Research Article
Bladder Neck Preservation during Radical Prostatectomy Needed for Recovery of Continence in Elderly Men (>70 years)
Yu YD1, Kang MH1, Choi KH1, Oh JJ2 and Park DS1*
1Department of Urology, CHA Bundang Medical Center, CHA University, Seongnam, Korea
2Department of Urology, Seoul National University Bundang Hospital, Seongnam, Korea
*Corresponding author: Dong Soo Park, Department of Urology, CHA Bundang Hospital, CHA University College of Medicine 59 Yatap-ro, Bundang-gu Seongnam 463-712, Korea
Published: 30 May, 2016
Cite this article as: Yu YD, Kang MH, Choi KH, Oh JJ, Park
DS. Bladder Neck Preservation during
Radical Prostatectomy Needed for
Recovery of Continence in Elderly Men
(>70 years). Clin Oncol. 2016; 1: 1004.
Abstract
Purpose: To determine the influence of bladder neck preservation (BNP) on postoperative continence and positive bladder neck surgical margin rates.
Materials and Methods: Total 321 patients over 70 years with localized prostate cancer underwent
robot assisted laparoscopic prostatectomy (RALP), with 163 men undergoing standard bladder neck
dissection (group 1) and 168 undergoing BNP (group 2). Group 1 patients received standard RALP
techniques with Ven velthoven continuous suturing for urethrovesical anastomosis and group 2
patients received both standard RALP techniques and lateral bladder neck dissection. Pre- and postoperative
urinary function and continence recovery were evaluated and compared between the two
groups.
Results: The overall positive margin rate was 4.9% in group 1 and 12.5% in group 2, indicating a
greater positive surgical margin rate with statistical significance in the bladder neck preservation
group (p=0.045). Postoperative continence was evaluated by EPIC short form questionnaire
and at 1 and 4 months postoperatively, the mean urinary function scores were higher in group 2
compared to group 1 with statistical significance (p=0.021 at 1month, p=0.043 at 4 months). Group
2 showed significantly higher continence rates at 1 and 4 months post-RALP than group 1.(p<0.001
at 1month, p=0.003 at 4 months). In group 2, the recovery of continence approached to 91.3%
at 4 months post-operation showing early return of continence was observed in the patients with
bladder neck preservation. Conclusions: In healthy elderly patients, early recovery of postoperative
continence and urinary functions after RALP can be achieved by bladder neck preservation.
Keywords: Prostate; Urinary bladder; Prostatectomy; Urinary incontinence
Introduction
Because of increasing social awareness of PSA testing, the detection of prostate cancer has increased in South Korea [1], and radical prostatectomy still remains the major definitive treatment for localized prostate cancer. Robotic-assisted laparoscopic radical prostatectomy (RALP) has been rapidly applied in recent years due to its advantages of minimal invasiveness compared to open surgery [2]. Post-prostatectomy urinary incontinence ranges between 2.5% and 87% depending on the definition of urinary control [3], and it significantly deteriorates quality of life (QOL). Thus, the recovery of continence is one of the most important factors for the quality of life of patients undergoing RALP, while the recovery of continence is related to multi-factors including age of the patients, better baseline urinary function as well as longer membranous urethral length and among these factors, the surgical technique such as nerve sparing and bladder neck preservation (BNP) is considered most critical [4]. The recovery rate of continence is relatively satisfactory, with rates of 85% to 97% at 1 year post-prostatectomy, but complete recovery may require a much longer time in some patients [5]. To the best of our knowledge, a few studies have evaluated the impact of BNP on urinary continence, QOL changes and surgical margins (SM) status but no study has analyzed the outcomes of BNP in elderly patients over age 70. Thus, this study focused on analyzing the outcomes of BNP using anterior bladder neck approach with lateral bladder neck dissection (LBND) technique for recovery of continence in elderly patients underwent RALP. Moreover, this study also compared the post-prostatectomy cancer control outcomes of BNP with non-preserving techniques during RALP by evaluating the rate of positive surgical margins.
