive. Analyses of
time-to-event variables were performed with the use of log-rank
statistics and Kaplan–Meier survival curves.
Table 1
Results
Patient population
Fifteen patients with advanced solid tumors received at least 1
dose of Vigil® (1.0 – 8.3 x 106 cells via ID injection). Demographics are
shown in Table 1. All patients underwent tumor procurement as part
of the standard medical management for palliative control of disease
and qualified for Vigil® immunotherapy. Time of Vigil® treatment was
a median of 166 days (range 45-369 days) after tissue procurement.
Safety
A total of 71 Vigil® autologous tumor cell administrations were
given to the 15 patients. All treatment-related AE’s were limited to Grade 1 injection site reactions such as erythema, swelling, induration,
tenderness, or pain (Table 2). Other non-treatment related AE’s were
observed: 31 grade 1, 8 grade 2 and 4 ≥ grade 3 [2 due to disease
progression, 1 grade 3 transient hypoglycemia and 1 grade 4 transient
hypoglycemia].
Survival
We observed the mean Kaplan-Meier survival for all 15 patients
treated with “lower-dose” Vigil® as 968 days from time of tissue
procurement. Separate survival of the γIFN-ELISPOT assayed (n =
12), (n = 3 not assayed for ELISPOT) showed similar results (data not
shown). Actual survival of 93% was observed at 1 year. Survival of
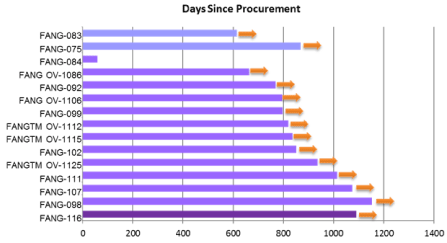
individual patients is shown by dose (Figure 1).
ELISPOT response
Twelve patients were analyzed for γIFN-ELISPOT assay at
baseline (pre Vigil®) and post treatment with Vigil® engineered
autologous tumor cells. All patients were baseline negative with
a median of 1 spot (range 0 to 2 spots). γIFN-ELISPOT reactivity
demonstrated a significant induction of systemic immune response
in 12 of 12 evaluable patients after treatment start with Vigil®. Eleven
patients had a positive γIFN-ELISPOT response status by month 2
(after 1 cycle of Vigil®) and one patient by month 3 (after 2 cycles of
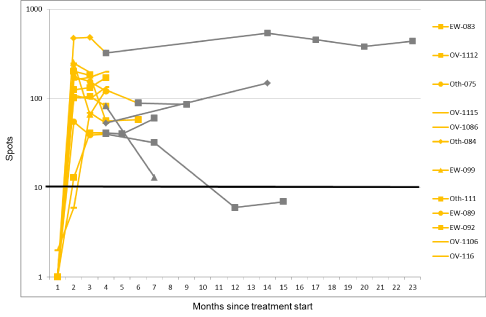
Vigil®) (Figure 2). The median value of ELISPOT “+” response status
after one cycle of Vigil® was 143.5 (6 to 474) spots. One patient had
responses below threshold of 10 spots prior to subsequent elevation.
In addition, three patients (F-075, F-084, Ov-116) were followed
for long-term ELISPOT assessments after completion of treatment
with Vigil® immunotherapy. Two of these patients maintain positive
ELISPOT status for 15 months (F-075) and 23 months (F-084) and had prolonged survival of ≥ 1075 days.
Table 2
Figure 1
Figure 1
Individual survival by dose. All 15 patients are represented by
purple bars.Light purple graph represents 1x106 cells, purple represents
4x106 cells and dark purple represents 8x106. The y-axis represents each
patient’s (#116, #098, #107, #111, #OV-1125, #102, #OV-1115, #OV-1115,
#099, #OV1106, #092, #OV1086, #084, #075, #083) survival organized by
dose level. The x-axis represents time in days since procurement.The orange
arrows represent survival “Alive” status.
Figure 2
Figure 2
γIFN-ELISPOT response curve. Positive is defined as a threshold
of ≥10 reactive spots. 12 patients are represented by color code of i) yellow:
on treatment with Vigil®, or ii) grey: off-treatment. The y-axis represents the
reactive spots on the γIFN-ELISPOT assay. The x-axis represents time in
months since treatment start. All patients were observed to have a negative
ELISPOT response prior to Vigil® (≤10 spots).
