Research Article
Radio Guided Parathyroidectomy in Oncologic Patients Using Portable Gamma-Camera: A Single Centre Experience
García-Pérez Francisco O1, Medina-Ornelas Sevastián S1* and Gómez-Pedraza Antonio2
1Department of Nuclear Medicine and Molecular Imaging, Mexico
2Department of Head and Neck Surgery, Mexico
*Corresponding author: Medina-Ornelas Sevastián S, Department of Nuclear Medicine and Molecular Imaging, National Institute of Cancerology, Mexico
Published: 05 Jan, 2017
Cite this article as: García-Pérez Francisco O, Medina-
Ornelas Sevastián S, Gómez-
Pedraza Antonio. Radio guided
Parathyroidectomy in Oncologic
Patients using Portable Gamma-
Camera: a Single Centre Experience.
Clin Oncol. 2017; 2: 1181.
Abstract
Objective: The objective of this study was to evaluate the utility of portable gamma-camera at real
time intraoperative imaging for assessing localization of parathyroid adenoma.
Materials and Methods: This was a retrospective analysis of patients with parathyroid adenoma
and oncologic underlying condition, such as breast cancer, renal, prostate, cervix, ovarian, and
melanoma; who underwent radio guided surgery at Instituto Nacional de Cancérologie (INCan,
México). Planar scintigraphy was performed 15 minutes after intravenous injection of 99mTc-MIBI,
60-120 min before intervention. The portable gamma-camera was used to identify the adenoma
during surgery, as well as to verify if it was removed completely. All surgical specimens were taken
for intraoperative histopathological evaluation.
Results: 20 patients were diagnosed with parathyroid adenoma (17 with usual location and 3 with
ectopic location). Parathyroid adenoma was localized Intraoperatively with a portable gammacamera
in all patients, reducing the time of surgery. All surgical specimens were confirmed as
parathyroid adenoma in the intraoperative and definitive histopathological evaluation.
Conclusion: Parathyroid scintigraphy with portable gamma-camera in intraoperative
identification of parathyroid adenoma has contributed to the development of minimally invasive
parathyroidectomy. Therefore, in our opinion, in addition to the realization of preoperative
scintigraphy, radio guided surgery with portable gamma-camera should always be performed,
thus reducing complications, hospital stay, surgical and recovery time, with the same therapeutic
effectiveness as classical treatment.
Keywords: Parathyroid adenoma; Portable gamma-camera; 99mTc-MIBI scintigraphy; Radioguided surgery; Minimally invasive parathyroidectomy
Background
Primary hyperparathyroidism (PHPT) is a metabolic disorder It characterized by hyper
secretion of parathormone parathyroid as a consequence of alterations in physiology at least one
parathyroid gland; such alteration may be due to glandular hyperplasia, parathyroid adenoma, rarely
parathyroid carcinoma or associated symptoms of multiple endocrine neoplastic syndromes I and II
[1,2]. Parathyroid cells exhibit both increased proliferative activity (leading to enlarged glands) and
decreased sensitivity to the inhibiting effect of increased calcium concentration on PTH secretion
(altered set point). Parathyroid adenoma has a prevalence of 1%, with maximum incidence is in the
3rd and 5th decade of life and being more common in women (3:1). Parathyroid adenomas have an
ectopic location in 5-10% of cases and the most common location is anterior mediastinum [2,3]. The conventional surgical approach is bilateral neck exploration; nevertheless the use of 99mTc-MIBI
scintigraphy Intraoperatively has made minimally invasive parathyroidectomy possible [4-6].
Parathyroid adenoma assessment with 99mTc-MIBI is based on longer retention of the tracer
in parathyroid compared with thyroid tissue, following injection, 99mTc-MIBI is distributed by the
bloodstream and is kidnapped intracellularly by mitochondria; the large number of mitochondria
cells present in most adenomas parathyroid makes a lot of radiopharmaceutical is grasped and
reflects the increase in metabolic activity adenomas compared to the surrounding thyroid tissue and
normal parathyroid glands [7-9].
The dual-phase parathyroid scintigraphy with 99mTc-MIBI
has sensitivity and specificity of 91% and 98.8%, respectively, and
is considered the best noninvasive study parathyroid for detection
[10,11]. A portable gamma camera has recently been introduced for
intra-operative visualization of radiotracer activity and can help to
localize the tumor during operation. The intra-operative use of this
portable device might lead to excision of additional parathyroid
tissue affected. In theory, this camera can also be used to improve
pre-operative adenoma or hyperplasia parathyroid visualization.