Materials and Methods
Patient enrollment
The patients of the study were recruited after receiving approval
from the CHA institutional review board and all of these patients
provided informed, formal written consent. From September 2013
to January 2016, total 321 patients over 70 years with biopsy proven
localized prostate cancer underwent RALP, with 163 men undergoing
standard bladder neck dissection (group 1) and 168 undergoing
BNP (group 2). The patients with a history of previous transurethral
resection of prostate or diagnosed incontinence were excluded from
the study. For group 1 patients, standard RALP techniques with Ven
velthoven continuous suturing for urethrovesical anastomosis was
performed, while group 2 patients received standard RALP techniques
of Ven velthoven continuous suturing for urethrovesical anastomosis
and LBND. RALP was performed by a single experienced surgeon.
Surgical technique
After making transperitoneal or extraperitoneal approach to
the retropubic space of Retzius, the bladder neck dissection was
performed as the first step of RALP. A ProGrasp™ grasper, Maryland
bipolar dissector, and curved monopolar scissors were equipped into
the third arm (left side of the patient), the first arm (left side of the
patient), and the second arm of patient's right side, respectively. The
position of spherical contour of the Foley catheter balloon was used
as a reference point to perform the bladder neck dissection. Sharp
dissection was carried out at the midline through the connective tissue
of the detrusor apron until bladder fibers show up. After confirming
linear fibers of the bladder neck, a combination of sharp and blunt
dissection was performed to separate bladder muscle fibers away
from the prostate, anatomically preserving a funneled bladder neck.
The use of monopolar current may obscure these bladder fibers due
to tissue charring, so that short bursts of bipolar current were applied
for hemostasis. After making incision along the curve of the prostate,
the dissection was extended laterally with focusing on prevention of
injuries of vessels projecting from the prostate lateral pedicle to the
dorsal vascular complex. Then sharp dissection was applied in a caudal
direction over the anterior bladder neck until the prostatic urethra
was exposed. More sharp dissection was done in lateral side to the
bladder neck with Maryland dissector and it resulted in confirmation
of the funneled shape bladder neck transitioning to the prostatic
urethra. During this lateral bladder neck dissection for the BNP, the
visual confirmation of the detrusor muscle fibers at the junction of
the lateral bladder neck, prostate base, and the fat pad of Whitmore
was the first and necessary step for the procedure. When the lateral
bladder neck dissection in bilateral sides was completed, the anterior
and lateral aspects of the seminal vesicle could be exposed. Then the
detrusor muscles in the posterior side of bladder neck, which was
located anterior to the seminal vesicles, could be dissected at the
midline until the bladder neck is divided. BNP was considered as
successful when the diameter of the bladder neck was approximate to
the diameter of the urethral stump so that reconstructive tapering of
bladder neck was not needed before the urethrovesical anastomosis.
During the Ven velthoven technique applied for the urethrovesical
anastomosis, a continuous suturing of the urethra from 3 to 9 o'clock
of the urethral lumen was done by using monofilament 3-0 double
arm sutures (Figure 1).
Outcomes and analysis
Preoperative urinary function and continence recovery were
evaluated by assessing the Expanded Prostate Cancer Index (EPIC)
short form in all 321 patients before RALP as well as at 1 and 4
months postoperative visits. Postoperative continence was defined
as using less than one diaper per day in EPIC query. Post-RALP
cystogram was obtained in all patients on the 9th postoperative day,
and the postoperative urine leakage was defined as anastomotic
contrast extravasation on cystography. For the patients with urine
leakage in cystography, urethral catheter was planned to be kept
for an additional 7 days. The pre- and postoperative variables were
compared between non-BNP group and BNP group by using Pearson
chi-square, Fisher's exact and multiple logistic regression analysis
with p-value ≤ 0.05 were considered as statistically significant. SPSS®
ver. 12.0 (SPSS Inc., Chicago, IL, USA) and SAS®
ver. 9.0 (SAS, Cary,
NC, USA) were used for the statistical analysis.
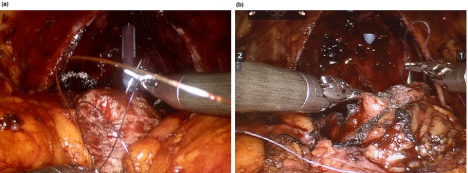
Figure 1
Figure 1
Urethrovesical anastomosis in (a) bladder neck preservation
patient; (b) Non-baldder neck preservation patient.
