Research Article
Renal Cell Carcinoma with Level IV Cavo-Atrial Thrombus: Short Term and Long Term Outcomes
Rajendra B Nerli*
Department of Urology, KLES Dr Prabhakar Kore Hospital & MRC, Belgaum, Karnataka, India
*Corresponding author: Rajendra B Nerli, Department of Urology, KLES Kidney Foundation, KLE University’s JN Medical College, KLES Dr Prabhakar Kore Hospital & MRC, Belgaum, Karnataka, India
Published: 16 Mar, 2017
Cite this article as: Nerli RB. Renal Cell Carcinoma with
Level IV Cavo-Atrial Thrombus: Short
Term and Long Term Outcomes. Clin
Oncol. 2017; 2: 1219.
Abstract
Introduction: With the technological advances surgical treatment of Renal Cell Carcinoma with
a level IV Cavo-Atrial Thrombus is now feasible, and the thrombus can almost always be removed
successfully. Patients with level IV Inferior Vena Caval thrombus can be treated safely and effectively
via radical nephrectomy and thrombectomy using Cardiopulmonary Bypass combined with Deep
Hypothermic Circulatory arrest.
Materials and Methods: During the study period, 20 patients (16 male and 4 female) underwent
surgery for RCC with IVC tumor thrombus extending into the right atrium. Preoperative workup
included chest, abdomen and pelvis CT scan, and Magnetic Resonance Imaging (MRI). Following
surgery all of the patients were followed up with a complete blood serum chemistry panel, chest
X-ray and abdominal CT.
Results: A total of 20 patients with mean (SD) age of 49.65 ± 10.32 years underwent radical
nephrectomy with IVC thrombectomy. Preoperatively all these patients were diagnosed to have a
T3cN0M0 RCC on clinical and radiological imaging. The mean (SD) operating time was 247.25 ±
40.08 mins, and the mean (SD) hypothermic circulatory arrest time was 17.25 ± 1.48 mins at a mean
core temperature of 20.4 ± 2.8°C. In a mean follow of 40.85 months, malignancy was the cause of
death in 9 of these patients, whereas five other patients died of causes unrelated to RCC and six
patients are still alive postoperatively. The median survival after the operation was 31.5 months.
Conclusion: Patients with level IV IVC thrombus RCC can be treated safely and effectively via
radical nephrectomy and thrombectomy using CPB combined with DHCA. This approach is
associated with low rates of morbidity and mortality.
Keywords: Cardiopulmonary bypass; Hypothermic arrest; Renal cell carcinoma; Thrombectomy; Tumor thrombus
Introduction
Formation of tumor thrombus and venous migration are unique to Renal Cell Carcinoma
(RCC) [1] with significant therapeutic and prognostic implications [2]. IVC (Inferior Vena Cava)
thrombus occurs in 4% to 10% of patients with renal cell carcinoma [3] of which 2% to 16% are
known to extend into the right atrium [4]. The tumor thrombus is known to invade the caval wall
which is however difficult, if not impossible, to predict preoperatively [1]. The intravascular growth
observed in RCC patients could signify a heightened or more aggressive biologic behaviour of the
tumor. Several experts agree that the RCC associated tumor thrombus does not translate to a specific
prognostic significance if it can be treated successfully with surgery [5]. Radical nephrectomy
together with thrombectomy is the only effective therapeutic option for these patients [6,7]. Surgical
management of RCC in which there is extension into the renal vein, IVC, or even the right atrium,
however, poses a significant technical challenge [8].
Several contemporary studies have demonstrated that tumor thrombus has a limited prognostic
role in the absence of nodal and/or metastatic disease and that about 45% to 70% of cases can be
cured with surgical extirpation [2,9]. While others have shown that the prognosis of RCC with IVC
thrombi is generally poor with 5 year survival rates about 25% to 57%, despite surgical resection of
RCC and tumor thrombus [2,10]. Reported operative mortality rates range between 2.7% to 13%
[11]. The major causes of death being pulmonary embolism and myocardial infarction or due to
complications related to the bypass procedures. However, with better perioperative management
and standardization of the surgical techniques, the mortality rates have decreased considerably [4].
In the present study, we have retrospectively reviewed our management of RCC cases with level IV thrombi using the Cardiopulmonary bypass with deep hypothermic
circulatory arrest approach. We have analysed our data to assess short
and long term outcomes.