Provided that image quality and field of view are sufficient, a
portable gamma camera could be used when a conventional gamma
camera is unavailable, occupied or increase the specificity of the lesion
based on the amount of activity in the affected tissue [12]. There are
few reports in literature about the use of portable gamma-camera
(pGMC) in PHPT treatment [12-14].
Parathyroid surgery allows the surgeon to identify radio guided
specifically abnormal or hyper functioning parathyroid gland, without
the need for a scan extensive bilateral cervical looking for abnormal
tissue macroscopically it might seem parathyroid and corroborate
histologically also can facilitate the realization the procedure with
local anesthesia and on an outpatient basis [13-15].
The objective of this study was to evaluate the utility of portable
gamma-camera at real time intraoperative imaging for assessing
localization of parathyroid adenoma in patients with oncologic
disease.
Figure 1
Figure 1
Static planar double-phase parathyroid scintigraphy with 99mTc-
MIBI. (Left) Image at 15 min shows physiologic early uptake in thyroid gland,
with clear focus of intense increased accumulation at lower pole of right
thyroid lobe. (Right) Late scan shows almost complete washout of 99mTc-
MIBI from thyroid gland, with obvious focal retention of radioactivity at lower
pole of right thyroid lobe. Minimally invasive radio guided surgery confirmed
presence of parathyroid adenoma.
Figure 2
Figure 2
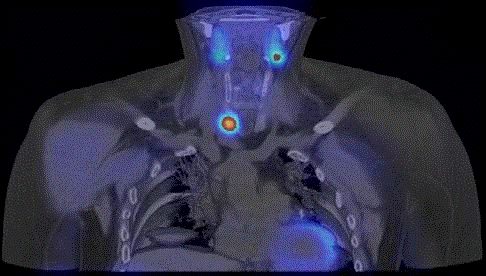
Image fusion of corresponding coronal slices of SPECT/CT
demonstrates that lesion with focal increased uptake of 99mTc-MIBI is
located in lower pole of right thyroid lobe.
Figure 3
Figure 3
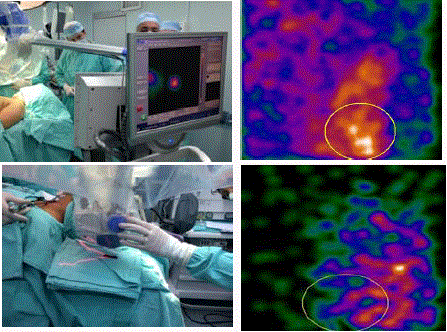
Surgical team making the radio guided parathyroidectomy. (Top
left) Medical staff positioning the portable gamma-camera on the patient's
neck 2 h after the intravenous injection of 99mTc-MIBI [approximately 740
MBq].(Top right) Intraoperative images obtained with portable gammacamera
[Sentinella, Oncovision®]of parathyroid adenoma localized in vivo
verified by the greater number of accounts within a ROI. (Bottom left) Images
post-surgical resection of the adenoma´s neck of the patient. (Bottom right)
Images obtained with portable gamma-camera of ex vivo of parathyroid
adenoma and verified by the number of accounts within the same ROI
previously outlined.
Materials and Methods
This was a retrospective analysis of patients with parathyroid
adenoma who underwent radio guided surgery at INCan.
They included patients with biochemical and scintigraphy
parameters of primary hyperparathyroidism.
Planar scintigraphy with the conventional gamma camera
(Symbia, Siemens®) of the neck and thorax was performed 15 min
and then 2-3 h after the intravenous injection of 99mTc-MIBI
(approximately 740 MBq [20 mCi]) before intervention in all patients.
The scan was considered positive for parathyroid disease when an
area of increased uptake that persists on late imaging is found 60-
120 min (Figure 1). Although only a marginal improvement in the
overall detection rate of parathyroid adenomas is reported with
SPECT(128 x 128 matrix, 60 x 25-s frames) was combined with CT
(130Kv, 17 mA, B60s kernel), using hybrid camera, in this protocol
each patient was carried out (Figure 2).