Discussion
This evaluation of lower-dose Vigil® immunotherapy in patients
with advanced solid tumors demonstrates preservation of immune
responsiveness (by γIFN-ELISPOT) to a similar degree as previously
reported in similar heavily pretreated patients who received higher
Vigil® doses (≥ 1 x 107 cells/ml) [1,2,5]. Importantly, there also appears
to be comparable survival duration. These results are encouraging
and suggest durable immune activity induced at up to a 1log lower
dose. This is of interest in further development of Vigil® technology
as the quantity of harvested tumor required to achieve such a dose
level could be obtained by image guided core biopsy rather than
surgical resection. As previously reported, a ≥ 2cm nodule has been
required to achieve manufacture of ≥ 4 vials of Vigil® at 1 x 107 cells/
injection. The potential for a clinically effective lower dose Vigil® as
demonstrated in these patients justifies further study in an effort to
increase the number of patients eligible for tumor harvest and to
minimize the potential for discomfort and side effects that can be
associated with a more extensive surgical resection.
The autologous tumor cell approach utilized by Vigil® provides
the full spectrum of tumor associated antigens, differentiation
antigens, tumor-germ cell antigens, and unique neoantigens that
are expressed on tumor cells [8]. The latter, specific to cancer cells
and exempt from central and peripheral processing, have emerged as
highly immunogenic immunotherapeutic targets [9-11].
A phase II study of a TGFβ2 antisense allogeneic tumor cell
vaccine (Belagenpumatucel-L) suggested a vaccine dose-response
relationship to survival; a 581 day median survival of those receiving ≥ 2.5 x 107 cells/injection compared to 252 days in those receiving
1.25 x 107 cells/injection (p = 0.0186) [12]. Unlike Vigil® the allogeneic
Belagenpumatucel-L would not have presented tumor specific
neoantigens, effected only a > 35% downregulation of TGFβ2 rather
than a 93.5% and 92.5% downregulation of TGFβ1 and TGFβ2,
respectively [1], and did not incorporate the GMCSF transgene.
Microenvironment TGFβ1, 2 is a multifariously immunosuppressive
cytokine affecting CD8 T-cells, CD4 T-cells (including induction of
Tregs) and dendritic cell proliferation, migration and activity [13].
In addition, the downregulation of TGFβ in murine pancreatic
cancer models in combination with allogeneic GMCSF secreting
GVAX shows significant benefit in survival and Treg depletion [14].
Likewise, TGFβ1 gene silencing in ovarian cancer cells demonstrated
enhanced immune response by downregulation of CD4CD25+FoxP3
Tregs, ovarian cancer antigen-specific immune response targeting
mesothelin and HE4, and increased numbers of CD8+ interferongamma
secreting T effector cells [15].
It is hypothesized that γIFN-ELISPOT assessment, considering
its correlation with survival, provides an early indicator of Vigil®
enhanced immunogenicity and clinical activity and, via an interaction
of multifactorial functional pathways, allows for effectiveness even at
lower doses. A broader in-depth assessment of the active T effector
γIFN-ELISPOT positive fraction and determination of the individual
neoantigen signal[s] induced are underway. Further evaluation
of lower dose Vigil® utilizing image guided biopsy is justified to
determine relationship to direct patient benefit parameters (i.e. safety,
comfort, response, time to progression and survival).
Acknowledgements
We gratefully acknowledge the generous support of the Be the Difference Foundation, the Wilson Charitable Foundation Trust, the Joe and Jessie Crump Foundation Medical Research Fund, the Helen L. Kay Charitable Trust, The Marilyn Augur Family Foundation, Summerfield G. Roberts Foundation and Young Texans Against Cancer.The authors would like to acknowledge Brenda Marr and Michelle Richey for their competent and knowledgeable assistance in the preparation of the manuscript.