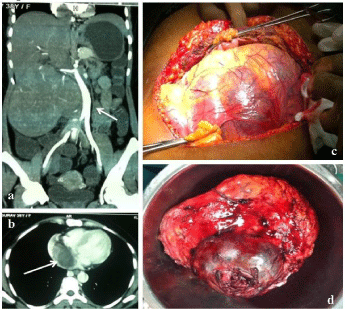
Figure 1
Figure 1
a) CT abdomen revealing a huge right renal tumor, pushing the
great vessels to the left side. IVC thrombus extending from bifurcation of IVC
to the right atrium. b) CT (Transverse section) showing thrombus occupying
the right atrium. c) Abdomen explored with B/L Chevron incision. Photograph
showing the huge right renal tumor. d) Excised renal tumor.
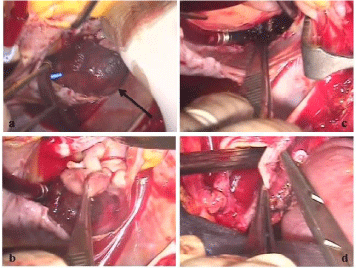
Figure 2
Figure 2
a) Thrombus seen occupying a huge portion of right atrium. b)
Thrombus being dissected and removed from the right atrium. c) Right atrium
after removal of thrombus. d) Right atrium being closed.
Patients and Methods
During the period Jan 1996 to Dec 2015, 20 patients (16 male
and 4 female) underwent surgery for RCC with IVC tumor thrombus
(level IV) extending into the right atrium. Preoperative workup
included chest, abdomen and pelvis CT scan, abdominal ultrasound
with color-Doppler, and Magnetic Resonance Imaging (MRI) (Figure
1). Magnetic resonance imaging was done to determine the exact
cephalad extent of the inferior vena cava thrombus. Loco-regional
and metastatic extension was evaluated in all cases by brain and chest
CT-scan, bone scan and hepatic ultrasound.
Surgical techniques
Trans-Esophageal Echocardiography (TEE) was performed at
the beginning of the surgical procedure in all patients to confirm
the level of the upper extent of the thrombus. TEE was continued
throughout the operation to detect air or tumor embolisms, and to check complete extraction of the thrombus. The abdomen was
entered through a bilateral chevron incision and extended through a
median sternotomy. The right colon and small bowel were mobilized
along the white line of Toldt and small bowel mesentery, exposing the
anterior surface of the inferior vena cava and both the renal veins. The
involved kidney was dissected from all the sides and the renal artery
ligated. Infra-renal IVC and contralateral renal vein were clamped
using a tourniquet. The patient was placed in the Trendelenberg
position to decrease the risk of air embolism. The renal vein on
the affected side was ligated and the nephrectomy was completed.
Further the patient was heparinised and cannulation was performed.
The right atrium was cannulated with minimal handling and avoiding
the tumour thrombus. A low profile ‘Ross basket’ cannula was
inserted into the right atrial appendage. Cardiopulmonary Bypass
(CPB) was commenced and the patient was systematically cooled to
a core temperature of 230C to 250C. After the required temperature
was attained, the patient was placed in Trendelenberg position. A
separate atriotomy was made almost to the level of the diaphragm
to allow complete visualization (Figure 2). The intra-abdominal IVC
was simultaneously opened. The thrombus was gently manipulated
and separated from the IVC, hepatic veins and Right Atrium (RA).
The ‘tumour waist’ at the level of the diaphragm required careful
manipulation to deliver the tumour tissue into the abdominal IVC.
Another area of concern was the hepatic veins, which contained
‘tongues’ of tumour tissue and required exploration under vision via
the RA to extricate. This was further aided by the use of Fogarty’s
embolectomycatheter. The thrombectomy was completed. The
cavotomy and atriotomy were then closed with continuous
polypropylene sutures. Cardiopulmonary bypass was reversed, aortic
clamp removed and the patient was rewarmed. All of the patients
were followed up with a complete blood serum chemistry panel, chest
X-ray and abdominal CT at 6 monthly intervals postoperatively.
Bone scans were done whenever necessary. All hospital charts and
follow-up information was obtained by contacting the patients
and/or their attenders. Complete follow-up was available for all the
patients. Cancer free status was determined by negative findings on
the aforementioned studies. Survival analysis was calculated and the
mean survival reflected the interval to last follow-up in patients still
alive or to death.
