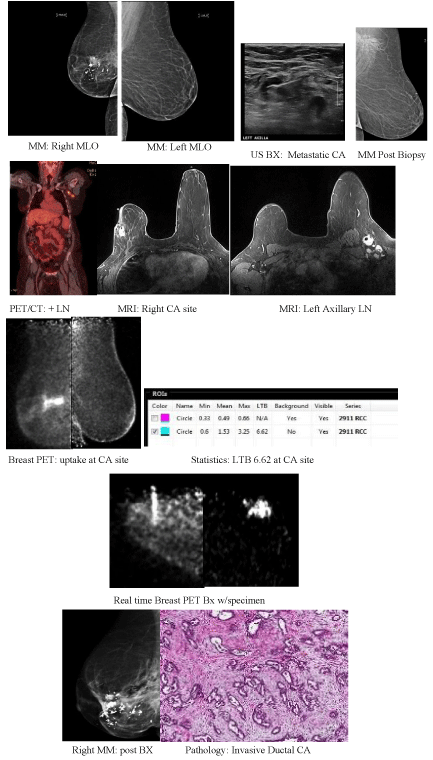
Clinical Image
Clinical Benefit of High Resolution Breast PET
Maria Victoria Velasquez and Kathy Schilling*
Christine E. Lynn Women's Health & Wellness Institute, Boca Raton Regional Hospital, Boca Raton, Florida, USA
*Corresponding author: Kathy Schilling, Christine E. Lynn Women's Health & Wellness Institute, Boca Raton Regional Hospital, Boca Raton, Florida, USA
Published: 17 Feb, 2017
Cite this article as: Velasquez MV, Schilling K. Clinical
Benefit of High Resolution Breast PET.
Clin Oncol. 2017; 2: 1207.
Clinical Image
Anatomic breast imaging techniques are very useful in the detection of breast cancer, but
can have limited sensitivity and positive predictive value [1]. These limitations have provided the
incentive for adjunctive metabolic technologies such as high-resolution breast PET. Metabolic or
functional imaging focuses on activity at the cellular level and can provide more precise information
and often better differentiation between benign vs. malignant findings.
Since its inception little more than a decade ago high-resolution, breast specific, PET imaging
has proven to be an invaluable clinical asset, particularly in complex case problem solving. The
instrumentation design of the Naviscan Solo-II™ high resolution PET scanner consists of a
pair of linear detector arrays with LYSO crystal scintillators coupled with position sensitive
photomultipliers. High-resolution breast PET utilizes tomographic reconstruction and uniform
high spatial resolution with increasing tumor depth. Multiple reiterative reconstruction and postreconstruction
filtering contribute to lesion conspicuity.
In addition to the high intrinsic spatial resolution (1.6 mm), sensitivity (92.5%), and specificity
(91.2%) [2], the ability to conduct real-time, guaranteed sampling of suspicious lesions through core
imaging verification provides an unprecedented advantage for breast biopsy [3,4].
As experienced dedicated breast imagers, we are always looking for advancements that can help
promote a more personalized approach to breast cancer diagnosis and treatment versus a one-sizefits-
all strategy. We have employed high-resolution breast PET for over 7 years, convinced of its
efficacy we use it as an ancillary option for many problematic cases. One such case is discussed here.
At just 35 years of age, this patient was initially diagnosed with poorly differentiated invasive
ductal carcinoma of the right breast. After treatment with lumpectomy, chemotherapy, and
radiation therapy the patient was returned to routine surveillance screening. Nine years later, she
suffered a recurrence in the right breast. Another lumpectomy and re-excision for positive margins
were performed. Once again, post-surgery the patient resumed routine imaging surveillance. Fast
forward another seven years. The patient presented with clinically enlarged lymph nodes on the
contralateral (left) side. Diagnostic imaging work up to include mammography, ultrasound, PET/
CT, and MRI were all performed. All modalities revealed abnormal lymph nodes, only MRI showed
enhancement at the previous right breast site. The patient underwent left node biopsy and ultimately
ALND on the left which proved she had recurrent, locally metastatic adenocarcinoma, Estrogen,
Progesterone and HER 2 negative. MR-guided biopsy of the prior right lumpectomy site was done
and the results were negative yielding only fat necrosis and fibrosis. The primary lesion associated
with the left lymphadenopathy could not be found. After consultation with oncology, we decided to
try high-resolution breast PET. Finally, the answer was revealed. Active tumor in the right breast,
with a PUV max of 3.25 and a lesion to background ratio (LTB) of 6.2 and metastasis to contralateral
axillary lymph nodes. The imaging diagnosis was confirmed through PEM-guided biopsy of the
right breast with the ability to confirm location accuracy through imaging the activity in core
samples. The post- biopsy mammogram showed the biopsy marker for the PEM guided biopsy in
the expected location but the clip from the MR- guided biopsy was distant from the lesion site.