Results
Patient characteristics including baseline urinary function, body mass index, cormobidities, prostate-specific antigen (PSA), biopsy Gleason grade, clinical stage and prostate size were similar between non-BNP group (group 1) and BNP group (group 2) (Table 1). Group 1 had a larger mean preoperative urinary function compared to group 2 (90.3 vs. 92.9), but the difference was statistically insignificant (p=0.35). The means age of the patient was 72.5 and 71.7 for group 1 and group 2, respectively (p=0.23). The mean prostate volume and preoperative PSA level were 38.6 ml and 9.4 ng/ml for group 1, while group 2 showed 39.0 ml and 9.8 ng/ml that indicates no statistically significant differences were observed between two groups (prostate vol. p=0.72, PSA p=0.59). Moreover, the biopsy Gleason grade between two groups was similar (p=0.21) and Gleason grade 7 (3+4) was the most common grade in both patient groups. The preoperative clinical stage of the two groups showed no statistically significant difference between two groups (p=0.48) as group 1 had 135 patients in T2, 16 patients in T3a, and 12 patients in T3b while group 2 was consisted of 139, 17 and 13 patients in stage T2, T3a and T3b, respectively. The mean body mass index (BMI) also showed no statistically significant difference between two groups as BMI for group 1 and 2 were 24.6 and 23.9 kg/m2, respectively, (p=0.34). The mean operation times (OPT) and the mean estimated blood loss (EBL) of group 1 were 198.2 minutes and 140.3 ml while group 2 recorded 185.4 minutes and 120.5 ml. The differences in the mean OPT and EBL between two groups were statistically insignificant (OPT p=0.86, EBL p=0.51). Both group 1 and 2 had the same length of catheterization that was 8 days and urethral catheter was removed on the 9th day post-RALP. The cystogram taken on the 9th postoperative day revealed no cases of urine leakage in both groups (Table 1). With respect to postoperative outcomes, the overall positive margin rate was 4.9% (8 patients) in group 1 and 12.5% (21 patients) in group 2, which was indicating a greater positive surgical margin rate with statistical significance in the bladder neck preservation group (p=0.045). According to the location of positive surgical margins, 5 patients in the lateral, 1 patient in the base, and 2 patients in the apical region of the prostate were confirmed. In group B, 1, 9 and 2 patients were confirmed for positive surgical margin in the lateral, base, and apical region of the prostate (Table 2). Postoperative continence was evaluated by EPIC short form questionnaire and at 1 and 4 months postoperatively, the mean urinary function scores were higher in group 2 compared to group 1 with statistical significance (p=0.021 at 1month, p=0.043 at 4 months). Moreover, group 2 also showed significantly higher continence rates at 1 and 4 months post-RALP than group 1. (p<0.001 at 1month, p=0.003 at 4 months) (Table 3). In group 2, the recovery of continence approached to 91.3% and the urinary function was 74.5 at 4 months post-operation so that relatively early return of urinary function and continence was observed in the patients with bladder neck preservation.