Results
During the study period of eighteen years, 28 patients with RCC
and level IV cavo-atrial thrombus presented to the uro-oncological
services of the hospital. Of these a total of 20 patients with mean (SD)
age of 49.65 ± 10.32 years underwent radical nephrectomy with IVC
thrombectomy. Twelve had RCC on the right side and the remaining
eight had on the left side. All these patients had a T3cN0M0 RCC
on clinical and radiological imaging. Preoperative evaluation in these
patients showed that, hepatic enzymes and serum bilirubin was raised
in three patients, two other patients had raised serum creatinine levels
and all the 20 patients were anemic. Minimal ascites was noted in
three patients and prominent veins over abdomen were visible in 13
of the patients. Pre-operative blood transfusion was necessary in five
patients. Following discussions with the cardiothoracic team, it was
decided to perform the surgery using cardio-pulmonary bypass and
instituted hypothermic circulatory arrest. All patients were started on
heparin preoperatively. The mean (SD) operating time was 247.25 ±
40.08 mins, and the mean (SD) hypothermic circulatory arrest time
was 17.25 ± 1.48 mins at a mean core temperature of 20.4 ± 2.80C.
Complete removal of the tumour thrombus was accomplished in all patients within the period of circulatory arrest. Post-operative blood
loss was <650 ml in all but three patients.
The histological types were: clear cell RCC in 17 cases (Fuhrman
nuclear grade II in two, grade III in fourteen, and grade IV in
one), papillary RCC in two cases (Fuhrman nuclear grade III),
and Primitive neuroectodermal tumor in one case. Perinephric fat
involvement (T4) was seen in four patients and hilar lymph nodes
(N1) were positive for tumor in five. None of the patients died during
the period of hospitalization. Two patients were re-explored within 8
hours for post-operative bleeding. The bleeding was noticed from the
pericardium in one and the internal mammary vessels in the other.
Post-operative blood transfusions were necessary in three patients.
The mean intensive care and hospital stay was 3.0 and 14.5 days
respectively. Immediate postoperative complications were as shown
in (Table 1). The raised preoperative hepatic parameters in three
patients gradually returned to normal in the postoperative period.
Serum creatinine which was raised in two patients preoperatively
similarly showed decline, but not to normal levels. In a mean follow of
40.85 months (range 16 - 90), malignancy was the cause of death in 9
of these patients, whereas five other patients died of causes unrelated
to RCC which included myocardial infarction (3), cerebrovascular
accident (1) and road traffic accident (1). Six patients are still alive
at 21, 33, 39, 42, 55 and 65 months postoperatively (median 40.5 and
mean 42.5 months). The median survival after the operation was
31.5 months. Survival proportion of the whole cohort is shown in a
Kaplan–Meier plot (Figure 3) with 2 survival rate of 98 percent and 5
year survival rate of 57 percent.
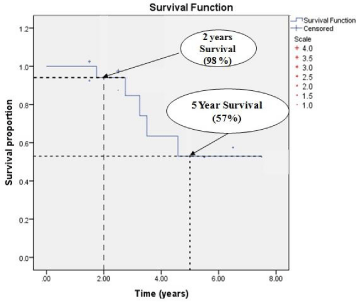
Figure 3
Figure 3
Survival proportion of the whole cohort is shown in a Kaplan–Meier
plot with 2 survival rate of 98 percent and 5 year survival rate of 57 percent.
