Case Report
Two Patients with Advance-Stage Renal Cell Carcinoma Developed Sunitinib-Related Skin Toxicity
Mehmet Cetinkaya1*, Ozgur Tanriverdi2, Hasan Deliktas1, Asude Kara3, Yelda Dere4 and Hayrettin Sahin1
1Department of Urology, Mugla Sitki Kocman University, Turkey
2Department of Medical Oncology, Mugla Sitki Kocman University, Turkey
3Department of Dermatology, Mugla Sitki Kocman University, Turkey
4Department of Pathology, Mugla Sitki Kocman University, Turkey
*Corresponding author: Mehmet Cetinkaya, Department of Urology, Mugla Sitki Kocman University, Turkey
Published: 31 Dec, 2016
Cite this article as: Cetinkaya M, Tanriverdi O, Deliktas
H, Kara A, Dere Y, Sahin H. Two
Patients with Advance-Stage Renal
Cell Carcinoma Developed Sunitinib-
Related Skin Toxicity. Clin Oncol. 2016;
1: 1177.
Abstract
With the current treatment modalities like molecular targeted therapy, general survival rates have
increased in patients with advanced-stage renal cell carcinoma. Sunitinib male at is one of these
drugs and its most frequently side effects are fatigue, diarrhea, hypertension, stomatitis, and hair
hypo-pigmentation. Additionally, various dermatological side-effects may also be seen such as
hand-foot syndrome, a yellowish color change to the face, splinter hemorrhage, erythematosus
reactions on the trunk, facial edema, facial erythematosus changes, alopecia, acneiform rash on the
face and dysesthesia in the scalp. Although sunitinib maleat-related scrotal skin toxicity is extremely
rarely seen, it should not be forgotten that this side-effect can be easily managed. Herein, we report
two cases with sunitinib maleat-related scrotal skin toxicity, which were diagnosed with advancedstage
renal cell carcinoma in this case report.
Keywords: Sunitinib; Kidney cancer; Scrotal cutaneous toxicity; Molecular targeted therapy
Introduction
With molecular targeted treatment, overall survival rates have been recently increased in patients
with advanced-stage Renal Cell Carcinoma (RCC) [1]. Sunitinib maleat, an orally tyrosine kinase
inhibitor, is one of these targeted molecules which have small molecular weight [1]. It is widely used
in the treatment of patients with advanced-stage RCC, metastatic neuroendocrine carcinoma, and
gastrointestinal stromal tumors [1,2].
Most frequently side-effects in patients using sunitinib maleat are fatigue, diarrhea, hypertension,
stomatitis, and hair hypo-pigmentation [1-3]. Additionally, various dermatological sideeffects
may also be seen such as hand-foot syndrome, a yellowish color change to the face, splinter
hemorrhage, erythematosus reactions on the trunk, facial edema, facial erythematosus changes,
alopecia, acneiform rash on the face and dysesthesia in the scalp [1-3]. However, sunitinib maleatrelated
scrotal skin toxicity is rarely seen [3,4].
Herein, we report two cases with sunitinib maleat-related scrotal skin toxicity, which were
diagnosed with advanced-stage renal cell carcinoma in this paper.
Case Presentation
Case 1
A 72-year old male, who have not previous disease other than controlled hypertension, presented
with complaints of increasingly worsening shortness of breath and cough. A solid mass in the left
kidney with showing heterogeneous contrast, its size was approximately 7 x 8 cm, was determined
in Computerized Tomography (CT) as well as multiple lymph nodes in mediastinum and bilateral
multiple nodules in pulmonary parenchyma. Moreover, he has widespread bone metastases in
thoracic as well as lumbar vertebrae. Then biopsy was performed from the mass in the left kidney
and it was diagnosed as a clear cell renal carcinoma.
