Case Report
The Goal of a Trifecta in Treatment Strategy for Bilateral Synchronous Testicular Seminoma: A Case Report and Literature Review
Richmond A Owusu1, Kanenori Okamoto BS2, Brett M Lowenthal3 and Tung-Chin Hsieh1*
1Department of Urology, UC San Diego Health, USA
2Department of Urology, UC San Diego School of Medicine, USA
3Department of Pathology, UC San Diego Health, USA
*Corresponding author: Tung-Chin Hsieh, Department of Urology, UC San Diego Health, USA
Published: 13 Feb, 2017
Cite this article as: Owusu RA, Kanenori Okamoto BS,
Lowenthal BM, Hsieh T-C. The Goal
of a Trifecta in Treatment Strategy
for Bilateral Synchronous Testicular
Seminoma: A Case Report and
Literature Review. Clin Oncol. 2017; 2:
1203.
Abstract
The most common testicular tumors among young men of reproductive age are Germ Cell Tumors (GCTs). Luckily, these tumors are very treatable with high survival rates. However, some of the long term consequences on survivors such as sterility and hypogonadism do not garner as much attention, given that the majority of tumors are unilateral. In the rare cases of bilateral testicular tumors, treatment consequences have more profound effect on quality of life and should garner serious consideration in devising a treatment strategy for these patients. Here, we report a case of bilateral synchronous seminoma found in a patient managed with a fertility-sparing surgical treatment strategy.
Introduction
The most common solid neoplasms among young men of reproductive age are testicular tumors, peaking in the age range of 20-39 [1,2]. Testicular tumors occur bilaterally with an incidence of 1-5% [3-6]. The standard of care for patients with a bilateral presentation is bilateral radical orchiectomy. However, anorchia results in sterility and hypogonadism requiring lifelong testosterone replacement, it is of interest to physicians and patients to explore fertility-sparing strategies for this subset of men. The aim of this case report is to provide as updated review of literature and to propose a new goal for management of bilateral testicular tumors aimed at achieving a trifecta of good oncologic outcome with fertility and hormonal preservation in carefully selected patients.
Case Report
A 36 year old male was referred to the UC San Diego Urology Department for primary infertility
due to azoospermia and an incidentally discovered right testicular masses suspicious for malignancy.
The patient’s notable past medical history included right-sided cryptorchidism requiring orchiopexy
at age eleven. He denied any other known risk factors such as prior testicular exposure to chemicals,
radiation, or toxins, history of high fever, epididymitis, orchitis, prostatitis, sexually transmitted
diseases, trauma to the testes, varicoceles, testicular torsion, post-pubertal mumps, or family history
of infertility. He had a palpable intra-testicular mass on the right and normal exam on the left.
Tumor markers included elevated beta human chorionic gonadotropin (β-HCG88 IU/L) with
alpha-fetoprotein and lactate dehydrogenase were within normal ranges (AFP <2ng/mL, LDH
191 Units/L). Scrotal sonogram revealed patient’s right testis mostly replaced by a heterogeneous
mass and left testis with 4mm hypoechoic intra-testicular nodule without vascularity located in the
inferior pole (Figure 1). Chest, abdomen and pelvic imaging were negative for metastatic disease.
Due to the patient’s desire to preserve fertility, testicular sparing procedure with concomitant sperm
extraction (TESE) was discussed for his left testicular lesion.
The patient underwent a right radical orchiectomy and a left partial orchiectomy after
intraoperatively confirming negative margins on frozen section. A concurrent successful left TESE
revealed viable sperm for cryopreservation. The patient’s post-operative course was uncomplicated.
The final histopathologic diagnosis revealed a 0.6 cm × 0.3 cm × 0.3 cm left testicular biopsy specimen
consistent with seminoma and a 3.7 cm × 2.6 cm × 2.3 cm pT1 right seminoma with negative spermatic cord
margins (Figure 2). Options of active surveillance with tumor markers, chemotherapy, and radiation
therapy were discussed with the patient. The patient elected surveillance until evidence of recurrence or after the couple achieve pregnancy and complete family planning.
At the time of this case report, the patient has not demonstrated any
evidence of recurrence and his post-operative hypogonadism is wellmanaged
with clomiphene citrate.
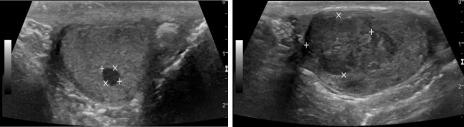
Figure 1
Figure 1
Scrotal ultrasound showing medial longitudinal view of the left testicle showing 0.48 x 0.37cm hypoechoic mass (left) and right testicle showing
heterogeneous testicular mass (right).
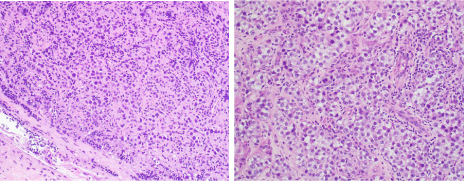
Figure 2
Figure 2
Histopathologic examination of the formalin fixed paraffin embedded and H&E stained left testicular biopsy specimen (left, 20x objective) and right radical
orchiectomy specimen (right, 20x objective). The sections show sheets of large, round polyhedral neoplastic cells with abundant clear cytoplasm, large central
nuclei and prominent irregular nucleoli. The tumor cells are in a poorly demarcated lobular architecture with delicate fibrous septa intimately associated with a
lymphoplasmacytic inflammatory infiltrate. There was rare mitotic figures and no necrosis identified. Overall, the findings are consistent with bilateral seminomas.