Table 1
Table 2
Table 3
Discussion
Although the upper age limit of radical prostatectomy as a treatment for localized prostate cancer is still controversial, generally radical prostatectomy was rarely was applied to the elderly patients over 70 years due to relatively short life expectancy and poor functional outcomes. On the other hands, some studies including Siddiqui et al. reported that the oncological outcomes of radical prostatectomy in elderly patients are comparable to the one of younger age patients [6]. In Korea, elderly population over 65 years of age is rapidly expanding and it accounts for 13.1% of the national population [7]. In turn, RALP as a treatment for localized prostate cancer in elderly patients is also increasing and this study tried to research the oncological and functional outcomes after RALP in patients over 70 years. The early recovery of continence after radical prostatectomy by performing bladder neck preservation has been emphasized since the early 1990s [8,9] and even after the adaption of minimally invasive surgery including RALP, the application of bladder neck preservation has been increasing. In addition, due to advanced video-endoscopic equipments of robotic surgery, fine dissection requiring procedures such as the bladder neck preservation and nerve-sparing have become relatively easier to perform and some studies have reported that bladder neck sparing is associated with earlier recovery of continence within a year of RALP [10-12]. However, a few researches including Ahlering et al. reported that an absence of tactile feedback may account for bladder neck dissection being regarded as one of the most challenging steps of RALP [13]. In this study, the patients with BNP using LBND had excellent outcomes of early return of continence by showing the continence rate of 91.3% at 4 months post-operation. These results are consistent with other previous studies showing better early continence recovery achieved by BNP during open radical prostatectomy or RALP [14-16]. Since the diameter of the bladder neck was approximate to the diameter of the urethral stump with tension free sutures during BNP, it can be assumed that the anatomical and functional reconstruction of the urethral sphincter complex was achieved through BNP. Thus, a better early continence and urinary function were restored as a result. Moreover, we tried to make as little thermal and physical damages to the tissues adjacent to prostate as possible during LBND so that most sensory nerve fibers innervating to the proximal urethra are believed to be preserved. In the recent studies [17], Ven velthoven continuous suturing technique decreased the rate of early continence recovery after RALP, but it was partially overcome by gaining of more surgical experience and technique of the surgeon. This was consistent with our study as the outcomes of continence recovery, operation time and blood loss became better in both group 1 and 2 patients as the number of RALP cases accumulated. In addition, the preoperative urinary functions of the patient in this study were comparable with the studies focused on the relatively younger patients [18,19]. This might be due to significantly lower rates of comorbidities of the patients in this study compared to the general elderly populations that was not intended during the selection of the patients. Thus if the rates of comorbidities were higher, the outcomes of postoperative continence and urinary function might have been changed and the further research concerning cormobidities is currently under active evaluation as our next study. In this study, no patient had urinary leakage in post operative cystography and we assume relatively longer time of urethral catheterization and meticulous suturing technique during urethrovesical anastomosis were the main contributions. The whole patients of this study were maintained with 8 days of catheterization to minimize the effects catheterization time on postoperative outcomes as well as to prevent urinary leakage by supporting wound healing on urethrovesical anastomosis. In accordance with the results of postoperative urinary leakages of the study, maintaining catheterization time for 8 days or longer can be recommended in elderly patients after RALP. Many studies suggested that bladder neck has preservation compromises cancer control by increasing the positive margins at the prostate base [18-20]. We also observed similar outcomes since 12.5% patients of group 2 had positive surgical margins while only 4.9% patients were positive in group 1. Regarding the location of positive surgical margins, group 2 patients had the greatest portions of positive surgical margins at the base of prostate and it was almost 6 times greater rate with a statistical significance compared to group 1. However, since there have been some studies, including Razi et al. [21] reporting BNP had no negative impact on the positive surgical margin rates, a further study with a greater number of the patients and longer follow up period should be taken place to conclude definite impacts of BNP on surgical margins. Moreover, other studies reported that higher stage tumors are related to significantly higher rates of positive surgical margins. Since the most of the patients in this study were assigned to T2 clinical stage, if a greater portion of the patients were with higher stages, the outcomes of surgical margins also might be changed. There are a few limitations in this study and the retrospective study design is one of those. Due to the retrospective design of the study, no randomization of the patients was applied so that relatively lower comorbidities were associated with the patients. Moreover, since a single surgeon performed all the operations in this study, there might be also some contributions of the learning curves in the early RALP cases. The follow up period was relatively short term as we mainly focused on evaluating the early postoperative outcomes. Thus, a longer follow up period should be taken in the further study.
Conclusions
In healthy elderly patients with lower cormobidities rates, early recovery of postoperative continence and urinary functions after RALP can be achieved by bladder neck preservation performed through lateral bladder neck dissection. However, bladder neck preservation showed negative impacts on positive surgical margins, but a further study still needed for the definite influence of bladder neck preservation on surgical margins to be made.
References
- Cooperberg MR, Broering JM, Carroll PR. Time trends and local variation in primary treatment of localized prostate cancer. J Clin Oncol 2010; 28: 1117-1123.
- Hu JC, Wang Q, Pashos CL, Lipsitz SR, Keating NL. Utilization and outcomes of minimally invasive radical prostatectomy. J Clin Oncol 2008; 26: 2278–2284.