After consultation with the Medical Oncology Department, the patient was started on treatment
of interferon 2α. In the evaluation made after 3 months of treatment, progression of the disease was
determined. Treatment was then started of 50 mg sunitinib maleat for 4 weeks every 6 weeks. On the 24th day of treatment, the patient presented with a skin reaction on
the scrotum, which was clearly defined with scattered desquamation
areas in the form of erythematosus atrophic plaque (Figure A). A
biopsy was taken from the lesion. The sunitinib maleat treatment
was halted and within 10 days the lesion completely recovered and
the biopsy result was evaluated as drug reaction. The patient was restarted
on the same treatment scheme and on the 16th day similar
scrotal lesions developed and again when the sunitinib treatment was
halted, the findings recovered. The patient was started on a treatment
program of continuous sunitinib maleat at 25mg/day and apart from
mild scrotal erythematosus plaques which lasted approximately 1
week, no other skin reaction was observed. After approximately 7
treatment cycles, progression developed in pulmonary metastasis and
with a worsening of general status the patient was lost 11 months after
the diagnosis.
Case 2
A 77-year old male, who was previously healthy, presented with
complaints of back and side pain which had been increasing for
approximately 2 months. On the examination with CT, a lobular
contoured solid mass in the right kidney with showing heterogeneous
contrast, its size was 77 x 59 mm and bilateral multiple nodules in
pulmonary parenchyma were determined as well as widespread
bone metastases in scintigraphic examination. With rightside
nephrectomy, a diagnosis was made of Grade T1 clear cell
carcinoma limited to within the renal capsule, 6.5cm in size, of nuclear
degree Fuhrman IV which had general necrosis and mitosis. Then
interferon 2α treatment was initiated by the Oncology department.
In the second month of treatment, intolerance and progression of
pulmonary metastasis were observed and therefore the treatment
was continued with 50mg/day sunitinib maleat for 4 weeks every 6
weeks. However, similar scrotal lesions, which were clearly defined
with scattered desquamation areas in the form of erythematosus
atrophic plaque, developed on the 14th day of treatment (Figure B).
The sunitinib maleat treatment was halted and within 10 days the
lesion completely recovered and the biopsy result was evaluated as
drug reaction. Treatment of 25mg/day continuous sunitinib maleat
was started and no skin reaction was observed. The patient then
transferred to another centre for follow-up and as the patient could
not be contacted; there is no further information available on the
clinical course.
On dermatological examination, widespread erythematosus
atrophic plaques with scattered desquamation were observed on the
scrotum (Figure A and B).
Histopathological examination showed interface dermatitis
characterized by vacuolar degeneration in the basal layer and
dyskeratotic cells with perivascular mononuclear inflammatory cells
in the dermis and these findings were reported as consistent with
drug induced dermatitis (Figure C and D).
Figures
Figures
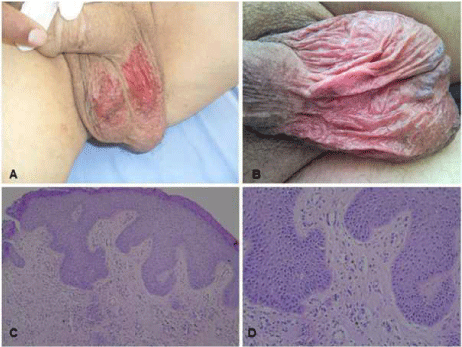
Macroscopic images and microscopic examination of sunitinib-related skin toxicity, A-B: Macroscopic image of Case 1 and Case 2, respectively showing live erythematous atrophic plaque with scattered desquamated areas clearly limited to the scrotum. C-D: Scrotum skin biopsy microscopic examination (HEx100, HEx200): interface dermatitis findings characterized by vacuolar degeneration in the basal layer and dyskeratotic cells with perivascular mononuclear inflammatory
cells to the dermis, consistent with drug induced dermatitis.
Discussion
Although various dermatological side-effects have been seen
in patients using sunitinib maleat, prevalence of its skin toxicity
has been reported as nearly < 15% in previous studies. Moreover,
sunitinib maleat-related scrotal skin toxicity is extremely rare [1-
4]. Sunitinib maleat-related scrotal skin toxicity was first described
by Billemont et al. [3]. In a total of 40 RCC patients treated with
sunitinib maleat, it was reported in only 5 (12%) patients that scrotal
erythematosus lesion developed accompanying desquamation.
Subsequently, a case of sunitinib-related recurrent scrotal
hemangiomas was reported by Tonini et al. [5].