Discussion
Testicular GCTs remain one of the most treatable cancers, with
survival rates over 90% [7]. Much of that credit goes to platinum-based
chemotherapy that makes even widely metastatic disease treatable.
However, less attention is given to the long term effects of treatment
on these young testicular cancer survivors such as sexual dysfunction
and hypogonadism [7-9]. Given that GCTs present typically in young
males of reproductive age, this should be an important consideration.
The fact that even management of unilateral tumors still have such
treatments effects means bilateral synchronous or metachronous
presentations presents a unique challenges and special considerations
for specialists in urologic oncology and male fertility. While unilateral
tumors have traditionally been managed with radical orchiectomy, a
similar approach to bilateral synchronous seminomas warrant more
dedicated conversations with patients about their fertility plans and
quality of life. Bilateral radical orchiectomy remains the standard of
care with excellent oncologic control for these patients. However, it
results in sterility and often low quality of life due to hypogonadism
requiring life-long hormonal replacement therapy.
Our literature review revealed mounting evidence of successful
management of bilateral testicular GCTs with testis-sparing surgery
with good oncologic control and preservation of testosterone levels.
Tomita et al. demonstrated three cases successfully managed with
unilateral orchiectomy for the larger tumor, followed by three courses
of chemotherapy with cisplatin, etoposide and bleomycin [10]. After
demonstrating a 98.6% non-recurrence rate at 7 year follow-up in 52
metachronous and 17 synchronous bilateral testicular germ cell tumor
cases, Heidenreich et al. [11] suggested that organ-sparing surgery
may be viable for cases with cold ischemia, organ confinement, size
less than 20 mm, multiple biopsies of the tumor bed, adjuvant local
irradiation postoperatively to avoid local recurrence, close followup
and high compliance. Another case of a patient with bilateral
synchronous testicular cancer and azoospermia demonstrated the
successful delivery of a healthy baby after Intracytoplasmic Sperm
Injection (ICSI) of sperm cryopreserved during bilateral orchiectomy
[12], highlighting the importance of planning for TESE before
orchiectomy procedures. Whenever feasible, sperm cryopreservation
should be offered to all patients with testicular tumors prior to
intervention given the importance of fertility preservation in
the management of these patients. A clear indication for partial
orchiectomy for management of testicular tumors is synchronous
or metachronous disease. With data supporting good oncologic and
hormonal preservation outcomes associated with partial orchiectomy,
we propose that, a new goal of a trifecta for management of bilateral
testicular tumors: oncologic control with hormonal and fertility
preservation. However, current literature is limited by the primary
outcomes not including all three components. Future studies with the
aim of achieving the proposedtrifecta are therefore needed to further
confirm potential shift in the standard of care for carefully selected
young males with bilateral testicular tumors.
References
- Hayes-Lattin B, Nichols CR. Testicular Cancer: a prototypic tumor of young adults. Semin Oncol. 2009; 36: 432-438.
- Boujelbene N, Cosinschi A, Boujelbene N, Khanfir K, Bhagwati S, Herrmann E, et al. Pure seminoma: a review and update. Radiat Oncol. 2011; 6: 90-102.
- Sarıcı H, Telli O, Eroğlu M. Bilateral testicular germ cell tumors. Turkish J Urol. 2013; 39: 249-252.
- Akdogan B, Divrik RT, Tombul T,Yazici S, Tasar C, Zorlu F, et al. Bilateral testicular germ cell tumors in Turkey: increase in incidence in last decade and evaluation of risk factors in 30 patients. J Urol. 2007; 178: 129-133.
- Che M, Tamboli P, Ro JY, Park DS, Ro JS, Amato RJ, et al. Bilateral testiculargerm cell tumors: twenty-year experience at M.D. Anderson Cancer Center. Cancer. 2002; 95: 1228-1233.
- Oliveira Soares R, Pinto Correia T, Cardoso A, Oliveira e Silva A, Cerqueira M, Carmo Reis F, et al. Synchronous bilateral seminoma. Arch Esp Urol. 2011; 64: 69-73.
- Huddart RA, Norman A, Moynihan C, Horwich A, Parker C, Nicholls E, et al. Fertility, gonadal and sexual dysfunction in survivors of testicular cancer. Br J Cancer. 2005; 93: 200-207.
- Boer H, Proost JH, Nuver J, Bunskoek S, Gietema JQ, Geubels BM, et al. Long term exposure to circulating platinum is associated with late effects of treatment in testicular cancer survivors. Ann Oncol. 2015; 26: 2305-2310.
- Hjelle LV, Gundersen PO, Ondenburg J, Brydoy M, Tandstad T, Wilsgaard T, et al. Long-term Platinum Retention After Platinum-based Chemotherapy in Testicular Cancer Survivors: A 20-Year Follow-up Study. Anticancer Res. 2015; 35: 1619-1625.
- Tomita E, Kondo T, Nakazawa H, Ito F, Hashimoto Y, Tanabe K. Successful testis preservation for bilateral testicular tumors with a new chemotherapy-based protocol: initial results of three cases. Int J Urol. 2007; 14: 879-882.
- Heidenreich A, Weissbach L, Holtl W, Albers P, Kliesch S, Kohrmann KU, et al. Organ sparing surgery for malignant germ cell tumor of the testis. J Urol. 2001; 166: 2161-2165.
- Roque M, Sampaio M, Salles PG, Geber S. Onco-testicular sperm extraction: birth of a healthy baby after fertility preservation in synchronous bilateral testicular cancer and azoospermia. Andrologia. 2015; 47: 482-485.