The portable gamma-camera (Sentinella, Oncovision®) was
used to identify the adenoma during surgery with the same activity,
after proper localisation, a minimally invasive parathyroidectomy
with minicervicotomy was started. This portable gamma camera
was equipped with a 4 mm pinhole collimator and uses a CsI (Na)
continuous scintillating crystal. The pinhole collimator was used to be
able to visualize the whole surgical field. The was placed at a distance
of 10 cm over the neck of the patient. Intrinsic spatial resolution is
1.8 mm, while extrinsic spatial resolution values are 7 mm and 21 mm
for a distance of 3cm and 15cm respectively.
After removing the adenoma, the activity it was verified in vivo
and ex vivo. It was taken as one whose site radioactivity counting was
20% higher than background radioactivity count, measured outside
the central compartment neck (Figure 3).
All surgical specimens were taken for intraoperative
histopathological evaluation.
Table 1
Results
Twenty patients were diagnosed with parathyroid adenoma (18
with usual location and 2 with ectopic location (Table 1), recruited
from February 2009 to June 2015. Of 20 accrued patients, 14 (70%)
were females and 6 (30%) were males. The average age was 39 years
(IC 95%), with a range from 18 to 69 years.
In all cases the 99mTc-MIBI scintigraphy showed increased
the concentration of the radiopharmaceutical in at least one gland
parathyroid. The preoperative scintigraphy with 99mTc-MIBI
showed sensitivity, specificity, diagnostic accuracy, PPV, and NPV
results of 100%.
Parathyroid adenoma was localized intraoperatively with
a portable gamma-camera in all patients, reducing the time of
surgery. The type of radio guided surgery was: minimally invasive
parathyroidectomy in 18 patients, and sternotomy in 2 patients
(1 anterior mediastinal and 1 posterior cervico-mediastinal). All
surgical specimens were confirmed as parathyroid adenoma in the
intraoperative and definitive histopathological evaluation (Figure 4).
The time from start of surgery to adenoma excision ranged from 15 to
45 min, mean 27 min (IC 95%). In all cases the radioactivity measured
Intraoperatively with the gamma camera, identified the affected gland, which coincided with the scintigraphic findings previous. The
pMGC showed sensitivity, specificity, diagnostic accuracy, PPV, and
NPV values of 100%.
No patient was identified disease multiglandular. All patients had
normal levels of calcium postoperative serum with mean 9.5 mg /
dl (IC 95%:7.65 -10.33 mg/dl), and PTH values with mean 47 pg/ml
(IC95%: 10-55). At the clinical and laboratory followup after 1, 3, 6,
and 12 months, no persistent or recurrent PHP was detected.
Discussion
Parathyroid scintigraphy with portable gamma-camera in
intraoperative identification of parathyroid adenoma has contributed
to the development of minimally invasive parathyroidectomy.
The guidelines for Parathyroid scintigraphy can be summarized as
follows: Only patients with a high probability of a solitary parathyroid
adenoma and a normal thyroid gland should be considered, the most
appropriate preoperative scintigraphicprotocol should be selected
on the basis of thyroid and parathyroid imaging information,
the radiation exposure dose to the surgeon and operating theater
personnel should be minimized by administering the lowest
dose of 99mTc-MIBI proven to be effective for performing of
Parathyroid scintigraphy, both in vivo or ex vivo γ-probe counting and intraoperative PTH measurement should be used to evaluate the
success and completeness of surgery [16-19]. Our series confirms
the value of scintigraphy in the detection and localization of ectopic
adenomas. Scintigraphy detected all the parathyroid adenomas in
both planar and tomographic images. The use of gamma probes allows
the detection of sources of radiotracers administered at the time
of induction of anesthesia and well counter during the procedure.
Gamma probes, however, translate focus intensity into count rate
and audio signaling and as such do not guarantee the more precise
localization given by imaging, and do not exclude de possibility of the
more adenomas [21].
Although of pMGC in PHP treatment has been used for years
in the treatment of ectopic parathyroid adenoma, no large series
of patients treated with this procedure have been published in the
literature.
Hypercalcemia occurring in patients with advanced breast cancer
is generally due to osteolytic metastases or to the activity of circulating
tumor-derived products. In these conditions, the production of
endogenous PTH is reduced. The frequency of hypercalcemia due to
primary hyperparathyroidism in breast cancer is unknown [20].