Although the mechanism of scrotal cutaneous toxicity
has not been clarified, Billemont et al. [3] hypothesized that
the underlying mechanism of this toxicity could be the antiangiogenic
effect of sunitinib maleat. It is also thought that hypoxiainducible
factor -1α (HIF-1α) and Vascular Endothelial Growth
Factor (VEGF) play an important role in sunitinib-related cutaneous
toxicity. This view has been supported in studies showing an in vitro
increase in plasma VEGF levels after treatment with sunitinib maleat
in patients with RCC [3]. Moreover, in patients with psoriasis, it has
been shown that HIF-1α was strongly unregulated and at the same
time angiogenesis was induced by VEGF [6]. As a result, increased
limited oxygen diffusion within the tissues in both normal and
tumor, which could be explained by paradoxical hypoxia, could cause an anti-angiogenic process.
In the most recent article on sunitinib maleat-related scrotal skin
toxicity by Chou et al. [7] sunitinib maleat-related scrotal cutaneous
toxicity was confirmed by biopsy as well as indicated that strongly
stained with VEGF by immunohistochemically examination was
determined in the endothelial cells of the dermal blood vessels in
a 74-year old male patient with RCC. This was the first paper to show
the relationship between VEGF and sunitinib maleat-related scrotal
cutaneous side-effect. Chou et al. [7] showed that there was no
staining with VEGF in normal scrotal tissue taken from a healthy
male and thus concluded that VEGF played a significant role in
sunitinib maleat-related scrotal skin toxicity.
Although cases presented in literature differ from each other
in respect of sunitinib dose and application schedule, the scrotal
cutaneous side-effect was observed to develop at 7-14 days after
starting the medication [3,4,6]. This can suggest that there is no
significant relationship between medication dosage and scrotal
cutaneous toxicity. In our cases, the side-effects were observed after
exposure to the drug, which is consistent with the data in literature.
Similarly it has been reported that within a week of stopping the
sunitinib treatment, cutaneous findings recovered. In the current
cases, it was also seen that the cutaneous findings recovered one week
after halting the sunitinib treatment.
The conclusion can be reached that the sunitinib-maleat related
cutaneous side-effect recovers after stopping the medication and
this side-effect can be easily managed with dose modification.
Therefore, that scrotal cutaneous toxicity could develop but
this is a manageable side-effect must be explained to patients
receiving sunitinib-maleat treatment.
In conclusion, although rare in the follow-up of patients receiving
sunitinib maleat treatment, scrotal cutaneous toxicity should not be
forgotten as one of the dermatological side-effects which may be seen.
When it is taken into account that a significant increase in survival
rates is achieved, this side-effect can be considered not to play a
significant role in discarding the medication.
References
- Ara M, Pastushenko E. Antiangiogenic agents and the skin: cutaneous adverse effects of sorafenib, sunitinib, and bevacizumab. Actas dermosifiliograficas. 2014; 105: 900-912.
- Rosenbaum SE, Wu S, Newman MA, West DP, Kuzel T, Lacouture ME. Dermatological reactions to the multitargeted tyrosine kinase inhibitor sunitinib. Supportive care in cancer: Support Care Cancer. 2008; 16: 557- 566.
- Billemont B, Barete S, Rixe O. Scrotal cutaneous side effects of sunitinib. N Engl J Med. 2008; 359: 975-976.
- Iacovelli R, Mancini ML, Risi E, Palazzo A, Cortesi E. Genital and inguinal cutaneous toxicity in male and female patients treated with sunitinib. International journal of dermatology. 2012; 51: 221-222.
- Tonini G, Intagliata S, Cagli B, Segreto F, Perrone G, Onetti Muda A, et al. Recurrent scrotal hemangiomas during treatment with sunitinib. Journal of clinical oncology: J Clin Oncol. 2010; 28: 737-738.
- Simonetti O, Lucarini G, Goteri G, Zizzi A, Biagini G, Lo Muzio L, et al. VEGF is likely a key factor in the link between inflammation and angiogenesis in psoriasis: results of an immunohistochemical study. Int J Immunopathol Pharmacol. 2006; 19: 751-760.
- Chou CY, Wang KH, Lin YH, Lin YT, Tsai HH. Sunitinib-induced scrotal cutaneous side-effect. The Journal of dermatology. 2013; 40: 67-68.