Discussion
Today radical surgery remains the mainstay of curative treatment
for RCC (Renal Cell Carcinoma). Progression of a tumour thrombus
into the inferior vena cava (IVC) makes surgery all the more
challenging. Clinically, four levels of thrombus extension into the
IVC have been defined by Nesbitt et al. [4]. In level IV, the thrombus
extends above the diaphragm into the right atrium, and the operating
uro-oncological team would need the help of the cardiothoracic
surgeons. Due to the scarcity of these operations, usually only case
reports or small series with short follow-up have been published
to date. Venous involvement was once thought to be a very poor
prognostic finding for RCC, but several reports demonstrate that many patients with tumor thrombi can be salvaged with an aggressive
surgical approach. These studies document 45% to 69% 5-year survival
rates for patients with venous tumor thrombi as long as the tumor is
otherwise confined to the kidney [12,13]. Patients with venous tumor
thrombi and concomitant lymph node or systemic metastases have
markedly decreased survival, and those with tumor extending into
the perinephric fat have intermediate survival [13,14]. The prognostic
significance of the cephalad extent of tumor thrombus appears to be
controversial, and it is difficult to compare various series because of
selection biases and related co-variables [14]. In several series the
incidence of advanced loco regional or systemic disease increased
with the cephalad extent of the tumor thrombus, accounting for
the reduced survival associated with tumor thrombus extending
into or above the level of the hepatic veins [14,15]. However, other
data suggest that the cephalad extent of tumor thrombus is not of
prognostic significance as long as the tumor is otherwise confined
[13]. Direct invasion of the wall of the vein appears to be a more
important prognostic factor than level of tumor thrombus and is now
classified as pT3c independent of the level of tumor thrombus [13-
16]. Involvement of the IVC with RCC renders the task of complete
surgical excision more complicated; however this approach offers the
only realistic hope for cure for most patients. Vascular control for
level III and level IV IVC thrombi requires more extensive dissection,
venovenous bypass, or cardiopulmonary bypass and hypothermic
circulatory arrest. Level IV IVC thrombi have traditionally been
managed with Cardiopulmonary Bypass (CPB) and Hypothermic
Circulatory Arrest (HCA), and this is still the preferred approach
in complex cases [13-15]. Several centers are now trying to avoid
hypothermic circulatory arrest and the associated hypocoagulable
state that ensues after coming off the pump and the increased risk of
cerebrovascular accident and myocardial infarction that accompanies
this procedure [7,13]. In this case the thrombus is mobilized below
the atrium, allowing sequential vascular control to be achieved
without opening the heart.
Chen, et al. [17] performed a retrospective analysis on 32 RCC
patients with IVC thrombus that underwent nephrectomy and
thrombectomy via the minimally invasive CPB/HCA approach. The
median operation time was 360 min (Inter Quartile Range (IQR):
300 to 435 min) with median CPB and HCA durations of 149 min
and 23 min, respectively. The median estimated blood loss was 2,500
ml. Four complications were observed but no deaths occurred perioperatively.
The median follow-up was 25 months (range: 4 to 64
months). The mean Overall Survival (OS) was 28.2 ± 4.6 months
while the Disease-Free Survival (DFS) was 19.5 ± 11.6 months. In
patients with M0 disease, ten patients developed metastases and were
treated with sorafenib as an adjuvant therapy. The mean OS and DFS
of this subgroup were 25.4 ± 12.8 months and 16.0 ± 14.2 months,
respectively. Dominik et al. [18]. evaluated long-term results of
surgical management of renal cell carcinoma with level IV tumour
thrombus in a large single institution series. Radical nephrectomy was
performed followed by sternotomy, institution of cardiopulmonary
bypass and extraction of the intracardiac tumour thrombus under
direct visual control during Deep Hypothermic Circulatory Arrest (DHCA). The mean (SD) duration of circulatory arrest was 16 ± 6min
at a mean hypothermia of 20 ± 3°C. In-hospital mortality was 9.5%.
The median survival (including in-hospital mortality) was 25 months.
In Kaplan–Meier analysis, 2 and 5-year overall cumulative survival
rate was 57 (95% confidence interval, CI 36–78) % and 37 (95% CI 15–
58) %, respectively. Cancer-specific cumulative survival was 68 (95%
CI 49–89)% at 2 years and 51 (95% CI 28–74) % at 5 years. Similarly
Nerli et al. [15]. Assessed the short term and long term survival of 7
patients with level IV thrombus who underwent surgical treatment
for localized RCC and inferior vena caval thrombus extending into
the right atrium using Cardiopulmonary Bypass (CPB) and deep
hypothermic circulatory arrest. Pathological investigations revealed
no renal capsular penetration of RCC in 4 patients and perinephric
fat involvement in 3. The mean operating time was 365 min (295-
390), anesthesia time was 395 min (335-440), cardiopulmonary
bypass time was 128 min (38-200) and hypothermic circulatory
arrest time was 28 min (14-38). The mean follow-up time was 38
months. Presence of capsular infiltration or positive lymph nodes
significantly affected survival of patients, with no patient having a
two year survival as opposed to 100% in patients with no capsular
infiltration. The authors concluded that long term survival following
the surgical treatment was possible in individuals with localized RCC
extending into the right atrium. Performance of complete radical
nephrectomy along with vena caval thrombectomy under circulatory
arrest was safe and without significant morbidity. Chowdhury et al.