It is known that high levels of PTH are associated with increased
bone resorption and degradation of the bone matrix. There are isolated
reports of low serum calcium and high PTH levels in a number of
studies involving small numbers of patients with advanced prostate
cancer. The extent of these abnormalities and their pathophysiological
significance is not well defined [22].
Estrems and cols. [13] evaluated the feasibility of this method
in a group of 29 patients: side localization with pMGC showed a
sensitivity of 86.6% and a specificity of 90.9% compared to the 79.3%
and 92.5%, respectively, of preoperative investigations (ultrasound
+ scintigraphy) while quadrant localization showed a sensitivity of
83.3% and a specificity of 90.9%, when compared to 48.35% and
72.7%, respectively, reported in the preoperative surveys.
Casella and cols. (Casella et al. [12]) evaluated the effectively of
the pMGC in a group of 20 patients properly localized all lesions
by side (diagnostic accuracy 100%) with both a sensitivity and a
specificity of 100%, while as far as quadrant was considered pMGC
showed a diagnostic accuracy of 98.1%, a sensitivity of 95.0%, and a
specificity of 98.8%.
This differentiates our protocol from other protocols described
by diverse authors. Casella et al. [12] perform intraoperative image
acquisition protocol, we intravenously infused 185 MBq of 99mTcsestaMIBI
immediately after the induction of general anesthesia.
Casara et al. [19] and Rubello et al. [15] perform minimally invasive
parathyroidectomy according to a two day protocol, also with an
established dose of radionuclide (37 MBq) that is injected just before
starting surgery. The absence of radiotracer uptake sources in the post
excision images confirms the completeness of the parathyroidectomy,
completeness that is usually confirmed by the significant fall in PTH,
also.
Detect this condition can be very complicated, especially in
patients with poor response to treatment, and that the first duty of
the physician is to rule out the possibility of progression; however
when symptomatology, especially gastrointestinal and mental,
not improve despite good management, it is necessary to consider
hyperparathyroidism, even when calcium levels are within normal
values, especially in prostate cancer.
Despite the limited number of patients studied, our study has
confirmed the possibility of replacing the intra operative PTH
measurement with the intraoperative use of the pMGC, because in
all cases the images obtained after removal of the parathyroid lesions
were comparable to the fall in post operative PTH levels. The pMGC
may also be a possible alternative to preoperative scintigraphy with
99mTc-sestaMIBI.
Conclusion
In our opinion, in addition to the realization of preoperative scintigraphy, radio guided surgery with portable gammacamera should always be performed, an smaller incision reduced complications, less surgical trauma, shorter length procedure is a very attractive surgical approach to treat patients with PHPT secondary to solitary parathyroid adenoma. has proven to be technically easy, safe, and with a low morbidity rate in the hands of a skilled surgeon. We suggest that serum PTH should be determined in all breast cancer patients with increased serum calcium concentration, especially in those with no evidence of metastatic disease; also in patients with other oncologic conditions with symptomatology that does not subside despite the good management, without ruling out possibility of disease progression.
References
- Bilezikian JP, Silverberg SJ. Clinical spectrum of primary hyperparathyroidism. Reviews in Endocrine and Metabolic Disorders. 2000; 237-245.
- Mariani G, Gulec SA, Rubello D, Boni G, Puccini M, Pelizzo MR, et al. Preoperative localization and Radioguided Parathyroid Surgery. J Nucl Med. 2003; 1443-1458.
- MacKenzie-Feder J, Sirrs S, Anderson D, Sharif J, Khan A. A Primary Hyperparathyroidism: An Overview. Int J Endocrinol. 2011; 11-18.
- Díaz-Expósito R, Casáns-Tormo I, Cassinello-Fernández N, Ortega-Serrano J, Mut-Dólera T. Aportación de la gammagrafía intraoperatoria en la detección del adenoma paratiroideo intratiroideo. Rev Esp Med Nucl Imagen Mol. 2014; 296-298.
- Rubello D, Pelizzo MR, Casara D. Nuclear medicine and minimally invasive surgery of parathyroid adenomas. Eur J Nucl Med Mol Imaging. 2003; 189-192.
- Prats E, Razola P, Tardin L, Andrés A, García López F, Abós, et al. Gammagrafía de paratiroides y cirugía radiodirigida en el hiperparatiroidismo primario. Rev Esp Med Nucl Imagen Mol. 2007; 310-330.