- Choi WW, Freire MP, Soukup JR, Yin L, Lipsitz SR, Carvas F, et al. Nerve sparing technique and urinary control after robot assisted laparoscopic prostatectomy. World J Urol 2011; 29: 21-27.
- Peyromaure M, Ravery V, Boccon-Gibod L. The management of stress urinary incontinence after radical prostatectomy. BJU Int 2002; 90: 155- 161.
- Guillonneau B, el-Fettouh H, Baumert H, Cathelineau X, Doublet JD, Fromont G, et al. Laparoscopic radical prostatectomy: oncological evaluation after 1,000 cases a Montsouris Institute. J Urol 2003; 169: 1261- 1266.
- Siddiqui SA, Sengupta S, Slezak JM, Bergstralh EJ, Leibovich BC, Myers RP, et al. Impact of patient age at treatment on outcome following radical retropubic prostatectomy for prostate cancer. J Urol 2006; 175: 952-957.
- Korean National Population Statistics. Accessed March, 23, 2016.
- Gomez CA, Soloway MS, Civantos F, Hachiya T. Bladder neck preservation and its impact on positive surgical margins during radical prostatectomy. Urology 1993; 42: 689-693.
- Latiff A: Preservation of bladder neck fibers in radical prostatectomy. Urology 1993; 41: 566-567.
- Ficarra V, Novara G, Artibani W, Cestari A, Galfano A, Graefen M, et al. Retropubic laparoscopic and robot-assisted radical prostatectomy: a systematic review and cumulative analysis of comparative studies. Eur Urol 2009; 55: 1037-1063.
- Freire MP, Weinberg AC, Lei Y, Soukup JR, Lipsitz SR, Prasad SM, et al. Anatomic bladder neck preservation during robotic-assisted laparoscopic radical prostatectomy: description of technique and outcomes. Eur Urol 2009; 56: 972-980.
- Rocco F, Carmignani L, Acquati P, Gadda F, Dell'Orto P, Rocco B, et al. Restoration of posterior aspect of rhabdosphincter shortens continence time after radical retropubic prostatectomy. J Urol 2006; 175: 2201-2206.
- Ahlering TE, Skarecky D, Lee D, Clayman RV. Successful transfer of open surgical skills to a laparoscopic environment using a robotic interface: initial experience with laparoscopic radical prostatectomy. J Urol 2003; 170: 1738-1741.
- Deliveliotis C, Protogerou V, Alargof E, Varkarakis J. Radical prostatectomy: bladder neck preservation and puboprostatic ligament sparing effects on continence and positive margins. Urology 2002; 60: 855- 858.
- Lowe BA. Comparison of bladder neck preservation to bladder neck resection in maintaining postprostatectomy urinary continence. Urology 1996; 48: 889-893.
- Gaker DL, Steel BL. Radical prostatectomy with preservation of urinary continence: pathology and long-term results. J Urol 2004; 172: 2549-2552.
- Willis DL, Gonzalgo ML, Brotzman M, Feng Z, Trock B, Su LM. Comparison of outcomes between pure laparoscopic vs. robot-assisted laparoscopic radical prostatectomy: a study of comparative effectiveness based upon validated quality of life outcomes. BJU Int 2012; 109: 898-905.
- Srougi M, Nesrallah LJ, Kauffmann JR, Nesrallah A, Leite KR. Urinary continence and pathological outcome after bladder neck preservation during radical retropubic prostatectomy: a randomized prospective trial. J Urol 2001; 165: 815–818.
- Katz R, Salomon L, Hoznek A, de la Taille A, Antiphon P, Abbou CC. Positive surgical margins in laparoscopic radical prostatectomy: the impact of apical dissection, bladder neck remodeling and nerve preservation. J Urol 2003; 169: 2049–2052.
- Aydin H, Tsuzuki T, Hernandez D, Walsh PC, Partin AW, Epstein JI. Positive proximal (bladder neck) margin at radical prostatectomy confers greater risk of biochemical progression. Urology 2004; 64: 551-555.
- Razi A, Yahyazadeh SR, Sedighi Gilani MA, Kazemeyni SM. Bladder neck preservation during radical retropubic prostatectomy and postoperative urinary continence. Urol J 2009; 6: 23-26.