Disclosure/Conflict of Interest
The following authors are shareholders in Gradalis, Inc. and Strike Bio: Gladice Wallraven, Padmasini Kumar, Nicolas Taquet, Jonathan Oh, Donald D. Rao, Beena O. Pappen, Neil Senzer and John Nemunaitis. The authors have no other relevant affiliations or financial involvement with any organization or entity with a financial interest in or financial conflict with the subject matter or materials discussed in the manuscript.
References
- Senzer N, Barve M, Kuhn J, Melnyk A, Beitsch P, Lazar M, et al. Phase I trial of "bi-shRNAi(furin)/GMCSF DNA/autologous tumor cell" vaccine (FANG) in advanced cancer. Mol Ther. 2012;20(3):679-86.
- Senzer N, Barve M, Nemunaitis J, Kuhn J, Melnyk A, Beitsch P, et al. Long Term Follow Up: Phase I Trial of “bi-shRNA furin/GMCSF DNA/Autologous Tumor Cell” Immunotherapy (FANG™) in Advanced Cancer. Journal of Vaccines and Vaccination. 2013;4(8):209.
- Jiang Y, Li Y, Zhu B. T-cell exhaustion in the tumor microenvironment. Cell Death Dis. 2015;6:e1792.
- Nemunaitis J, Barve M, Orr D, Kuhn J, Magee M, Lamont J, et al. Summary of bi-shRNA/GM-CSF augmented autologous tumor cell immunotherapy (FANG) in advanced cancer of the liver. Oncology. 2014;87(1):21-9.
- Ghisoli M, Barve M, Mennel R, Lenarsky C, Horvath S, Wallraven G, et al. Three-year Follow up of GMCSF/bi-shRNA(furin) DNA-transfected Autologous Tumor Immunotherapy (Vigil) in Metastatic Advanced Ewing's Sarcoma. Mol Ther. 2016;24(8):1478-83.
- Oh J, Barve M, Matthews CM, Koon EC, Heffernan TP, Fine B, et al. Phase II study of Vigil® DNA engineered immunotherapy as maintenance in advanced stage ovarian cancer. Gynecol Oncol. 2016;143(3):504-510.
- Barve M, Kuhn J, Lamont J, Beitsch P, Manning L, Pappen B, et al. Follow-up of bi-shRNA furin / GM-CSF Engineered Autologous Tumor Cell (EATC) Immunotherapy Vigil® in Patients with Advanced Melanoma. Biomedical Genetics and Genomics. 2016;1(3):81-86.
- Schumacher TN, Schreiber RD. Neoantigens in cancer immunotherapy. Science. 2015;348(6230):69-74.
- Castle JC, Kreiter S, Diekmann J, Lower M, van de Roemer N, de Graaf J, et al. Exploiting the mutanome for tumor vaccination. Cancer Res. 2012;72(5):1081-91.
- Gubin MM, Artyomov MN, Mardis ER, Schreiber RD. Tumor neoantigens: building a framework for personalized cancer immunotherapy. J Clin Invest. 2015;125(9):3413-21.
- Lu YC, Robbins PF. Targeting neoantigens for cancer immunotherapy. Int Immunol. 2016;28(7):365-70.
- Nemunaitis J, Dillman RO, Schwarzenberger PO, Senzer N, Cunningham C, Cutler J, et al. Phase II study of belagenpumatucel-L, a transforming growth factor beta-2 antisense gene-modified allogeneic tumor cell vaccine in non-small-cell lung cancer. J Clin Oncol. 2006;24(29):4721-30.
- Santarpia M, Gonzalez-Cao M, Viteri S, Karachaliou N, Altavilla G, Rosell R. Programmed cell death protein-1/programmed cell death ligand-1 pathway inhibition and predictive biomarkers: understanding transforming growth factor-beta role. Transl Lung Cancer Res. 2015;4(6):728-42.
- Soares KC, Rucki AA, Kim V, Foley K, Solt S, Wolfgang CL, et al. TGF-beta blockade depletes T regulatory cells from metastatic pancreatic tumors in a vaccine dependent manner. Oncotarget 2015;6(40):43005-15.
- Wei H, Liu P, Swisher E, Yip YY, Tse JH, Agnew K, et al. Silencing of the TGF-beta1 gene increases the immunogenicity of cells from human ovarian carcinoma. J Immunother. 2012;35(3):267-75.