- Goldstein R, Billheimer D, Martin W, Richards K. Sestamibi scanning and minimally invasive radioguided parathyroidectomy without intraoperative parathyroid hormone measurement. Ann Surg. 2003; 722-731.
- Mitchell BK, Cornelius EA, Zoghbi S, Murren JR, Ghoussoub R, Flynn SD, et al. Mechanism of technetium 99m sestamibi parathyroid imaging and possible role of p-glycoprotein. Surgery. 1996; 120: 1039–1045.
- Froeberg AC, Valkema R, Bonjer HJ, Krenning EP. 99mTc-tetrofosmin or 99mTc-sestamibi for double-phase parathyroid scintigraphy? Eur J Nucl Med Mol Imaging. 2003; 193–196.
- Demirkurek GH, Adalet I, Terzioglu T, Ozarmagan S, Bozbora A, Ozbey N, et al. Efficiency of gammaprobe and dual-phase Tc-99m Sestamibi scintigraphy in surgery for patients with primary hyperparathyroidism. Clin Nucl Med. 2003; 186-191.
- Denham D, Norman J. Cost-effectiveness of preoperative sestamibi scan for primary hyperparathyroidism is dependent solely upon the surgeon’s choice of operative procedure. J Am Coll Surg. 1998; 293-305.
- Casella C, Rossini P, Cappelli C, Nessi C, Nasciembeni R, Portolani N. Radioguided Parathyroidectomy with Portable Mini Gamma-Camera for the Treatment of Primary Hyperparathyroidism. Int J Endocrinol. 2015; 1-6.
- Estrems P, Guallart F, Abreu P, Sopena P, Dalmau J, Sopena R. The intraoperative mini gamma camera in primary hyperparathyroidism surgery. Acta Otorrinolaringol Esp. 2012; 450–457.
- Ortega J, Ferrer-Rebolleda J, Cassinello N, Lledo S. Potential role of a new hand-held miniature gamma camera in performing minimally invasive parathyroidectomy. Eur J Nucl Med Mol Imaging. 2007; 165-169.
- Rubello D, Massaro A, Cittadin S, Rampin L, Al-Nahhas A, Boni G, et al. Role of 99mTc-sestamibi SPECT in accurate selection of primary hyperparathyroidpatients for minimally invasive radio-guided surgery. Eur J Nucl Med Mol Imaging. 2006; 1091–1094.
- Kavanagh DO, Fitzpatrick P, Myers E, Kennelly R, Skehan SJ, Gibney RG, et al. A Predictive Model of Suitability for Minimally Invasive Parathyroid Surgery in the Treatment of Primary Hyperparathyroidism. World J Surg. 2012; 36: 1175-1180.
- Rubello D, Casara D, Saladini G, Piotto A, Pagetta C, Pelizzo MR. 99m Tc-MIBI Radio-Guided Surgery in Primary Hyperparathyroidism: a Prospective Study of 128 Patients. Tumori. 2002; 88: S63–S65.
- Flynn MB, Bumpous JM, Schill K, McMasters KM. Minimally invasive radioguided parathyroidectomy. J Am Coll Surg. 2000; 24-31.
- Casara D, Rubello D, Piotto A, Pelizzo MR. 99mTc-MIBi Radio-Guided Minimally Invasive Parathyroid Surgery Planned on the Basis of a Preoperative Combined 99m Tc-Pertechnectate/99m MIBI and Ultrasound Imaging Protocol. Eur J Nucl Med. 2000; 27: 1300–1304.
- Fierabracci P, Pinchera A, Miccoli P, Conte PF, Vignali E, Zacagnini M, et al. Increased Prevalence of Primary Hyperparathyroidism in Treated Breast Cáncer. J Endocrinol Invest. 2001; 24: 315-320.
- Tsuchimochi M, Hayama K. Intraoperative Gamma Cameras for Radioguided Surgery: Technical Characteristics, Performance Parameters, and Clinical Applications. Phys Med. 2013; 29: 126–138.
- Murray RM, Grill V, Crinis N, Ho PW, Davison J, Pitt P. Hypocalcemic and Normocalcemic Hyperparathyroidism in Patients with Advanced Prostatic Cancer. J Clin Endocrinol Metab. 2001; 86: 4133-4138.