Same-day PEM-guided biopsy is feasible for most patients. It results in decreased radiation dose
to both the patient and medical staff and expedites the patient’s preoperative staging workup for
breast cancer. The feasibility and advantages of performing high-resolution PET imaging and PEMguided
biopsy on the same day are well documented [5]. The ability to perform real-time image
guided biopsy with the ability to confirm specimen sample activity is an unprecedented clinical
benefit. This case demonstrates correct sampling proven by activity in specimen imaging. The post
PET biopsy mammogram image also shows that the clip placed on the MR guided biopsy was far
distant from the actual cancer site.
The radiology community at large has expressed confidence
in the value of using high-resolution PET imaging of the breast to
improve detection and diagnosis [6]. At our center we have seen
first-hand the accuracy of this modality and the benefit it provides
to patients. Patient care is improved by accurately identifying the
extent of disease so appropriate management can be assessed. Breast
surgeons can appreciate the precise information provided for presurgical
planning.
Interest in nuclear breast imaging has increased significantly with
the advancement of dedicated devices with improved technological
capabilities that allow extremely high sensitivity and specificity at very low dose. Breast density notification laws have also contributed
to the debate and highlighted the need for functional vs. anatomic
breast imaging methods.
Encouraging work is underway with many radiotracers not
currently approved for use in the United States. 18F-fluoroestradiol
may have a role in predicting early response to treatment in the breast
[7]. With initial flare in responders, 3’-deoxy-3’-18F-fluorothymidine
(18F-FLT) is also being assessed in treatment response [8]. New
pathways in radiotracer development only broaden the horizon for
high-resolution breast PET.
Individualized assessment is a key component of our practice.
By having multiple modalities at our disposal we can maximize early
detection which decreases interval cancer rate. Patients need a more
tailored approach to diagnosis and treatment. We feel that functional
imaging with high-resolution breast PET can play a major role in that
paradigm.
Figure
References
- Kolb TM, Lichy J, Newhouse JH. Comparison of the Performance of Screening Mammography, Physical Examination, and Breast US and Evaluation of Factors that Influence Them: an Analysis of 27,825 Patient Evaluations. Radiology. 2002; 225: 165-175.
- Berg WA, Madsen KS, Schilling K, Tartar M, Pisano ED, Larsen LH, et al. Comparative Effectiveness of Positron Emission Mammography and MRI for Presurgical Planning of the Ipsilateral Breast in Women with Breast Cancer. Radiology. 2011; 258: 59-72.
- Lu X, Anashkin E, Matthews CG, Luo W. Real- Time Viewer for PEM Guided Biopsy. IEEE Transactions on Nuclear Science. 2010; 57: 1139-1145.
- Kalinyak JE, Schilling K, Berg WA, Narayanan D, Mayberry JP, Rai R, et al. PET Guided Breast Biopsy. Breast J. 2011; 17: 143-151.
- Argus A, Mahoney MC. Positron Emission Mammography: Diagnostic Imaging and Biopsy on the Same Day. AJR Am J Roentgenol. 2014; 202: 216–222.
- Greene LR, George RF. Radiologists Views on Positron Emission Mammography. Radiol Technol. 2012; 84: 18-30.
- Linden HM, Stekhova SA, Link JM, Gralow JR, Livingston RB, Ellis GK, et al. Quantitative fluoroestradiol positron emission tomography imaging predicts response to endocrine treatment in breast cancer. J Clin Oncol. 2006; 24: 2793–2799.
- Kong FL, Kim EE, Yang DJ. Targeted nuclear imaging of breast cancer: status of radiotracer development and clinical applications. Cancer Biother Radiopharm. 2012; 27: 105–112.