[19]. Described an alternative technique of vena caval and intraarterial
tumor thrombectomy to decrease perioperative mortality and
morbidity. Radical nephrectomy with tumor thrombectomy from the
vena cava and right atrium was performed under mild hypothermic
cardiopulmonary bypass and intermittent cross-clamping of the
supraceliac abdominal aorta. Interatrial tumor thrombectomy
was performed on a beating, perfused heart in 4 patients and a
hypothermic, cardioplegia-perfused heart in 2 patients. The aortic
cross-clamp time was 12 and 15 minutes for two patients respectively.
The cumulative hepatic and renal ischemic time was 16 minutes
(range, 14 to 22 minutes) at 32°C. The mean cardiopulmonary bypass
time was 53.3 ± 8.9 minutes (range, 40 to 65 minutes). At a mean
follow-up of 43 ± 24.6 months (range, 10 to 70 months), all patients
were active and remained disease-free. Modine et al. [20]. Reported
on their early experience with a simplified CPB technique, wherein
the right atrium thrombus was extracted under normothermic
CPB without cross clamping or cardioplegic arrest. A cavotomy
was performed at the ostium of the renal vein and an endoluminal
occlusion catheter was introduced to perform the thrombectomy.
Atrial and caval thrombectomy were achieved successfully. Currently,
better surgical results than those published can be expected because
of the enormous improvement in perioperative and postoperative
care. A risk of 5–10% can currently be hypothesized for an operation
with the use of DHCA in patients with RCC/level IV cavo-atrial
thrombus [18]. Long-term results are of equal importance and also
justify the correctness of such a complex and demanding surgical
procedure needed to treat these level IV IVC thrombus. In a
retrospective study including 1192 patients operated for RCC with
tumour thrombus between 1982 and 2003 at 13 European institutions
[21], the median survival was only 18 months for 63 patients with
supra-diaphragmatic tumour thrombus. Independent prognostic
factors in multivariate analysis were tumoursize, perinephric fat
invasion, lymph node invasion, tumour thrombus level and distant
metastasis [21]. There was no improvement in postoperative survival
of patients with multiple distant metastases when compared with the
natural history of untreated RCC [22]. In another multi-institutional
study that collected retrospective data from 11 USA and European
academic institutions between 1970 and 2006 [23], 77 patients had
tumour thrombus extending into the right atrium; with median
survival time of 12 months and 22% 5-year cumulative survival. In a
multivariate analysis, tumour size, Fuhrman grade, nodal metastasis
and tumour thrombus level correlated independently with the
survival. Mohammed Nouh et al. [24] has made a suggestion about
angioscopic removal of such tumor thrombi under direct vision.
Such an endoscopic removal of the tumor thrombi could provide
several advantages. At first, it would allow direct visualization of
the tumor thrombi and the caval lumen throughout the technique.
Secondly, it would avoid the aggressive time-consuming dissection
of IVC from the posterior abdominal wall and liver mobilization
with their surgical consequences. Thirdly, it would allow removal of
thrombi in a relatively bloodless field. Fourth, it would reduce the
length of incision and soft-tissue dissection. Fifth, it would avoid the
complicated techniques and the surgical consequences of CPB and
DHCA.
Table 1
Conclusion
Patients with level IV IVC thrombus RCC can be treated safely and effectively via radical nephrectomy and thrombectomy using CPB combined with DHCA. This approach is associated with low rates of morbidity and mortality.
References
- Ciancio G, Soloway M. Resection of the abdominal IVC for complicated renal cell carcinoma with tumor thrombus. BJU Int. 2005; 96: 815-818.
- Zisman A, Wieder JA, Pantuck AJ, Chao DH, Dorey F, Said JW, et al. Renal cell carcinoma with tumor thrombus extension: biology, role of nephrectomy and response to immunotherapy. J Urol. 2003; 169: 909-916.
- Mootha RK, Butler R, Laucirica R. Renal cell carcinoma with infra-renal vena caval tumor thrombus. Urology. 1999; 54: 561-565.
- Nesbitt JC, Soltero ER, Dinney CP, Walsh GL, Schrump DS, Swanson DA, et al. Surgical management of renal cell carcinoma with IVC tumor thrombus. Ann ThoracSurg. 1997; 63: 1592–600.
- Bachmann A, Seitz M, Graser A, Reiser M F, Schafers H J, Lohe F, et al. Tumour nephrectomy with vena cava thrombus. BJU Int. 2005; 95: 1373-1384.
- Bertini R, Roscigno M, Lapenna E, Pasta A, Petralia G, Strada E, et al. Radical nephrocapsulectomy and cavalthrombectomy with extracorporeal circulation and deep hypothermic circulatory arrest in right anterior minithoracotomy: a minimally invasive approach. Urology. 2008; 71: 957-961.
- Subramanian VS, Stephenson AJ, Goldfarb D A, Fergany AF, Novick AC, Krishnamurthi V. Utility of preoperative renal artery embolization for management of renal tumors with inferior vena caval thrombi. Urology. 2009; 74: 154-159.
- Kirkali Z, Van Poppel H. A critical analysis of surgery for kidney cancer with vena cava invasion. Eur Urol. 2007; 52: 658-662.
- Wszolek MF, Wotkowicz C, Libertino JA. Surgical management of large renal tumors. Nat Clin Pract Urol. 2008; 5: 35–46.
- Kim HL, Zisman A, Han KR, Figlin RA, Belldegrun AS. Prognostic significance of venous thrombus in renal cell car- cinoma. Are renal vein and inferior vena cava involvement different? J Urol. 2004; 171: 588-591.
- Terakawa T, Miyake H, Takenaka A, Hara I, Fujisawa M. Clinical outcome of surgical management for patients with renal cell carcinoma involving the inferior vena cava. Int. J Urol. 2007; 14: 781-784.
- Campbell S, Lane B R, Wein AJ, Kavoussi L R, Novick A C, Partin AW, et al. Ed Campbell-Walsh Urology, Elsevier- Saunders, Philadelphia. 2012; 1413-1474.
- WotkowiczC, Libertino JA, Sorcini A, Mourtzinos A. Management of renal cell carcinoma with vena cava and atrial thrombus: minimal access vs median sternotomy with circulatory arrest. BJU Int. 2006; 98: 289-297.
- NerliR B, Dixit, Gan M, Vikram P, Shishir D, Hiremath MB. Renal Cell Carcinoma with Vena Caval Thrombus Extending into the Right Atrium: Our Experience. Int J Nephrol Urol. 2010; 2: 497-503.
- Zini L, Destrieux-GarnierL, Leroy X, Villers A, Haulon S, Lemaitre L, et al. Renal Vein Ostium Wall Invasion of Renal Cell Carcinoma With an Inferior Vena Cava Tumor Thrombus: Prediction by Renal and Vena Caval Vein Diameters and Prognostic Significance . J Urol. 2008; 179: 450-454.
- Chen YH, Wu XR, Hu ZL, Wang WJ, Jiang C, Kong W, et al. Treatment of renal cell carcinoma with a level III or level IV inferior vena cava thrombus using cardiopulmonary bypass and deep hypothermic circulatory arrest. World J Surg Oncol. 2015; 13: 159.
- Dominik J, Moravek P, Zacek P, Vojacek J, Brtko M, Podhola M, et al. Long-term survival after radical survival after surgery for renal cell carcinoma with tumor thrombus extension into the right atrium. BJU Int. 2012; 111: E59-E64.
- 18. Chowdhury UK, Mishra AK, Seth A, Dogra PN, Honnakere JH, Subramaniam GK, et al. Novel techniques for tumor thrombectomy for renal cell carcinoma with intraatrial tumor thrombus. Ann Thorac Surg. 2007; 83: 1731-1936.
- Modine T, Haulon S, Zini L, Fayad G, Destrieux-Garnier L, AzzaouiR, et al. Surgical treatment of renal cell carcinoma with right atrial thrombus: Early experience and description of a simplified technique. Int J Surg. 2007; 5: 305-310.
- Wagner B, Patard JJ, Méjean A, Bensalah K, Verhoest G, Zigeuner R, et al. Prognostic value of renal vein and inferior vena cava involvement in in renal cell carcinoma. Eur Urol. 2009; 55: 452-459.
- Vogt PR, Ensner R, Pretre R. Less invasive surgical treatment of renal cell carcinomas extending into the right heart and pulmonary arteries: surgery for renal cell carcinoma. J Card Surg. 1999; 14: 330-333.
- Martinez-Salamanca J, Huang WC, Millan I. Prognostic impact of the 2009 UICC/AJCC TNM staging system for renal cell carcinoma with venous extension. Eur Urol. 2011; 59: 120–127.
- Nouh MA, Inui M, Kakehi Y. Renal Cell Carcinoma with IVC Thrombi; Current Concepts and Future Perspectives. J Clin Oncol. 2008; 2: 247-256.